Vulvar cancer: a hidden disease
Vulvar cancer is the fourth most common cancer of the female genital tract. In 2008, roughly 3,460 cases of vulvar cancer will be diagnosed in the United States and about 870 will die of this cancer, according to the American Cancer Society.
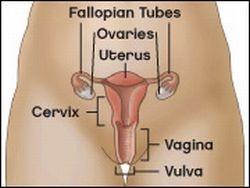
There are several different types of vulvar cancer. More than 90 percent are squamous cell carcinomas. Squamous cells are the same kind of cells that comprise most of the skin on the body and the cells that line the inside the body's cavities.
The second most common type of vulvar cancer is melanoma, accounting for about five percent of cases. Just like on other parts of the body, melanomas develop from the skin cells that produce pigment or color.
The cause of vulvar cancer is unclear, but human papillomavirus is suspected to be a possible risk factor, as is smoking. Patients infected with HIV, the virus that can lead to AIDS may also be more vulnerable to developing vulvar cancer.
"In premenopausal women, many of these cancers are associated with HPV types 16, 18 or 33," says Isabel Blumberg, M.D., a clinical instructor of obstetrics, gynecology and reproductive science at the Mount Sinai School of Medicine in New York, N.Y.
Vulvar cancer, which affects external female genital organs, is most common on the inner edges of the labia majora or the labia minora. The cancer can also affect the clitoris or Bartholin glands, the tiny, mucus-producing glands on either side of the vaginal opening. It most often affects women 65 years and older, but it can also affect younger women.
The symptoms may or may not be obvious. "Itching is a common complaint, although many patients may be asymptomatic," Blumberg said. Other symptoms may include:
- Pain or tenderness
- Burning sensation;
- Non-menstrual related bleeding;
- Any change in size, color, or texture of a birthmark or more in the vulvar area; or
- Open sores, bumps or lumps in the vulvar region.
"Any pigmented lesion in the vulvar area with an increase in size, change in color or development of ulceration should indicate further investigation," says Amy Freeman, M.D., a board-certified dermatologist in private practice in Millburn, N.J.
Like many cancers, the earlier the cancer is detected, the more curable it is. Vulvar cancer has a high cure rate, as long as it is detected and treated early. It's very important for women to seek medical attention if they experience persistent itching, burning or pain in the vulvar region, or if they notice skin changes or open sores that won't heal properly or in a timely fashion.
A biopsy is necessary to make a proper diagnosis. If the doctor finds an abnormal area in the vulvar area, he or she will biopsy a small piece of skin and examine it under a microscope. Vulvar cancer is most often treated with surgery. The type of surgery needed will be based on the size, depth and spread of the cancer. Radiation may also be necessary.
Women with a history of skin cancer may want to ask their dermatologists or gynecologists to add a vulvar examination to their annual check-ups. It is another opportunity for women to take charge of their own health.
More information about vulvar cancer is available from the National Cancer Institute's Web site: http://www.cancer.gov.
The article ist adapted from the original press release. Image courtesy: cdc
09.09.2008