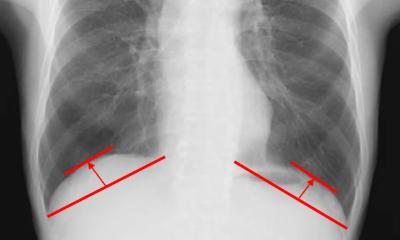
Against all odds: MRI does well in lung imaging
At first sight magnetic resonance imaging (MRI) does not seem to be particularly well suited for lung diagnostics: too much air, too much movement and too little water make image acquisition a real challenge. Nevertheless, MRI is useful and in certain cases even superior to CT say the members of HTIP (Heidelberg Thorax Imaging Plattform), an association of the radiology departments of the University Hospital Heidelberg, the German Cancer Research Center and the Thoraxklinik Heidelberg. The latter is a reference center for cystic fibrosis where lung imaging plays a crucial role, and PD Dr Michael Puderbach, Senior Consultant of the radiology department of Thoraxklinik explains the use and the advantages of MRI in paediatrics.

Dr Puderbach, MRI and lung imaging, that’s not a match made in heaven?
Puderbach: Indeed, at first sight anatomy and modality do not match well. The lung is the domain of computed tomography since MRI is a kind of water imaging: it looks at protons and protons are the water supplier in the body,
and there is little water in the lungs. The lung is a big sponge which, depending on the breathing situation, is up to 90 percent filled with air. Consequently there is little tissue to be imaged. This is the basic problem for MRI.
In addition, there are the breathing process and the heart which is a pulsating hollow organ. These two factors make image acquisition even more difficult. And finally there are the facts that the tissue transitions – from lung parenchyma to air – show immense differences in signal intensity which creates artifacts, and that the alveoli, little oxygen-filled bubbles, compromise the signal. These are major problems for MRI.
That does not sound particularly promising for meaningful diagnostics. Nevertheless you have been using MRI routinely in lung diagnostics for many years. What are the advantagesof this modality?
Puderbach: MRI technology has not stagnated. Sequences have become faster and faster which means we can bypass movement. There are different techniques – gating and triggering – to digitally stop heartbeat and breathing. The new developments allow us to visualize the lung on the one hand morphologically, which means MRI to a certain extent competes with CT, and on the other hand functionally. This is the major advantage of MRI: it offers possibilities to visualize function, such as perfusion. CT can do that as well albeit only with very high radiation exposure. And last but not the least MRI does provide functionalities the CT does not have at all. For us ventilation for example is very important.
How does that work: visualizing ventilation?
Puderbach: Firstly there is a rather complex procedure involving gas as contrast agent. In the past hyperpolarized helium 3 was used, an experimental gas that is difficult to handle. More recently xenon has appeared on the stage which is more readily available and easier to handle. However, for four years now we have applied a method that does not require gas at all but makes use of physiological processes such as breathing and heartbeat to visualize lung perfusion and ventilation. It is called FD MRI – Fourier decomposition MRI.
What’s so appealing about this method is the fact that the patient does not have to ‘do’ anything at all: no breath-hold, no belt around the body, no electrodes for triggering. The patient is in the scanner and can breathe freely. Moreover it is a rather fast procedure. We need about ten minutes to image ventilation and perfusion in an adult thorax. For children the examination takes five to ten minutes depending on the size of the thorax.
Where are the boundaries between MRI and CT?
Puderbach: We use MRI as standard imaging modality to assess pulmonary issues. Moreover all cystic fibrosis patients are scanned once a year. The CT is used to clarify unclear cases and obviously it is still the gold standard for example to visualize lung structures when the peripheral respiratory tract is involved. CT and MRI are complementary modalities and for each individual patient we have to decide which imaging method is best suited. This holds particularly true in paediatrics where you have a wide range of patients, from the three week old baby to the 18-year-old adolescent. While the latter has no problems being in the MRI scanner for half an hour, the baby needs to be sedated. Then you have to decide what is less harmful: sedation or radiation exposure in the CT.
Which field strength do you use?
Puderbach: We use 1.5 Tesla. Today 3 T is being used in many areas but 1.5 T is better for our particular purposes. Higher field strengths cause problems in the lung: artifacts in the transition between air and tissue are considerably increased when using 3 T. Lower field strength means more signal, thus theoretically one could even reduce to 0.7 T. However, lower field strength also means a weaker gradient system which is a disadvantage. As far as I am concerned, the ideal lung scanner would be a low field system with a strong gradient.
Where do you think lung imaging is heading for?
Puderbach: With technological developments being so fast these days I am sure much will happen both in MRI and in CT. I think MRI has to become faster and it has to somehow become breathing-independent because breathing-based procedures are stressful for the patient. In short: MRI has to aim towards faster examinations with free breathing. As far as functional imaging is concerned, I think the potential of ventilation and perfusion imaging is not yet fully exploited. FD or a similar technology without contrast agent and free breathing – that would be a major innovation.
Dr Puderbach, thank you very much for this interview.
25.06.2012