What wounds tell us
Every day, patients are admitted to surgeries, hospitals and outpatient clinics with chronic wounds. Careful inspection gives a wound therapist clues to the appropriate primary care required even before further diagnostic procedures are carried out. So what do the clinical signs and symptoms tell us?
Report: Heidi Heinold
Wound surfaceNot all surfaces indicate wound infection. There are greasy white surfaces that are hard to detach from the wound and look like pus. However, this is actually fibrin that has to be removed when treating the wound but which is not a sign of bacterial colonisation or infection.
Bacterial colonisation is differentiated as follows:
Contamination: Bacteria are present in the wound but they are not multiplying. The granulation tissue appears rosy, the healing process is not affected, the typical wound smell does not develop; this appearance is also found in
Colonisation: Here the wound is colonised with germs which can multiply but the patient and wound healing are not yet affected. This is different in
Critical colonisation: In this state between colonisation and local infection there is increased exposure to bacteria. There are no obvious signs of healing and the first signs of infection are present. If granulation tissue is present it appears sensitive. There is an increased production of wound exudate, healing is delayed and pockets may develop as well as discolouration with surfaces that cause intensive, malodorous smells. Local pain can develop or existing pain may intensify as a sign of an active infection, which is characteristic of
Infection: Here we see the classic and systemic signs of infection: Redness, heat, swelling and pain, along with multiplying bacteria. Oedemas develop around the wound, its surroundings are sensitive to pain, there is increased secretion of (as the case may be) purulent fluids. The patient may develop a fever and the blood count may show an increased number of leucocytes.
Wound smell
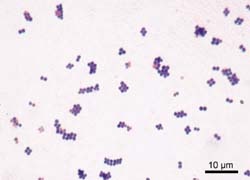
Smell is one of the first signs of an infection caused by certain types of bacteria. It is necessary to carry out an antibiogram and resistance determination to treat the pathogens systematically. Staphylococci and streptococci – particularly the MRSA strains – initially do not cause specific smells, which makes early identification difficult.
Suspected MRSA/VRE infection: These pathogens cause neither smells nor colourings of the wound cover. As the wounds may have existed for months or even years it is advisable to carry out a germ and resistance determination to prevent further development of resistance. Pseudomonas aeruginosa is phenotypically resistant to silver – one should use only dressings tested and certified by the manufacturer concerning their effectiveness against this species.
Wound rim
Chronic wounds, particularly those found on the lower extremities, point to underlying diseases not apparent or diagnosed for years. Each causes a typical appearance of the rim of a wound so that the therapist can start treatment accordingly.
An irregular, non-horny rim, independent of a warm foot and distended veins, can indicate an ulcus cruris venosum (venous leg ulcer). A regular wound rim with keratosis, independent of a cool, pale to bluish discoloured, and non-oedematous leg, can indicate an ulcus cruris arteriosum (arterial leg ulcer).
A regular, slightly raised and horny wound rim that almost looks cut out with warm, rosy but dry skin can be an indication of undiagnosed or insufficiently treated diabetes mellitus.
We purposely did not show the fourth criterion, wound exudate, because there is not an unambiguous correlation with certain underlying diseases and the resulting wound care procedures, which we have only been able to hint at. The important issue is to increase the clinical awareness of the signs that make wound diagnosis possible even at the first contact with the patient. This is then followed up with further diagnostics, particularly with regard to microbial colonisation.
08.03.2007