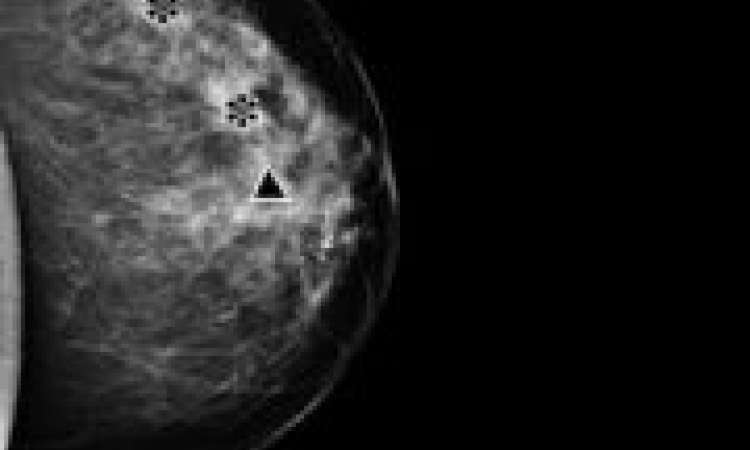
Quality assurance first
Germany's Federal Committee of Physicians and Statutory Health Insurance Funds set up three model projects, based in Bremen, Wiesbaden and Weser-Ems, to trial the third edition of the European guidelines on healthcare within the German system and to develop the necessary organisational structures to make these work.

Following negotiations over the ‘Model Project Mammographic Screening in Bremen’, between the Association of Statutory Health Insurance Physicians of the Hanseatic City of Bremen and the national associations of the statutory health insurance funds of the City of Bremen, Dr Hans Junkermann MD, of Heidelberg, was appointed project leader as there was no role model or similar project in any other German city mammographic screening in Bremen oriented itself on examples from the Netherlands, Sweden and England.
The objective was to create conditions to provide quality assured mammography and sufficient information for all women in Bremen aged 50-69 years. The objective of mammographic screening, according to the European guidelines, is to lower the mortality rate from breast cancer by about 30%. According to those guidelines, the main features of mammographic screening should be:
• Organised screening following written invitation to all women aged 50-69, based in the region
• Mammography to be carried out by a qualified radiography assistant who has undergone further training
• Second assessment of each mammographic examination, with both assessments being carried out by practicing radiologists, with further training, who evaluate at least 5,000 images annually
• Assessment based on EU guidelines
• Second diagnosis of all pathology results
• Complete, gapless documentation and publication of results
• Pre-and postoperative, interdisciplinary conferences with compulsory attendance
• Work flow and results based on EU standards
• Internal and external quality assurance
Every step in mammographic screening, from initial invitation to diagnosis, the documentation and possible further assessments right up to surgery (if necessary) must be carried out with quality assurance. Mammographic screening is a chain of events where each step, plus the whole procedure, must be totally quality assured.
Individual steps
• All women aged 50-69 should receive a written invitation to voluntarily participate in the programme. They can change appointments by phone, fax or email.
• Examinations are carried out in special facilities where specially trained radiography assistants work autonomously and self-dependently
• Each mammogram is assessed by two practicing radiographers, independently
• Any suspicious images are discussed and assessed with the doctor responsible for the project and patients are then recalled for further assessments
• Final diagnosis is carried out in the screening centre through clinical examination, ultrasound scan, additional mammography and, if indicated, biopsies
• All clinical, pathological and radiological results of patients examined are introduced to, and discussed by surgeons, radiologists and pathologists during multidisciplinary, pre-operative conferences. Results of surgery and courses of treatments are discussed during post-surgical meetings.
The model project in Bremen, the first to be set up, began in July 2001, followed soon afterwards by Wiesbaden, then by Weser-Ems just over a year later.
Up to 31/12/2001, a small number of women due for examination were invited on a daily basis, while the facilities for the clinical aspects of the mammographic screening (assessment, first and second pathology examination, stereotactic biopsy) were being set up. Simultaneously, further training was carried out for staff; guidelines for regular, ongoing training were developed, and external quality assurance was finalised with the reference centre in Nijmegen, Netherlands. Medical documentation programmes were selected and tested and the final data protection concept completed. Around this time, the Goetsche and Olsen’s Meta study was published by the Cochrane Institute, which took a clear stance against mammographic screening, causing confusion in Bremen as much as elsewhere.
Since 1/1/2002 Bremen’s mammographic screening unit has worked to full capacity. In May of that year, the WHO contradicted Goetsche and Olsen’s interpretation with the Lyon IARC (International Agency for Research on Cancer) statement and clarified: Quality assured mammographic screening reduces mortality rates from breast cancer by up to 35%. On one hand, this ended the emotionally heated discussion on disadvantages or benefits of mammographic screening. However, it also made it clear that only quality assured, organised mammographic screening lowers mortality, as opposed to the opportune (grey) type of screening, then widespread in Germany.
In October 2002, Germany’s National Cancer Institute published the ‘Shanghai-Study’, which declared that manual examination of the breast was not a suitable method for early detection of breast cancer. So, from a scientific point of view, only organised mammographic screening can be considered as a suitable tool of early detection that can lower mortality significantly.
In the first two years, 83,102 women across the three model project regions were invited for screening. 44,934 women from the target groups participated in mammographic screening. 6% of participants were recalled for further assessments. 2% of participants had tissue removed through needle biopsies. Breast cancer was discovered in more than 9 (9.6) in a 1,000 women, and in 17% of cases the cancer was still at the in situ stage. The proportion of invasive carcinomas of less than 10mm in diameter was 36%. There were no significant differences between the three model projects. With the exception of the participation rate, all EU guidelines were achieved or exceeded. Three times as many cases of breast cancer were detected in Bremen and Wiesbaden, with intensive medical care, compared with the period before the screening programme began.
Dealing with external quality assurance is a new and unusual concept in the German healthcare system and was initially considered to be limiting, strange and controlling by staff involved in the mammographic screening programme. However, today external quality assurance is regarded as a natural safeguard and a check on one’s own work to ensure efficiency, benefits and evidence.
Experiences gathered from the model projects provide the foundations for the national programme for quality assured mammographic screening, based on EU guidelines, which was recently adopted in Germany.
01.07.2004