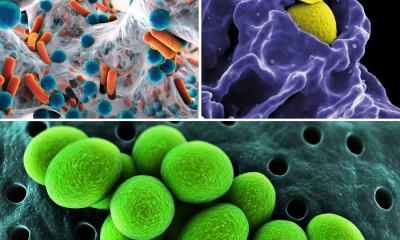
Sponsored • Orthopaedics
The fragile patient in arthroplasty: Sustainably lower risk of infection in hip fractures
Arthroplasty treatment of fragile patients is a major challenge faced by orthopaedic surgeons. The patients, often geriatric, come with a variety of risk factors and comorbidities that can negatively impact the success of an arthroplasty procedure.
Fragile patients are frequently geriatric cases that are characterised by an increased risk of intra- and postoperative complications such as periprosthetic fractures, infections, luxation and revisions. Along with advanced age, these patients come with a range of comorbidities, the most significant of which is osteoporosis, one of the main risk factors for fractures. A weakened immune system, anaemia, chronic diseases such as diabetes, cardiovascular diseases, malnutrition and even previous surgical procedures are other potential risk factors. Intra- and postoperative complications can therefore occur quite often. Because not all risk factors can be optimised before surgery, fragile patients require particular pre-, peri- and postoperative care with major surgical procedures such as hip arthroplasty, primary joint replacement and especially fracture treatment.
Treating femoral neck fractures: Hemiarthroplasty – a good option for fragile patients
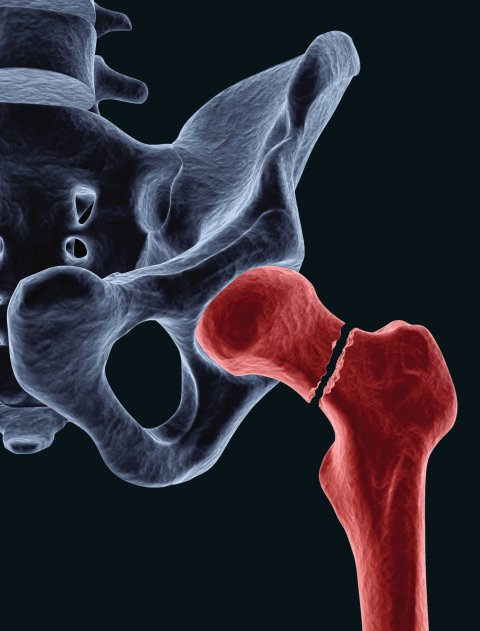
Image source: iStock/Raycat
Hip fractures such as proximal femoral fractures (femoral neck fractures) occur frequently in this patient group as a result of a fall, often facilitated by osteoporosis and other comorbidities. These are severe injuries that must be taken seriously and require prompt surgical treatment. Along with the surgical treatment itself to restore the mobility of the patient, it is essential to prevent postoperative complications that can occur at a higher rate in this patient group. Targeted rehabilitation measures are also important so that patients recover quickly and regain their mobility after a hip fracture. For patients with limited mobility, poor general health and limited life expectancy, hemiarthroplasty (HA) is a good option after a femoral neck fracture. The advantages of an HA are the short duration of surgery and rapid mobilisation after surgery with good clinical, functional, and radiological outcomes.
Infection prevention: Essential when treating femoral fractures
Just as for primary arthroplasty procedures, periprosthetic joint infection (PJI) is a rare but devastating postoperative complication that can occur more often with proximal femoral fractures than with elective procedures.
Treatment of a PJI, particularly in polymorbid patients, is associated with high mortality and a high rate of complications. The 1-year mortality for older patients with a femoral neck fracture is twice as high as the control group of the same age with no fracture. There are also reports of 1-year mortality rates of up to 50%. Affected patients often have a complex individual risk profile that must be taken into account. Experts point out that the success rate decreases the more local and systemic risk factors there are.
Infection therapy is also associated with high costs and leads to financial losses for hospitals. Prevention should therefore be the highest priority.
Recommended article
Sponsored • PJI risk mitigation
Arthroplasty: Avoiding infection and revisions in high-risk patients
The main goal of arthroplasty is to relieve pain, improve and restore joint function and recover quality of life. Periprosthetic joint infection remains a complication that has to be taken seriously.
Comprehensive package of measures for infection prevention
For effective infection prophylaxis with arthroplasty treatment of fragile patients, a package comprising a range of measures should be considered. The use of bone cement containing antibiotics to help prevent serious deep infections can form part of such a package. Evidence shows that when treating femoral neck fractures with hemiarthroplasty with dual antibiotic loaded bone cement, the risk of PJI can be lowered by up to 69% compared to a low-dose, single antibiotic loaded bone cement. In some clinics in Germany, the use of dual loaded antibiotic bone cement has become standard for arthroplasty procedures in geriatric patients to avoid potential periprosthetic complications.
Source: Heraeus
05.09.2022