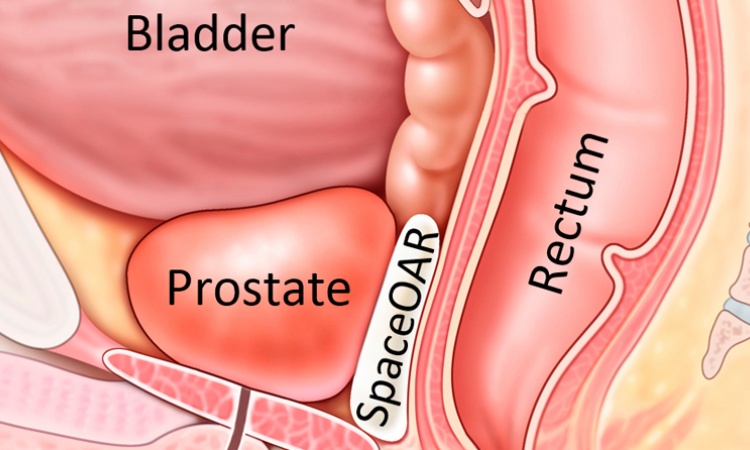
Treating bladder cancer
Hexaminolevulinate combined with guided blue light cystoscopy
Bladder cancer is highly challenging in terms of patient management and medical costs. As the fourth most frequent cancer in men and ninth in women in developed countries, although BC is a common disease it is still under-represented in public awareness and in cancer research .

Interviewed during the 28th Annual Congress of the European Association of Urology* in Milan, this March, Didier Jacqmin, Professor of Urology at Hôpitaux Universitaires de Strasbourg, France, and pioneer in BC since the 1980s, explained evolutionary changes in this field. ‘As the industrial risk factors decreased over time we saw more cases of non-invasive bladder cancer in people who smoked,’ he explained. ‘We also saw high rates of recurrence of 60 to 70% in the first three years after being diagnosed with non-muscle-invasive bladder cancer.’
In terms of the financial impact, he added: ‘In muscle-invasive cancer the costs can easily be calculated. You have an expensive surgery at the beginning, but after that the follow-up is quite simple. In other forms of cancer such as non-muscle-invasive bladder cancer you have very intensive follow-up plans, which are quite expensive.’
Over the last three decades he has seen achievements in patient management. ‘First we improved surgery, knowing that in some situations we were able to replace the bladder. However this cannot be performed in all patients. After that, chemotherapy was developed. Bladder instillations like mitomycin in non-muscle-invasive cancers and systemic chemotherapy for muscle-invasive cancer showed good results.
‘The next step was an improvement of the instruments from rigid to flexible and now to high definition video cystoscopes. The latest development for non-muscle-invasive cancer is the optical imaging agent hexaminolevulinate in combination with guided blue light cystoscopy. Since 1999, using this technique we can detect more lesions. Overall, the peak of the evolution in management of bladder cancer we see today is the much better detection of bladder cancer.’
Due to that use of hexaminolevulinate with guided blue light cystoscopy the rate of recurrence is decreasing. ‘This,’ he confirmed, ‘has been shown in many studies and I can see it with my patients.’
The professor found it more difficult to answer the question of a cost-benefit ratio when investing in blue light-guided cystoscopy. ‘It depends on the country you are working in and its associated health system,’ he explained. ‘However by reducing the recurrence rate, it reduces the number of hospitalisations and therefore the overall cost. It also has an impact on the quality of life of the patients.’
For those patients, there is a further plus to the system. ‘With blue light-guided cystoscopy you have a very clear and easy to understand image,’ Prof. Jacqmin pointed out. ‘People like images, they tell you much more about the disease than words. The patients understand their disease much better when you show the pink colour of the tumour.’
* Sponsored by Ipsen
29.07.2013