Keep up-to-date with developments
Radiologists should know the indications for PET/CT scanning

In recent years PET/CT has proved a versatile and promising examination procedure, especially in oncology. Thus, according to Professor Christoph Eilles, head of the Nuclear Medicine Department at University Hospital Regensburg, ‘Radiologists should know the indications for carrying out PET/CT scans, be aware of what the procedure can deliver and when it makes sense to schedule or recommend such a scan.’ Also, although all indications are not yet known, because their number has grown continuously it is important that radiologists keep abreast of developments.
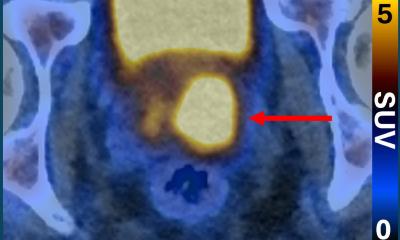
An important prerequisite to be able to assess PET data is radiologists’ knowledge of metabolic processes and opportunities for different tracers. ‘There are different substances, although currently only the FDG tracer is licensed, which delivers information about the glucose metabolism – ideal for imaging most tumours,’ he points out. There are, however, also tumour entities that need different tracers, e.g. prostate cancer where Choline is used, or brain tumours where Tyrosine is utilised. For some problems PET/CT is now regarded as the procedure of choice, e.g. for staging bronchial carcinoma. ‘If the radiologist discovers this type of tumour PET/CT is the best procedure to deliver an overview of the extent to which the cancer has spread in the body,’ he explains. The procedure is also very important as a follow-up examination for unclear diagnoses. Here PET/CT can be very helpful in achieving a differentiation between metastases, benign tumours and the presence of infections. As PET/CT is a different procedure to that of a radiological examination, the nuclear medicine specialist must always be informed about medication and previous treatment.
Dynamic processes must also be considered, such as the behaviour of the tracer over time. ‘Time can play an essential role, for instance in the differentiation between a radiation necrosis and tumour recurrence in the case of brain tumours, where it’s important to determine whether the tracer accumulates in the focal lesion or whether it is quickly excreted.’ For brain tumours the basic examination is an MRI scan, with images later fused with those of the PET/CT. ‘But, PET/CT can also initially be utilised pre-operatively as extensions of the brain tumour may not be visible on the MRI scan and the exact localisation of particularly malignant parts is particularly practicable with this procedure. This is of especial importance for a biopsy,’ he says, also adding his appreciation that PET/CT image data can be directly transferred into the radiation devices. Now, next to PET/CT are devices for a hybrid application of MRI and PET. ‘Whether or not this combination of the modalities in one machine will be as successful as that of the PET/CT, however, is still unclear and is currently being examined in studies. Anyhow, the separate MRI and PET images can be fused easily through software.
However, MRI/PET could be helpful for brain tumour diagnoses because PET/CT is mainly used for attenuation correction and the MRI for tissue imaging. With all other tumours, apart from the head, PET/ CT is used for localisation, often even together with a contrast medium examination in one process. Professor Eilles welcomes a rapprochement between radiologists and nuclear medicine specialists – facilitated by the use of the PET/CT, along with the formation of working groups by their specialist associations, and talk of a partly combined medical specialist training. ‘In Regensburg we already have some radiologists who spend a year with us in the department of nuclear medicine to learn how to better assess PET images. Beyond the question of which modality is the best procedure, it’s the experience and expertise of the person operating the machine that’s decisive.’
PROFILE
Trained in medicine at the Friedrich-Alexander University, Nuremberg-Erlangen Professor Christoph Eilles, in 1977 he gained a doctorate at the university’s Eye Clinic. Following his habilitation at the Julius-Maximilian University of Würzburg, in 1989 he received the Bavarian State Ministry teaching licence. In 1992 he became Professor of Nuclear Medicine at Regensburg University Hospital and, a month later, became head of the Department of Nuclear Medicine. Professor Eilles is a member of various specialist associations and on the advisory board of several publications.
02.11.2012