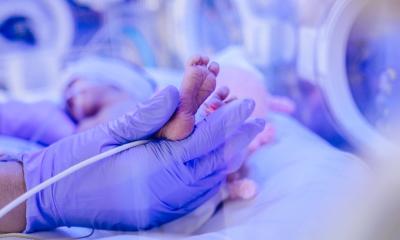
Giving the tiniest patients a chance
‘An environment that promotes development improves the survival chances of premature babies’
The number of premature births increases continuously in all European countries – with the exception of Sweden. Every year around 500,000 children – every 10th baby – in Europe are premature, i.e. born before the end of the 37th week of pregnancy and with a birth weight below 2,500g.
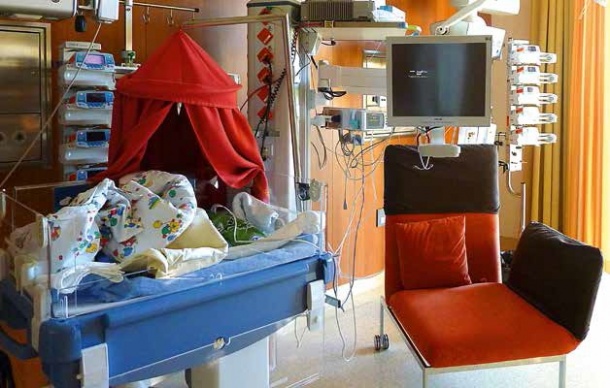
Along with these ‘near term babies’, the number of ‘extremely low birth weight infants’, who can now survive from the 24th week of pregnancy, has also been increasing. However, premature babies are at risk of future health problems.
At a symposium held by Dräger during the 108th Annual Congress of the German Society of Paediatrics and Adolescent Medicine experts explained how the neonatal ward environment and parental involvement can positively impact on the neurological development and growth of a baby’s brain. Since its inception in 2008, the European Foundation for the Care of Newborn Infants (EFCNI) has lobbied for the causes of newborn and premature infants and their parents. For Silke Mader, founder member and chairwoman of the foundation, the promotion of better neonatal care is something very close to her heart as much as it is a purpose. Based on her own experience of giving birth prematurely she is raising awareness of this topic amongst the public and even with the European Parliament. The benchmarking report compiled by the foundation in 2010, which compares neonatal standards across Europe, uncovered alarming differences and a north-south divide. The EFCNI White Paper on Maternal and Newborn Health and Aftercare Services: Caring for Tomorrow, published last year, based on the findings of this report, is the first evidence-based paper to substantiate demands for improved care of pregnant women and newborns. The fact is that, so far, there are no unified standards across the EU, no standardised documentation systems and no obligatory hygiene guidelines for the care of newborns. This leads to very different quality standards and outcomes for those affected. The main demand is the implementation of family-orientated care, parents’ rights are not acknowledged in many countries: ‘Instead of viewing them as the guarantors of the children’s wellbeing, they are often treated as guests on the special care baby unit,’ says Silke Mader. The foundation is also lobbying for high, unified standards for the care of children and for the working conditions for staff.
Oliver Hantke, Architect for the Federal Association ‘The Premature Baby’ e.V. is currently developing a website (www.neoträume.com) that will from 2013 provide inspiration for the professional design of neonatal intensive care units. Based on the premise that ‘everything revolves around the child’ he is introducing building blocks for the design of the different areas on the ward, ranging from the patient area with a protected environment for babies and parents via a buffer zone to a zone with a normal, adult-appropriate environment. Professional groups have defined ideal case standards for this purpose. Apart from conceptional approaches, examples of recently built or refurbished wards are to inspire the viewers’ imagination and also to show decision makers what can actually be achieved. Neoträume considers itself as an open-ended, continuous project and a place to record dreams and wishes.
Care concept with parents
Dr. Erna Hattinger-Jürgenssen, Consultant at the Neonatology Centre of the University Hospital Salzburg, spoke of her experiences with the implementation of a type of environment and care that promote the development of premature infants, the first ward of this kind in German speaking countries. She was no longer content with the fact that, whilst physical closeness between parents and newborns is now considered to be a matter of course, it is often not possible to realise this for premature babies due to various technological limitations. After a planning stage lasting seven years, two years’ building and overcoming many prejudices, the Parent-Child-Centre and Perinatal Centre opened in Salzburg in June 2010. Based on Scandinavian ward designs, parents are automatically integrated into the care concept. A maximum of two incubators are in a sufficiently large room, with comfortable beds, along with five parentchildren rooms to enable parents to carry out frequent, long sessions of ‘kangaroo care’, i.e. direct skin-to-skin contact with their babies. Families also have a lounge and respite area on the ward in the immediate vicinity of the intensive care ward, with bedrooms, kitchen and play area for siblings. The design of the egg-shaped new building incorporates the latest findings on noise and light reduction. According to Dr Hattinger- Jürgenssen, the objective of optimum care for premature babies is to continue the neurological development begun before birth, within the context of intensive care medicine. This obviously cannot be identical, but the differences compared to development in the womb should be kept as little as possible. Silke Bahr, Marketing Manager Neonatology for Central Europe at Dräger introduced the technical opportunities that can help achieve an environment that promotes development. Apart from a lighting concept based mainly on indirect lighting, the noise level can also be monitored with the help of a noise-display. If noise levels around the incubator rise too much, an ‘ear’ lights up in red and visually alerts for noise reduction.
Improved incubators
The incubator design has also undergone many improvements in recent years. Dräger incubators can be closed quietly, the motor supplying warm air runs on as quiet a noiselevel as possible and light from the monitors is minimised via a daynight mode setting. Potential false alarms during Kangaroo care sessions, which stress babies and parents, can be excluded. Customers can see 3-D visualisations when planning the design of a neonatal ICU. At the Dräger design centre in Lübeck the entire plan can be reconstructed true to scale and inspected for evaluation.
PROFILE
Silke Mader - After a premature birth and the demise of one of her twins, in 1999 the former nursery nurse became involved with the Parents Initiative ‘Unsere Frühchen’ (Our Preemies) in Munich. In 2003 she became the organisation’s Federal Chair and, in 2006, its Executive Chairwoman. Two years later she was a founding member of the European Foundation for the Care of Newborn Infants (EFCNI). Silke Bahr is still its Executive Chair.
Erna Hattinger-Jurgenssen MD - Gaining a medical degree in Vienna and Innsbruck, and then pursuing a specialty in paediatrics, in 2000 she became a consultant at the Neonatology Centre Salzburg and a senior consultant in 2005, frequently deputising at the Centre. To a large extent the Centre is the result of her efforts and bears her marks. In addition to her clinical work she founded the association ‘früh-R-leben’ (literally ‘live- and experience - earlier’) for premature and newborn infants and their parents.
05.11.2012