Article • Bubble business
A transducer halts abdominal bleeding
Stopping abdominal wall bleeding with contrast-enhanced ultrasound was just one of the exciting developments in CEUS presented at the Bubble Conference 2017 in Chicago.
When you cut your finger you apply pressure to the wound until the bleeding stops. Professor Dirk-André Clevert from the Institute for Clinical Radiology at the Ludwig Maximilian University Hospital, Munich, Germany, remembered this simple remedy when seeking a non-invasive method to stop abdominal wall bleeding.
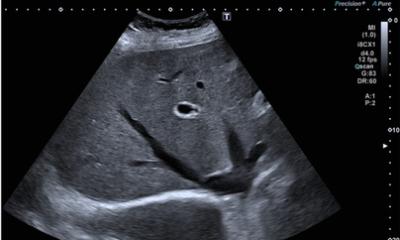
In a first step, the radiologist precisely locates the bleeding site with the help of fusion imaging, i.e. computed tomography and contrast-enhanced ultrasound (CEUS). Then, using the transducer, he applies pressure to the damaged vessel. Intermittent contrast medium injections enable him to check whether the bleeding continues. ‘In most cases, it stops within 30 minutes,’ Clevert underlines, adding,
The procedure was born out of necessity.
Dirk-André Clevert
‘The procedure was born out of necessity. The fact that vessels involved in abdominal wall bleedings tend to be very small, turning endovascular therapy into quite a challenge, and that access via the groin can be difficult in older and obese patients triggered the search for a new method to manage the bleeding. Clevert had used a similar pressure approach with false aneurysm in the groin post catheterisation. While the bleeding can indeed be stopped by applying constant pressure on the lesion, ‘the aneurysm procedure is more difficult since the groin vessel is much larger. The abdominal wall with its weaker perfusion presents itself for this technique.’ Penetration, however, is the limiting factor: ‘The closer the bleeding is to the surface the easier it is to stop. Deeper than five or six centimetres, it becomes rather difficult.’ Also, obviously if the bleeding is located behind a bone, the pressure technique won’t work either. ‘With soft tissue, it’s a very helpful procedure,’ Clevert reports. Since substantial physical strength is required the radiologist recommends upright standing during pressure application rather than sitting down: ‘Ideally, the patient couch is lowered so the transducer can be placed on the relevant site with arms outstretched.’ Professor Clevert presented this technique at the recent Bubble Conference 2017 in Chicago, the largest annual event in North America dedicated to new developments in contrast-enhanced ultrasound. The ‘bubble’ refers to gas-filled microbubbles used for contrast in CEUS. While the system has shown its value as a non-invasive, cost-efficient and radiation-free diagnostic imaging procedure, more recently CEUS has also revealed its treatment potential. In addition to Clevert’s new method to manage abdominal wall bleeding, a procedure was presented at the conference to briefly open the blood-brain barrier using contrastenhanced ultrasound. The oscillation of the microbubbles widens vessels just long enough to allow the bubbles to cross the blood-brain barrier. ‘If we manage to pack these bubbles with pharmaceuticals, the way we pack the trunk of our car, we can transport substances into the brain tissues in a targeted fashion,’ Clevert explains. In addition, the bubbles can be loaded with specific markers that inter alia dock onto VGF-2 receptors that are expressed during tumour angiogenesis – thus a high level of VGF-2 receptors is often associated with tumour growth.
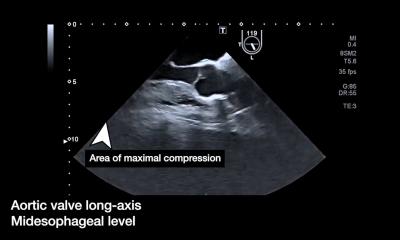
Myocardial imaging was another exciting feature at the conference. CEUS detects an infarction very early and enables a more precise prognosis of the extent of the cardiac event than catheterisation. Wall motion disorders and myocardial perfusion can be visualised better with contrast-enhanced ultrasound. Last but not least, technological developments were presented at the Bubbles Conference. Whilst a conventional ultrasound system produces a maximum of 60 frames per second during a dynamic study, new algorithms and different transmission and reception settings may well increase this number to 6,000 frames per second to significantly enhance image resolution. ‘The researchers in Chicago,’ Clevert confirmed, ‘demonstrated that bubbles can handle the stress created by such high frame rates.’
27.11.2017