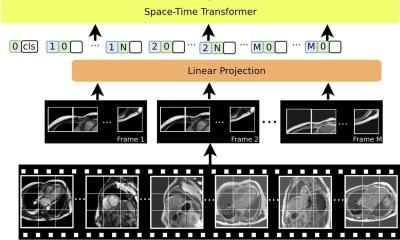
Image source: User Ksheka on en.wikipedia, Wolff-Parkinson-White syndrome 12 lead EKG, CC BY-SA 3.0
News • Merging modalities
AI combines ECG and X-ray to diagnose arrhythmic disorders
Kobe University Hospital’s Dr. Makoto Nishimori and Project Assistant Professor Kunihiko Kiuchi et al. (of the Division of Cardiovascular Medicine, Department of Internal Medicine) have developed an AI that uses multiple kinds of test data to predict the location of surplus pathways in the heart called ‘accessory pathways’, which cause the heart to beat irregularly.
In this study, the researchers were able to improve diagnosis accuracy by having the AI learn from two completely different types of test results - electrocardiography (ECG) data and X-ray images. They hope that this methodology can be applied to other disorders based upon the successful results of this research. The research results were published online in ‘Scientific Reports’.
Image source: Unsplash/Alexandru Acea
Wolff-Parkinson-White (WPW) is an arrhythmic disorder. Patients with WPW syndrome are born with surplus pathways inside their hearts called ‘accessory pathways’, which can cause tachycardia episodes where the pulse speeds up. Catheter ablation involves using a catheter to selectively cauterize accessory pathways and can completely cure this disorder. However, the success rate of catheter ablation varies depending on the location of the accessory pathways. Conventionally, a 12-lead ECG (i.e. a regular electrocardiography) has been used to predict accessory pathway location prior to treatment. However, this current method that relies solely on ECG is insufficiently accurate, which makes it difficult to give patients a full explanation that includes the success rate of treatment. This research study tried using AI to solve this problem.
The researchers used a methodology for teaching AI called deep learning. Deep learning involves entering the data for each patient and the corresponding answers into a program. By repeating this learning process, the program automatically becomes smarter. Using this methodology, the research group was able to present a solution to a previously unresolved problem, thus further promoting the application of AI to modern medicine.
Firstly, Dr. Nishimori’s team developed AI using only ECG data and compared its performance to previous methods. They conducted repeated learning where they gave the AI each patients’ ECG data and the accessory pathway location (i.e. the answer) in each case at the same time, successfully creating an AI with a higher accuracy rate than previous methods. However, the AI was unable to perform correct predictions every time from ECG data alone. The cause of this issue was thought to be that the ECG data is affected by the differences in size and position of each heart, therefore the ECG data did not match even when the location of the accessory pathway was the same. This problem was resolved by having the AI learn data, such as information on each heart’s size, from chest x-ray images at the same time (Figure below). By simultaneously learning both the pre-treatment ECG and X-ray image data, the AI was able to obtain the missing information and its diagnostic accuracy was significantly improved compared to when only ECG data was used.
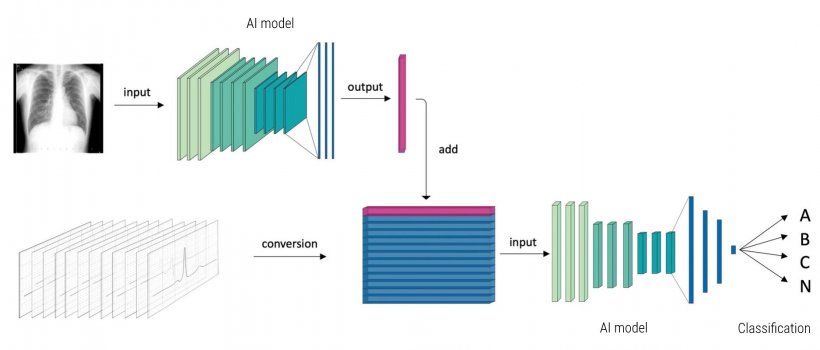
Image source: Kobe University (adapted from: Nishimori et al., Scientific Reports 2021 (CC BY 4.0))
The advancement of AI technology in recent years has made it possible for AI to make highly accurate diagnoses based on various kinds of test data in the field of medicine. However, there are cases where data from a single test is insufficient for AI to perform an accurate diagnosis. This research study successfully increased the accuracy by having the AI learn not only from ECG results but also from chest X-ray images, which are a completely different type of data. AI-mediated accurate diagnoses will enable doctors to give pre-treatment patients a more accurate explanation of their condition, which will hopefully put patients at ease. In addition, this research could be applied to various other disorders and will hopefully lead to the implementation of AI diagnosis software.
Source: Kobe University
22.04.2021