Article • Prostate cancer detection
MRI tumour scans overlaid onto ultrasound
New medical software which overlays tumour information from MRI scans onto ultrasound images is helping to improve detection of prostate cancer by guiding surgeons as they conduct biopsies.
Report: Mark Nicholls
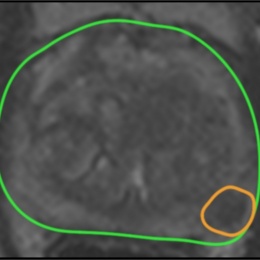
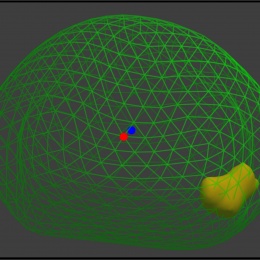
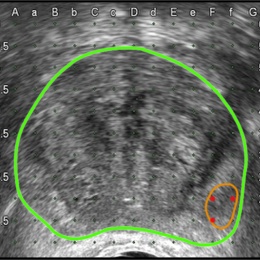
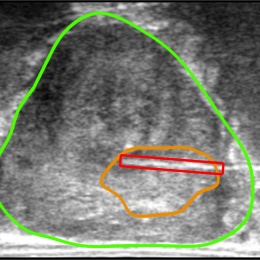
Developed at University College London (UCL), the software is deployed via a system called SmartTarget and embraces artificial intelligence (AI) to use both systems in tandem to enable surgeons to pick up clinically-relevant cancers missed when using visual detection methods. Whilst MRI-targeted biopsies have improved detection rates to almost 90% in recent years, the UCL team believe the SmartTarget system further enhances this by allowing a 3-D model of the prostate and cancer to be created for each patient from their MRI scans using advanced image processing and machine learning algorithms. Then, during biopsy, the model is fused with ultrasound images so that surgeons can target areas of concern.
In a recent study – funded by the UK Department of Health and Social Care and Wellcome Health Innovation Challenge Fund – 129 people with suspected prostate cancer underwent two biopsies – one using the SmartTarget system and one where surgeons could only visually review the MRI scans. The two strategies combined detected 93 clinically significant prostate cancers, with each picking up 80 of these cancers; each missed 13 that the other method picked up. As a result, the researchers report that visual reviews of MRI scans by surgeons should be used in tandem with SmartTarget because the technique enables surgeons to make subtle adjustments, such as adapting to the patient’s and prostate movement as the needle is inserted.

Co-senior author Dr Dean Barratt, at UCL Medical Physics & Biomedical Engineering and UCL Centre for Medical Image Computing, who invented the SmartTarget system, said: ‘We developed the system to equip surgeons with vital information about the size, shape and location of prostate tumours during a biopsy that is otherwise invisible on ultrasound images. The software provides a clear target. Because MRI-targeted biopsies require a very high degree of expertise and experience, we hope that the imagery displayed by SmartTarget will help to bring high accuracy prostate cancer diagnosis to a much wider range of patients and hospitals.'
'In essence, the software makes tumours that are otherwise invisible on ultrasound images, visible. This reduces the need for the surgeon to rely solely on a mental model of where a tumour is, which relies heavily on skill, experience, and the ability to visualise anatomy in three-dimensions,’ Barratt explained. ‘The result is increased confidence, which can be particularly important for urologists who have relatively little experience in the tumour-targeted biopsy technique. Benefits for patients also include increased confidence that, using the system, their surgeon can target a tumour accurately. Tumour targeting using MRI has been shown to be much more reliable than conventional biopsy methods and requires fewer needle insertions to make a diagnosis, resulting in a quicker, less-invasive procedure.’

The system, he added, also requires much less data on where the boundary of the prostate lies in the ultrasound images. Consequently, the surgeon does not need to use the software to define the entire boundary, leading to a much more streamlined clinical workflow without laborious interaction that is required with other systems.
The software has been commercialised by SmartTarget Ltd, a UCL spin-out company, and is already in use in several hospitals in the UK and USA. Co-senior author Professor Mark Emberton, Dean of UCL Faculty of Medical Sciences, said: ‘With this study we now have hard data showing that SmartTarget is as good as a group of experts in targeting tumours in the prostate, and have a glimpse of how clinicians and computers will be working together in the future.’
Profiles:
Dean Barratt is an Associate Professor in the Department of Medical Physics & Bioengineering at UCL, conducting research to develop software-based technologies to make data from diagnostic and/or surgical planning images available before a procedure, to be aligned with images obtained during the procedure to aid surgical navigation, particularly on developing image guidance methods that employ 3-D ultrasound imaging.
Mark Emberton is Professor of Interventional Oncology at UCL, an Honorary Consultant Urologist at University College Hospitals NHS Foundation Trust and Dean of UCL Faculty of Medical Sciences. His research aims to improve diagnostic and risk stratification tools and treatment strategies for prostate cancer, specialising in the implementation of new imaging techniques, nanotechnologies, bio-engineering materials and non-invasive treatment approaches.
26.02.2019