Article • MRI/US-Fusion
Munich medical duo refine biopsy teamwork
Ultrasound biopsy is rather unreliable to detect or exclude prostate cancer: many tumours are difficult – or impossible – to visualise sonographically and tissue sampling is haphazard rather than targeted.
Interview: Daniela Zimmermann
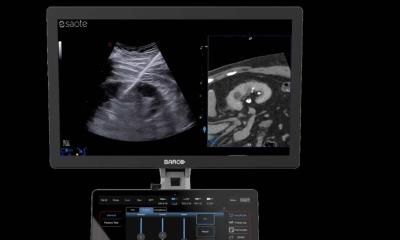
Now, a new technology offers relief. The fusion of MR images and real-time ultrasound allows the targeted biopsy of a prostate tumour and for the first time the examiner can precisely view the region of interest.
Due to technological progress during the past few years MRI today offers a high success rate in the early detection of prostate cancer. Several protocols that look at different parameters, such as perfusion, diffusion or contrast enhancement, provide a wealth of diagnostically relevant information. A so-called in-bore MR biopsy, however, is very time-consuming and resource-intensive: the patient is difficult to access and the magnetic field requires the use of special needles. In contrast, ultrasound is rapidly and easily available, yet the different echo patterns prevent reliable detection of prostate tumours, particularly when lesions are small. Fusion biopsy now combines the strengths of both imaging modalities by merging – fusing – pre-acquired MR images with ultrasound images in real-time.
Image fusion, as such, is not a new technology but has already proved its mettle in various other applications: for about ten years this has been used in abdominal imaging to reliably visualise liver, kidneys and vasculature and to differentiate pathologies.
Urologists have the patients, we have the imaging systems

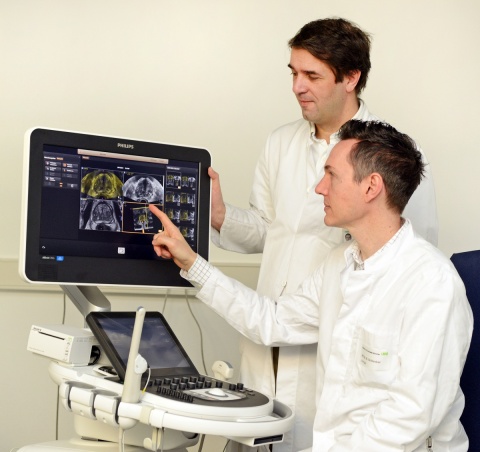
Ever since image fusion was introduced at the University Hospital Munich, the radiology and urology departments have been cooperating closely. ‘We realised, pretty much right away, that both parties would benefit from a cooperation,’ says Professor Dirk-André Clevert of the Institute of Clinical Radiology, who heads the Interdisciplinary Ultrasound Centre at his institution. ‘Urologists have the patients; we have the imaging systems. Together we can offer better diagnostics and treatment – in terms of patient-focus and science.’
His colleague Dr Boris Schlenker, at the Urological Clinic and Polyclinic, who coordinates the Interdisciplinary Prostate Centre in Munich, adds: ‘There was no apprehension whatsoever. With both of us working at a large university hospital we are used to cooperating across disciplines.’ Today the two specialists are an experienced team, which smoothly performs the combined MRI/ultrasound procedures in the operating room (OR). While radiologist Clevert focuses on getting the most out of the images and finding the best possible biopsy path, urologist Schlenker can concentrate on moving the biopsy needle.
Initially, physical and technological issues prevented the fusion technology from being applied to the prostate but the development of a specialised transducer and accompanying software cleared the path for use with transrectal ultrasound (TRUS).
Clevert explains the procedure: ‘In a first step, we have loaded the MRI images onto the ultrasound system and then we mark the regions of interest on these images. During the actual ultrasound exam, the MR images are superimposed on the TRUS images. As soon as the images are synchronised and registered, you can move the transducer through the MR images in the same way you’d move a computer mouse through an animated sequence. The MRI markers are virtually displayed on the TRUS images.’

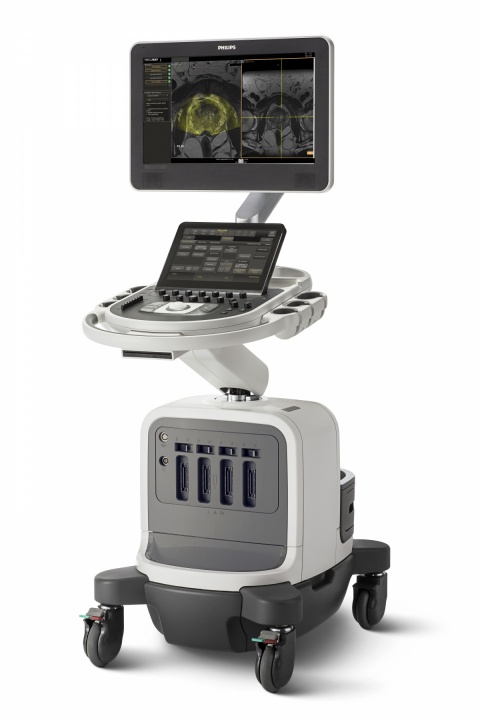
The two physicians use a Philips Affiniti system with its major advantage, speed, as Schlenker reports: ‘Most other systems require extensive acquisition of volume data sets. That means you need to acquire MR images of ten to twelve prostate slices and then do the same with your ultrasound system. Thus, the preparation of the data volumes takes quite a bit of time. In the new system fusion is done by plane. Instead of having to circle the prostate many times, fusion is now done by a single click.’
Clevert agrees: ‘The number of buttons to be hit to get to your results was reduced to the absolute minimum. Today, we do a fused prostate biopsy in somewhere between five and ten minutes.’
The current German S3 guideline on prostate cancer requires MRI only for patients who previously underwent one or more negative biopsies, but where a malignant prostate tumour continues to be suspected.
The standard for primary diagnosis is randomised punch biopsy – a controversial procedure. In a punch biopsy tissue samples are collected according to a certain pattern in order to cover as many prostate regions as possible. However, the punches themselves are done at random and thus offer limited diagnostic value. Particularly smaller early-stage tumours are frequently missed.
Many of today’s well-informed patients are not prepared to accept this uncertainty as Schlenker and Clevert can tell from their experience in the consultation room. More and more patients bring their own MR images to the clinic to have them used during prostate biopsy.
Fusion technology will become reality
While fusion technology is not yet considered in the guidelines, both interest in the new procedure and positive evidence are increasing. Several studies published in the past two years confirm the benefit of fusion technology in prostate cancer detection, such as a study comparing targeted fusion biopsy and 12-core biopsy [Siddiqui MM, Rais-Bahrami S, Truong H et al (2013); Eur Urol 64:713–719]. Among subjects, 320 out of 582 underwent standard biopsy with negative results, despite an elevated PSA level of 9.9 ng/ml. Additional fusion biopsy led to Gleason score upgrading in 81 of these subjects, which had major implications for the treatment strategy.
The two Munich experts in their different fields are confident that fusion technology will prevail. For them it is already a reality.
Profiles:
Dr Boris Schlenker is Ass. Professor of Urology. He is senior physician and faculty member at the Department of Urology, University Hospital Grosshadern, Ludwig-Maximilians University Munich, since 2013 and coordinator of the Interdisciplinary Prostate Centre, Munich. He is also a Fellow of the European Committee of Sexual Medicine (FECSM), Member of the German Board of Urology and Fellow of the European Board of Urology (FEBU).
Prof. Dirk-André Clevert began his medical career at the MRT-Diagnostik-Institut Westend in Berlin and the Department for Internal Medicine at Waldkrankenhaus Gransee. After a three-year residency in the Radiology Department at Passau Hospital, in 2003 the Berliner moved to Munich, heading the Interdisciplinary Ultrasound Centre – the focal point of all ultrasound activities in Munich University Hospital in Grosshadern – since the centre’s opening in 2004.
ECR - Don't miss
Saturday, March 5, 10:30–12:00 Room Z
Molecular Imaging
05.03.2016