Carotid Plaque Imaging
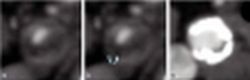
Ischaemic stroke accounts for 80-85% of all cerebrovascular accidents and causes considerable morbidity and mortality, thereby placing a significant burden on western societies. In the UK alone, stroke costs amount to 10.4 billion EUR annually. These events commonly are a consequence of systemic atherosclerotic disease and with the internal carotid arteries supplying 75% of cerebral blood flow, plaque formation in their extracranial segments is recognized as a frequent source of arterioarterial embolism, site of haemodynamically significant stenosis or even vessel occlusion, all potentially leading to disabling distal ischaemia. In large randomized landmark trials in Europe and the USA in 1991 the degree of luminal narrowing has been found to predict the likeliness of ischaemic events and, today, endarterectomy is well established as a surgical measure of secondary prevention of ischaemic stroke in cases of symptomatic high-grade stenosis since it was shown that it is more effective than medical management alone. Irrespectively, purely haemodynamic infarcts from severely narrowed carotid segments are actually much less frequent than their embolic counterparts, i.e. there is onlyamoderate correlation between the degree of stenosis and clinical events. Indeed, it has become evident from cardiological data that it is the atheromatous plaque itself which is the culprit lesion that defines most of the risk of ischaemic stroke since plaques are not a uniform and inert entity but have a certain dynamic. Intralesional processes are reflected in distinct histomorphological features and a classification of their nature has been put forward by The American Heart Association, revised and criticized.
This article was first published in the VISIONS, issue 11/2007, a publication of Toshiba Medical Systems
29.08.2007