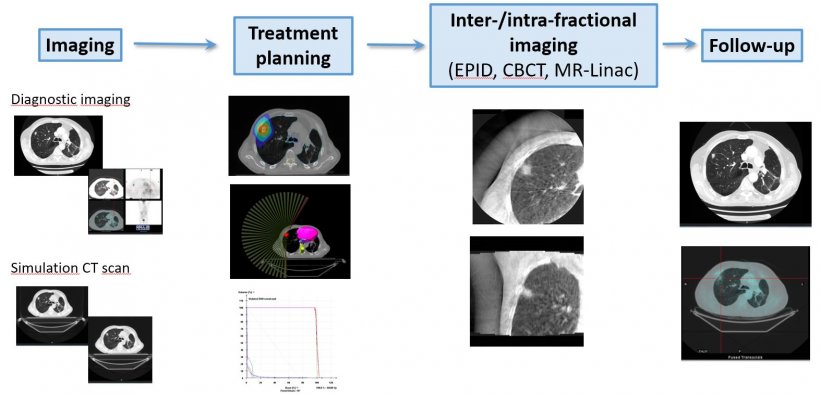
The whole workflow in radiotherapy is based on medical images, a potential source of information on tumour biology, on- and post-treatment tumour remission. AI will help to analyse these images and create decision support tools. CT - computer tomography; EPID - electronic portal imaging device; CBCT - cone beam computer tomography; MRI-linac - magnetic resonance imaging-based linear accelerator.
Article • Screening, early detection, treatment optimisation
AI techniques advancing oncology care
Cancer care and the treatment clinicians can offer patients is being increasingly enhanced by Artificial Intelligence (AI). The technology has a role in diagnosis, with algorithms trained to design and deliver patient care, can match patients to clinical trials they may benefit from, and even help predict outcomes and those at greatest risk.
Report: Mark Nicholls
The session, New Frontiers of AI and Data Analytics in Oncology at the online HIMSS21 European Health Conference, explored where AI and data analytics is having the greatest impact today: screening and early detection, auto-planning for radiotherapy, treatment optimisation, identification of new biomarkers and more.

Clinicians are constantly seeking new ways of developing and implementing innovative technologies to support transformation of cancer care delivery, with AI pivotal to that, said Dr Tufia Haddad. But while new drugs and treatments were being approved on a weekly basis, she emphasised that they were only relevant if oncologists and their teams were up-to-date with the advances to ensure the right drugs reached the right patients. “With this in mind,” she said, “we aim to develop clinical decision support tools for our oncologists to help them select the best care, whether it is a standard care treatment option, or a clinical trial opportunity.”
Her presentation “Improving Patient Health and Provider Efficiency with Advanced Clinical Decision Support Systems” highlighted how the Mayo Clinic in the United States was working with commercial partners to develop a clinical trial matching system that extracts information from electronic health records to ensure patients match the trial’s inclusion and exclusion criteria. “We use natural language processing and machine learning to train the system to identify patient tumour attributes in order to match inclusion and exclusion criteria in individual clinical trials,” said Dr Haddad, who is an Associate Professor of Oncology at the Mayo Clinic College of Medicine and Science, and a Consultant in the Department of Oncology.
This has the potential to allow us to better tailor our screening and prevention recommendations to patients and reduce morbidity and the cost of care as well
Tufia Haddad
Once brought into practice, there was an immediate and sustained impact in how the system allowed our providers to better understand the clinical trial opportunities. “Because they were doing it more efficiently,” she continued, “they had more time to spend counselling the patient about the potential benefits of participating in a clinical trial. We also saw a dramatic increase in our clinical trial accrual, both to our cancer specific study as well as our broad Phase I experimental cancer therapeutics programme as well.”
Another priority is to develop a model to better assess breast cancer risk. “I really believe that having AI-enabled advance clinical decision support systems can improve provider efficiency, engagement and effectiveness,” she said. “For cancer risk assessment, it can help us individualise risk with increased accuracy and, overall, this has the potential to allow us to better tailor our screening and prevention recommendations to patients and reduce morbidity and the cost of care as well.”

Professor Barbara Alicja Jereczek-Fossa, Associate Professor of Radiation Oncology at the University of Milan, Italy, and Head of the Radiotherapy Division at the European Institute of Oncology, Milan, outlined how radiation oncology has an essential role in cancer management, contributing to cure in about 40 per cent of all cancer patients. But with a huge amount of data to study to gain more knowledge on prognostic and predictive factors, AI is increasing in importance.
Her colleague Professor Matteo Pepa, a bioengineer working in her department on AI, highlighted how AI plays a role in the radiotherapy workflow steps of patient consultation, planning, image acquisition, segmentation, radiotherapy delivery and follow-up.

“AI can be used as a decision support tool for radiation oncology,” he said. “The radiation oncologists can put their mind to the best course of treatment before expending resources on lengthy a treatment planning process.”
With image acquisition, AI is utilised in synthetic image generation, CT artefacts reduction, and image quality improvement. Deep learning can help determine optimal radiation parameters, he said, and reduce planning time while improving the quality of images. “The last step is radiotherapy follow-up and AI and machine learning models have been proven to be successful in predicting outcome,” he added.
AI can be deployed to streamline workflows and support the radiologist in creating richer and more definitive reports that can translate into more informed clinical decisions with a higher diagnostic confidence
Mathias Goyen
The session also heard from Mathias Goyen, GE Healthcare’s Chief Medical Officer for Europe, with examples of where AI is streamlining radiology workflow, automating repetitive and tedious tasks to allow the radiologist to focus on core roles. He gave examples in breast and prostate cancer, where technology is offering support. “One challenge for clinicians regarding breast cancer is how to increase detection rates, how to reduce false positives and how to avoid unnecessary patient recalls,” said Professor Goyen. He outlined how a GE Healthcare workflow solution used deep learning that allows for advanced cancer detection, a significant improvement in workflow and delivered reding time reduction of almost 30 per cent. Another example was an AI-powered advance visualisation review and reporting tool for prostate MRI. “AI can be deployed to streamline workflows and support the radiologist in creating richer and more definitive reports that can translate into more informed clinical decisions with a higher diagnostic confidence,” he said.
Profiles:
Dr Tufia Haddad is an Associate Professor of Oncology at the Mayo Clinic College of Medicine and Science, Chair of Digital Health for the Department of Oncology, and serves as the Mayo Clinic Cancer Center Associate Director for Practice Innovation Platform. Her clinical practice and research are dedicated to breast cancer.
Professor Barbara Alicja Jereczek-Fossa is an Associate Professor of Radiation Oncology at the University of Milan and Head of the Department of Radiation Oncology at the IEO European Institute of Oncology IRCCS in Milan, Italy. Her main research and clinical interests include urological malignancies, breast cancer, combined modality approach, and high precision radiotherapy.
Professor Matteo Pepa is a Biomedical Engineer at the Division of Radiation Oncology and at the Radiomic Group of the IEO European Institute of Oncology IRCCS in Milan, Italy. He is also adjunct professor at the University of Milan and his areas of expertise include medical imaging, artificial intelligence, radiomics and radiation oncology.
15.07.2021