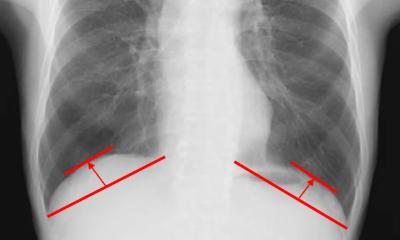
Ultrasound and the lung
Lung ultrasound is a technique with widespread uses and advantages in a range of areas from critical care through to less urgent medical areas. Most of all, it is of particular help in the rapid diagnosis of acute respiratory failure. During a session at WFUMB, its benefits and the latest techniques will be outlined by medical intensivist Dr Daniel Lichtenstein -- Lung Ultrasound in Acute Respiratory Failure.
Discussing areas where lung ultrasound can have clear benefits for the clinician and patient, Dr Daniel Lichtenstein explained: ‘Lung ultrasound is a standardised method that in a critical care setting allows the physician to answer most questions on acute respiratory failure. But, there are also advantages on less urgent questions, meaning it has a role not only in intensive care, but also in anaesthesiology, the emergency room, pulmonology, paediatrics, cardiology, thoracic surgery, family medicine, and polyvalent medicine through third world.’
Dr Lichtenstein, from Ambroise-Paré Hospital, Faculté Paris-Ouest, Paris, has conducted a number of studies to demonstrate the relevance of lung ultrasound in acute respiratory failure diagnosis and in the effective implementation of the protocols BLUE (Bedside Lung Ultrasound in Emergency) protocol and FALLS (Fluid Administration Limited by Lung Sonography).
There are, he said, a number of areas where lung ultrasound in acute respiratory failure is most effective. ‘These include knowing immediately the aetiology of an acute respiratory failure (BLUE-protocol); for immediately managing acute circulatory failure (FALLS-protocol); and for decreasing referrals to thoracic CT in an emergency.’
Ultrasound also has a use in broader settings in accident and emergency units and intensive care unit for medical or trauma problems. ‘Some examples include diagnosing acute haemodynamic pulmonary oedema, pneumothorax, and most cases of pneumonia and pulmonary embolism,’ he said.
Severe asthma or COPD, he added, is in the scope of the BLUE-protocol for a response in less than four minutes.
Since 1992, Dr Lichtenstein has written a number of books on whole body ultrasound with a critical focus on lung ultrasound, BLUE-protocol and derived uses. In many cases, he believes that the simpler forms of equipment are more effective for optimal use of lung ultrasound in the critically ill. ‘If a machine is too sophisticated, and not designed for the lung (by determination, or by hazard), the basis of lung ultrasound, that is real-time, respect of artifacts, natural image will be more difficult to find,’ he explained. ‘The simplest equipment is the best. I use a 1992 technology with a single microconvex probe for the whole body and no facility such as Doppler or harmonics.’
He believes for radiologists to use this technique effectively they need to have effective academic knowledge and training and recognise the importance and value of the method. During the session, he will offer advice on this.
Additionally he wanted to point out that a hospital also needs available trained physicians, on-site day and night, ready at short notice to respond to any acute situation.
"Lung ultrsound in acute respiratory failure", Friday, August 26, 11:00-11:25
Daniel Lichtenstein
Dr Daniel Lichtenstein is a medical intensivist at Ambroise-Paré Hospital, Faculté Paris-Ouest, Paris. Using training in both medical intensive care and ultrasound, since 1989 Professor Lichtenstein has developed the use of general ultrasound applied to the intensive care, in the hospital’s François Jardin’s medical ICU.
His many articles in international medical literature include 18 original articles and several reviews. His book L'Echographie Générale en Réanimation, published by Springer-Verlag in 1992, also became a fully reviewed version in 2002 (Translated into English 2005, title: General ultrasound in the critically ill, a sell-out, replaced by the 2010 edition Whole Body Ultrasonography in the Critically Ill.
A well-known lecturer and workshop leader at national and international congresses, he is also President of CEURF (Circle of Emergency Ultrasound for Re-animators of France, a non-profit association that aims to promote the use of ultrasound in general intensive care and emergency.
25.08.2011