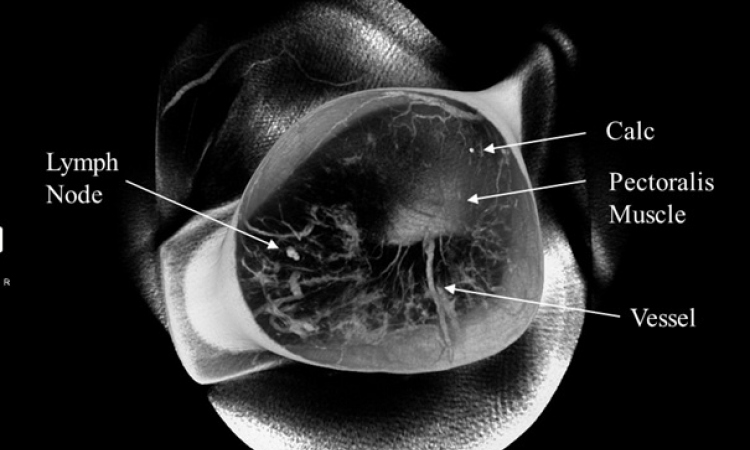
Integrated diagnostics and therapy in oncology
International Congress topics bridge the gap between science, hospitals and innovations
Cancer imaging is one of the most promising medical fields. Hybrid technologies, such as PET/CT or future MRI/PET, are the tools radiologists and oncologists use to gain ever deeper insights into the biological characteristics of tumours. During the Medica Congress the Integrated diagnostics and therapy in oncology imaging session (Thursday 19 November) innovative tools and related developments in their use will be aired.
Professor Hans-Ulrich Kauczor, Medical Director of the Radiology Clinic of the Department for Diagnostic and Interventional Radiology at the University of Heidelberg, who will chair the session, explained in an EH@Medica 2009 interview, why this event should prove invaluable for those working in oncology.
One of the reasons that the Integrated diagnostics and therapy in oncology session is important, ‘…is its close link between application and product, i.e. the transfer of knowledge in connection with the accompanying exhibition. And for me as a clinical radiologist the concept of broadening my horizon through a look at the medical industry is also exciting,’ said Prof. Kauczor. ‘A further aspect plays a particularly important part in the field of oncological imaging: We want to convey the innovations in medical technology and their importance for science and hospitals; that is, we want to point towards the potentials of developments in medical technology and the respective trends these will result in for future Medica exhibitions.’
Although Medica visitors cannot actually see the most exciting developments, such as PET-CT or MRI-PET, the professor pointed out: ‘Oncological imaging is not exclusively dependent on large equipment. Although this plays an important part, there have also been developments of smaller, more manageable products that visitors can find out about at the exhibition, today or in the future. One example is image-guided tumour therapy, which Professor Thomas Helmberger will discuss during the session. The necessary software, navigational aids or robots - all of these can be found at the exhibition. The same goes for preventive oncology, which Dr Christoph Herborn will talk about.
‘There are tools that could improve the significance of imaging in the future and thus make it more cost efficient. In the first instance I’m thinking about laboratory tests, or simple clinical tests that determine the probability of an oncological disease. We can achieve much higher validity for the relatively expensive imaging examinations with the help of these tests because they help us to utilise the modalities in more purposeful ways. These concepts already exist in the case of a breast cancer: A genetic disposition combined with positive BCRA1 or BCRA3 levels signals a strongly increased risk of developing breast cancer and therefore the need for an MRI mammography. There are similar developments for other medical indications.’
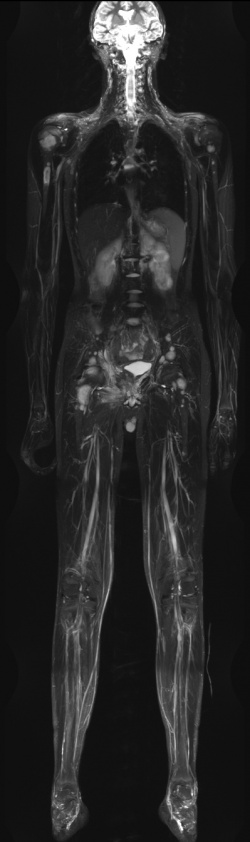
What does he consider the most important trends in cancer imaging? ‘Oncological imaging of the future will have two components. One is the diagnosis of cancer spread across the entire body. The other will be the functional-molecular, i.e. tumour-biological characterisation. This will probably be concentrated around the location of the primary manifestation of tumourous disease, with the objective of developing individualised therapy and evaluating the therapy response. Modern therapy management consists of a mix, a so-called sandwich therapy: Initially, neo-adjuvant, immunomodulating or anti-angiogenetic medication is used, then radiotherapy, possibly followed by a heavy ion boost.
‘We already have therapy concepts that begin neo-adjuvantly and where PET is then used to control to what extent the glucose metabolism decreases. If a level falls below a certain value we operate. If the tumour doesn’t respond we immediately utilise radiotherapy.
‘There are approaches entailing the use of different pre-operative radiotherapies, some of which currently do not yet have a truly curative dose, but only a pre-saturation to “scare” the tumour and to operate even if vital cells are still there. These schemata for certain tumour entities show that the future has already begun.’
18.11.2009