Article • Going nuclear
Ischaemia: Advances in nuclear imaging
Experts outlined approaches to ischaemia imaging during the recent British Cardiovascular Society conference. In a ‘Detection of ischaemia by cardiac imaging in 2018’ session, comparisons were made between solid state SPECT cameras, whether spatial resolution or visual assessment was of the greater importance, if CT-FFR offered advantages over CT perfusion, and the challenges in defining a gold standard of imaging ischaemia.
Report: Mark Nicholls

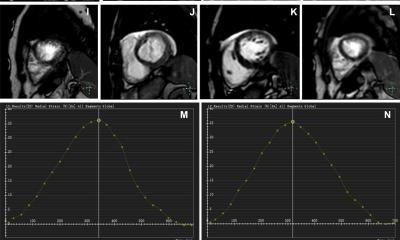
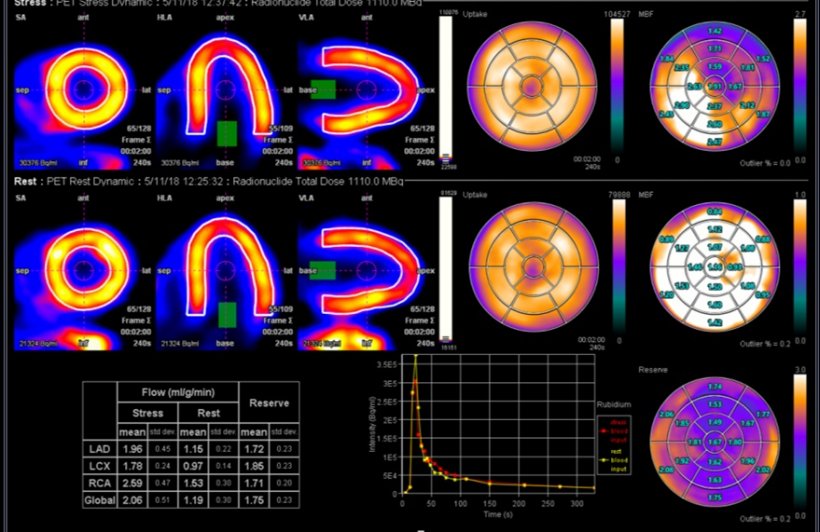
Discussing ‘Advances in nuclear ischaemic testing, from SPECT to PET and beyond’, Dr Kshama Wechalekar, who heads Nuclear medicine and PET at the Royal Brompton Hospital in London, and is President of the British Nuclear Cardiology Society (BNCS), told delegates that advances in nuclear imaging with solid state technology offered improved ability to detect ischaemia. ‘There is improved spatial resolution from multiple solid state CZT (Cadmium Zinc Telluride) detectors and therefore sensitivity is very high,’ she explained. ‘You can reduce the acquisition time at least by half with excellent quality and the equipment has a small footprint. The advantages of solid state detector cameras is that you can reduce the radiation dose by one third, have high sensitivity and resolution, an open design suitable for claustrophobic patients, and good image quality even in obese patients.’
SPECT, PET and CMR
The future of SPECT Nuclear cardiac imaging is in solid-state technology. Dynamic imaging, although technically challenging, can add value to MPI in the detection of ischaemia
Kshama Wechalekar
Recent studies have shown ability to do dynamic imaging offering potential in quantitative myocardial perfusion with SPECT, Wechalekar pointed out, adding that SPECT is less expensive than current PET and MRI. ‘The future of SPECT Nuclear cardiac imaging,’ she concluded, ‘is in solid-state technology. Dynamic imaging, although technically challenging, can add value to MPI in the detection of ischaemia. Whilst PET is the most accurate imaging technique for ischaemia assessment and prognosis, it remains expensive and less accessible.’ She also felt that the new tracer, Flurpiridaz, with results of phase III trials in the UK pending, might change the future of PET MPI.
One area of concern was how to persuade more people to train in nuclear cardiology with falling numbers in the field. ‘The BNCS Council is working hard to improve curriculum, organise level 1 and 2 training courses, and to identify centres that can offer nuclear cardiology training across the country that is easily accessible for trainees,’ she said.

Dr Chiara Bucciarelli-Ducci, Consultant Senior Lecturer in Cardiology/non Invasive Imaging Bristol Heart Institute, University of Bristol, explored the issue of quantitative versus visual assessment in CMR stress perfusion. She explained that stress CMR has been included in the ESC guidelines since 2014 (ESC revascularisation guidelines) based on evidence using visual assessment of ischaemia, rather than quantitative. Bucciarelli-Ducci discussed pros and cons of both visual and quantitative assessment, limitations and opportunities to increase spatial resolution, and very recent studies showing that there is no difference in diagnostic accuracy visual vs. quantitative. Quantitative perfusion is promising, but the acquisitions and analysis need simplification to meet the need of a busy clinical service. ‘CMR perfusion (visual) is a good clinical tool already,’ she concluded, ‘but can get better while quantitative CMR perfusion is evolving into faster and robust tools. While several methods are available, more in-vivo and clinical validation is needed with a number of studies in the pipeline.’
Function addition can improve specificity

Dr Marc Dweck, BHF Reader in Cardiology and Consultant Cardiologist at the University of Edinburgh and the Edinburgh Heart Centre, posed the question ‘CT-FFR/CT perfusion - neither or both?’ ‘CT Perfusion,’ he acknowledged, ‘is interesting, but I’m not sure how we are going to use it in clinical practice. With CT-FFR you get beautiful pictures, where you can look down the coronary arteries and see areas that are not getting enough blood. The advantage of this technique is that you can use it on a post-hoc basis, on scans where you are not sure if a lesion is obstructive or not, without any extra radiation or medication for the patient. This may be useful in lowering the rates of patients being sent to the cath lab following CT.’ Patients most likely to use CT-FFR, he added, are those with borderline lesions, though he stressed the key lies in a patient’s history and only using CT-FFR in patients with recalcitrant angina symptoms.
CT is a powerful imaging technique that informs about coronary artery anatomy (plaque burden, stenosis severity, plaque characteristics), he concluded, but emphasised that the addition of functional technique to the scan protocol can improve its specificity to identify obstructive stenosis, providing a comprehensive assessment of anatomy and function. With CT perfusion, radiation dose is increased, while CT-FFR has increased cost, though CT-FFR potentially fitted in better with patient workflows.

Professor Darrel Francis discussed the problems of computed tomography in the presentation ‘Ischaemia detection - are all our ideas completely wrong?’ Francis closed the session by pointing out that all previous speakers had described sensitivities and specificities, concepts that are meaningful only if ischaemia is dichotomous (present versus absent). His audience poll revealed cardiologists unanimously considered ischaemia to be a continuous gradation rather than dichotomous.
Profiles:
President of British Nuclear Cardiology Society Dr Kshama Wechalekar leads nuclear medicine and PET at the Royal Brompton Hospital in London, where she specialises in heart/lung nuclear imaging. Her main interests lie in using hybrid-imaging techniques, such as SPECT-CT and PET-CT, to improve understanding of pathophysiological processes affecting the heart and lungs. She has special interest in cardiac sarcoidosis and other inflammatory conditions of the heart.
Dr Chiara Bucciarelli-Ducci is Consultant Senior Lecturer in Cardiology/non Invasive Imaging at the Bristol Heart Institute, University of Bristol, and co-Director of the Clinical Research and Imaging Centre (CRIC Bristol). She is currently one of the vice-presidents and chair of cardiac MRI of the European Association of Cardiovascular Imaging (EACVI).
Professor Darrel Francis is Professor of Cardiology, Imperial College London. His work in ischaemia has included the ORBITA trial of revascularisation and the BRAVO trial of automated haemodynamic optimisation of cardiac resynchronisation therapy pacemakers.
Dr Marc Dweck is Senior Lecturer and Consultant Cardiologist at the University of Edinburgh and the Edinburgh Heart Centre. A British Heart Foundation Intermediate Clinical Research Fellow, he is a keen advocate of multi-modality cardiovascular imaging and is trained in echocardigraphy, carotid ultrasound, computed tomography (CT), cardiovascular magnetic resonance (CMR), PET/CT and PET/MR imaging.
26.08.2018