HDTV advances into Germany
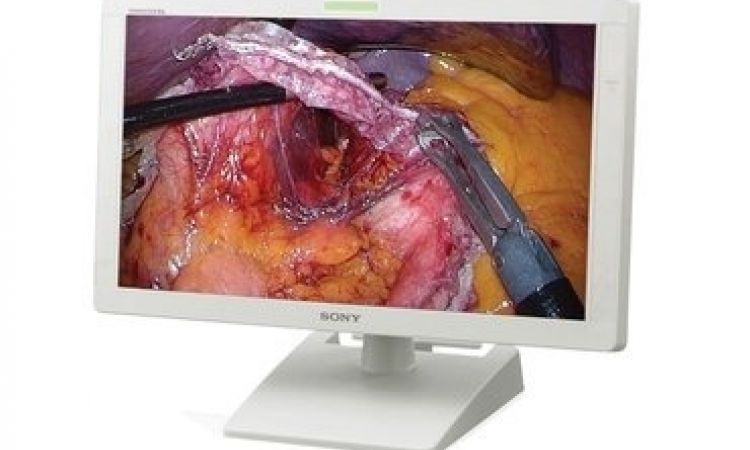
About a year ago, gastroenterologist Professor Horst Neuhaus began to use a high definition TV (HDTV) system as an aid in the endoscopic procedures carried out at Dusseldorf's Evangelisches Krankenhaus, in the Medical Clinic and Reference Centre for Endoscopy, of which he is head.

An HDTV system has also been used for about the same period at the Visceral, Vascular and Thoracic Surgery department in the Markus Hospital, Frankfurt. ‘One of the main advantages of minimally invasive surgery (MIS) – with or without HDTV – is that there is a much better view of the operating field via the monitor,’ Prof. Karl-Hermann Fuchs, Head of the Clinic told us.
Explaining the HDTV system to Denise Hennig of European Hospital, Prof. Neuhaus said that, up to now, PAL technology (with the 690 lines of a television set) was used for endoscopy. However, with 1,080 lines, HDTV technology increases image resolution fourfold. ‘This improved resolution can be subjectively seen on the flat screen monitors,’ he said. ‘Mucous structures and possible changes can be differentiated much better. We are more sensitive to the detection of the slightest changes, which we wouldn’t have been able to notice before. We are able to get much closer to where we need to be and can, if necessary, intervene with minimally invasive procedures (MIS) straight away. A further advantage of the new camera system is narrow band imaging (NBI), which was introduced by Olympus around the time that HDTV technology was introduced.’
NBI, Prof. Neuhaus explained, is a procedure that emphasises the colours blue and green within the colour spectrum. ‘These have short wave lengths that penetrate tissue to a lesser extent. Haemoglobin, for example, also absorbs within the short wave range at around 460 nanometers. NBI technology helps to blank out the red colour range completely, as if we were using a filter. This colour-changed imaging allows us to characterise the mucous membrane structures in much more detail and also to detect subtle tissue changes. When we detect a change in the mucous membranes using conventional, white light endoscopy, which comprises the entire colour spectrum, we need to use chromo-endoscopy (endoscopy involving the topical application, i.e. spraying on, of chemical agents (colour stains) to improve tissue characterisation) to establish a differentiated diagnosis between infected and neoplastic tissue. However, in reality, this wasn’t often done. These days we can just press a button to switch on the NBI system and can immediately differentiate changes in mucous membranes, differentiate any lesions from their surroundings and detect tissue changes much better.’
In this case, he foresees the end of the use of chemical agents. ‘There’s a range of studies, on Barrett’s oesophagus, for example, which show that NBI is just as good as chromo-endoscopy. As far as I know there are no comparable studies for the colon, but from the clinical point of view the situation here seems similar. As we no longer have to use chromo-endoscopy, the differentiation between harmless benign and infected, suspicious tissue can be achieved much quicker. However, in a way there is a chance that this gain in time might be cancelled out by HDTV technology, because this allows us to see far more detail, which means that we may spend more time characterising the area we are examining and also possibly taking tissue samples.’
Are there technical improvements he would like to see? ‘HDTV and NBI should be at the disposal of all endoscopists. First, we have the primary problem that we cannot find enough cases with early changes. On the one hand it’s because people might not even go to their doctors or, on the other, because conventional technology has not enabled us to detect these early changes, or we have overlooked them. However, if in doubt, the doctor should consult a reference centre for endoscopy.
‘In terms of early stage cancer treatment, I imagine there will be further, technical improvements. Currently, it is still very complex to remove larger areas with endoscopic mucosal resection, or with the submucosal dissection introduced by the Japanese,’ he pointed out. ‘We are working on systems that will allow us to significantly speed up the cutting procedures, or which will allow us to carry out whole wall resections endoscopically. We don’t yet have sufficiently evaluated surgical staplers, or suture procedures, used for flexible endoscopy. However, we are confident that - particularly in view of the new MIS procedure NOTES (Natural Orifice Transluminal Endoscopic Surgery) - these instruments will be significantly improved. It’s now up to the medical industry.’
Visceral, vascular and thoracic surgery
‘In MIS we get an enlarged view of the operating field via the monitor,’ said Prof. Karl-Hermann Fuchs, at the Markus Hospital. ‘This gives us a far more precise view than we sometimes get with open surgery – particularly in areas that are difficult to access, such as the oesophagus or deep rectum.
‘HDTV technology adds an extra advantage to this, because even more precise images are created. It allows us to see nerve structures, small vessels and the entire anatomy in much more detail. A further technical advantage within this system is narrow-band imaging, which allows us to define the borders of tumours far more precisely.’
Another advantage is that the system appears to remove some of the strain and fatigue for surgeons, who must concentrate for hours in front of a monitor in the operating theatre. ‘This is just a purely subjective experience,’ he added. ‘It has not yet been scientifically proven. However, I’m sure this technology will establish itself over the next few years, and then we will get studies that record and document these advantages in figures.’
Asked what improvements he would value most in such a system, the professor said he did not have sufficient technical knowledge to come up with suggestions. ‘That’s a job for engineers,’ he pointed out, and reiterated: ‘All I can say is that we get a better image, which is great as it makes our work a lot easier. This not only applies to tumour removal, or organ resections, but also any other surgical procedures; it makes preparation easier because the improved image achieved via the monitor is often more precise than what we can see with our bare eyes in open surgery.
‘Improved imaging also opens up new perspectives in flexible endoscopy. We are currently developing a new operating procedure called NOTES (Natural Orifice Transluminal Endoscopic Surgery), which is groundbreaking in MIS. The method utilises natural body orifices as entry channels. Once access has been gained in this way only a small incision is then required to access the operating field. In April, the gallbladder of a patient in Strasbourg was successfully removed transvaginally. This kind of surgery is in its infancy, but will definitely become important as a further means of access for MIS.
Working together
‘Flexible endoscopists and surgeons are slowly beginning to work together,’ pointed out Professor Fuchs. ‘I had the advantage of having learned flexible endoscopy and also the other, open and laparoscopic surgical procedures from the beginning, and I’ve been practising them for 25 years. That’s why I can judge that these medical fields belong together. The fact that endoscopists, gastroenterologists and visceral surgeons work closer together is a positive development. We can all learn and benefit from one another.’
25.06.2007