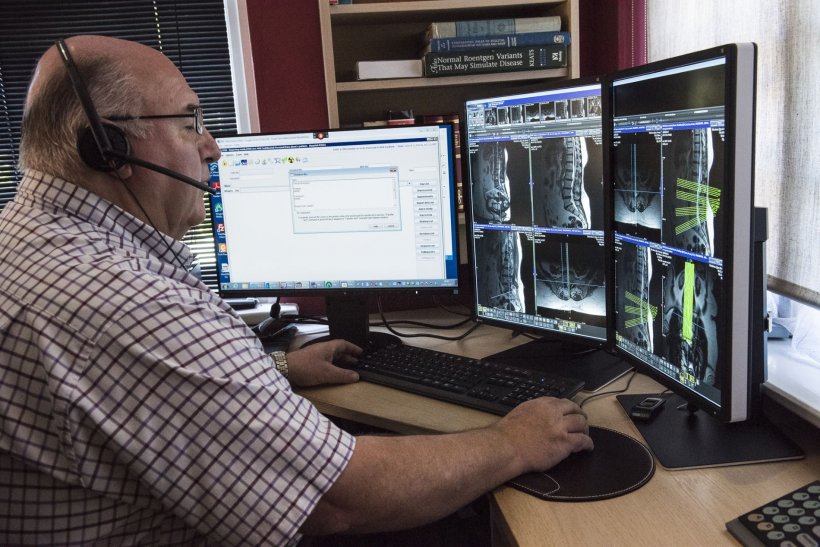
Image source: Medica
Article • Imaging workflow challenges
The long-term impact of Covid-19 on teleradiology
The coronavirus pandemic – an international tragedy – created unprecedented upheaval and challenges within health systems, economies, and society. In hospitals, new ways of working had to evolve. Social distancing led to virtual consultations and teleradiology has found an added dimension, with its success, practicality, and effectiveness likely to see more widespread future use. We asked three radiologists about the relevance of teleradiology during the epidemic, and what the future holds.
Report: Mark Nicholls

Evidence collected during the SARS-CoV-2 pandemic by a team from the University of Tennessee, USA, clearly showed changing patterns in the use of teleradiology. Dr Mohammed Quraishi, Assistant Professor of Radiology, Section Chief of Body Imaging and Informatics Director at the University of Tennessee Medical Center, believes the term “teleradiology” needs disambiguation. ‘Often it brings to mind a radiologist far removed geographically, perhaps in a different country, reading for multiple hospitals with limited rapport with any specific hospital,’ he said. ‘I would term this “external teleradiology”, because the radiologist is external to the local group. It's important to differentiate this from ”internal teleradiology” where a radiologist, employed by the practice, reads remotely.’
In the USA, practices during the pandemic increased internal teleradiology, and significantly decreased external teleradiology. ‘The reason seems two-fold,’ Quraishi surmised. ‘First, removing radiologists from the hospital makes sense when trying to mitigate the risk of contracting SARS-CoV-2 and, second, the increase in internal teleradiology – as opposed to external teleradiology – was almost certainly due to the drastic decrease in case volume.’
Whilst, traditionally, internal and external teleradiology have been used for on-call and overnight shifts for emergency radiology cases, day-time shifts during the pandemic were transferred to internal teleradiology – bringing off-site reading into the daily fold to help decrease radiologist exposure to potential SARS-CoV-2 infection, and allowing radiologists to work at home. The increased use of internal teleradiology was seen throughout the USA – particularly in the northeast, where the pandemic had prevalence.
To gauge changing teleradiology use, the group queried 290 locations, representing a geographically diverse cross section of institutions. They found an overall jump in the proportion of sites installing home workstations (65.2%) and switching normal daytime shifts to internal teleradiology (73.6%). Around 56% of respondents said they saw enough benefit from the experience that they plan to continue similar workflows post-COVID.
Specifically, 64.8% reported decreased stress levels, and 96% found improved or no change in turnaround times, a position Quraishi echoed from his personal experience. ‘I found internal teleradiology less stressful, with an overall increase in productivity,’ he said. ‘Radiologists also reported less interruptions at home allowing them to focus on interpreting studies.’ He believes the pandemic will see a change of emphasis in the use of teleradiology, with practices re-evaluating teleradiology with new business models, services and workflows, such as second opinion reads or even practices sending out studies for subspecialty interpretations.
Recommended article

Article • Professional affairs
Radiologists suffer from burnout and gender inequality
In an exclusive interview, Mauricio Castillo, president of the American Roentgen Ray Society (ARRS), spoke about the impact of dissatisfaction and gender discrimination in radiology, the focus of his Wilhelm Conrad Roentgen Honorary Lecture at ECR 2017.
Teleradiology to fight burnout problems
Given increased evidence of radiologist burnout and demands for better work/life balance, teleradiology might offer a solution. ‘According to our survey, the majority of groups plan to incorporate internal teleradiology into the post-pandemic workflow. I predict internal teleradiology will rise across the country and, as groups get comfortable with that, there will likely be spill over into external teleradiology.’

Former NHS consultant Dr Stephen Davies, now Medical Director of the Medica Group, a business providing teleradiology services to the NHS, said: ‘Working from home using teleradiology has allowed radiology teams to work “in hospital” and out of hospital on rotation and increase opportunity for social distancing.’ Medica has facilitated “pass through” home reporting for radiologists to undertake their NHS sessional work using Medica’s existing image transmission and reporting. ‘The culture shift towards using technology to enable high-quality home working has risen during the COVID-19 crisis,’ he pointed out. Teleradiology has been used across the scope of diagnostic imaging, from emergency reporting – stroke and COVID chest X-rays – to elective imaging, and geographically this has been ‘without boundaries and is widespread’.
Teleradiology – a long-term growth
‘Teleradiology has been on a long-term growth trajectory and this will continue,’ Davies predicted. ‘COVID has increased the understanding of working from home. Teleradiology providers deliver a scalable, flexible quality assured reporting service which can respond to geography, reporting demand, time constraints and subspecialty constraints.’ He believes post-crisis teleradiology will become a bigger part of daily work routine with radiology services finding a new balance between ”in house” face-to-face radiology and protected and uninterrupted teleradiology home working. However, Davies has noted a downturn in volumes for all teleradiology services during the crisis, primarily due to a fall in elective work and emergency cases during lockdown, although, as restrictions ease, elective imaging services are increasing.
Yet over the last decade, Dr Davies said teleradiology has been growing and is part of service provision for more than 90% of the NHS, with the delivery technology becoming ever-more sophisticated. That now sees the Medica Group offering a round-the-clock service across 90 UK hospitals. ‘The more experienced users of teleradiology have integrated the provision into their service in a seamless fashion. I expect this trend to continue and increase,’ he added.
Key lessons have been learned in teleradiology use during the epidemic, primarily from the NHS, rather than teleradiology companies – particularly ‘successful teleradiology replicating NHS office radiology requires more than simple deployment of a workstation over simple domestic broadband. ‘Teleradiology,’ he predicts, ‘will continue to become more sophisticated with increasingly advanced operational delivery and image review, both supported by artificial intelligence. Its penetration will increase into the provision of radiology reporting both emergency and elective work and will also use its platform and operational expertise to deliver emerging digital telepathology.’

With the Basel area a COVID-19 hotspot in Switzerland, the Department of Radiology at the University Hospital Basel provided support via its teleradiology capability. As cases rose in March, the unit – which delivers regular teleradiology services to local and regional hospitals at night and weekends – introduced a structured CT reporting template for COVID-19 cases that included quantification of lung opacifications. ‘Around the peak of new infections in Switzerland at the end of March,’ said Dr Thomas Weikert, resident at the department, ‘we saw increasing numbers of CTs performed with the question of COVID-19 associated pulmonary infiltrates rising by +17% a day. ‘If that continued, we would have been in serious trouble very quickly. Luckily, the curve flattened during April as rigid public health measures taken by the Swiss authorities brought the number of new infections down. We were also developing automated quantification pipelines to prepare ourselves for the situation where it was not possible to conduct all the analyses manually.’
For COVID cases, lung segmentation was conducted and via density thresholding, the percentage of lung tissue affected by infiltrates was established. ‘This is very useful for clinicians especially when it comes to follow-up. It is about quantifying COVID-related changes.’ The unit (which also runs an international expert teleradiology reading program to provide structured reporting on Idiopathic Pulmonary Fibrosis (IPF) cases, which allows hospitals in Central Eastern Europe and Asia to send high-resolution chest CTs of suspected IPF to the university hospital), has continued to provide structured COVID-19 reports to local/regional partner hospitals via teleradiology.
The value of teleradiology during the pandemic has been apparent and the Basel department monitored its growth during this period with an internal RIS/PACS crawling tool, allowing them to identify all exams with COVID-19-related clinical questions. ‘Teleradiology for COVID-19 cases can prove beneficial in three respects. First,’ Weikert continued, ‘by promoting structured reporting, including quantification of pulmonary changes; second, should regional hotspots arise in the future, overwhelming capacities of the regional health service providers, teleradiology could share the diagnostic workload with radiology departments in less affected areas; third, by automatically analysing cases from many regions, it could be part of a regional outbreak early warning system. If many exams are diagnosed with COVID-19-suspected pulmonary changes, a warning signal could be sent to the authorities. I think, in a broader way, telemedicine, which includes teleradiology and provision of services of other specialties, will get a profound boost by this, because there are many people who used telemedicine for the first time and I think they will continue to use that.’
Consequently, Weikert expects the role of telemedicine and teleradiology to rise independently of the current public health crisis.
Profiles:
Dr Mohammed I Quraishi is Assistant Professor of Radiology, Section Chief of Body Imaging and Informatics Director at the University of Tennessee. He researches data analytics and medicine, working towards ultimately improving patient care through advancing healthcare efficiency, diagnostic accuracy, cost-savings, and mitigation of physician burn-out.
Dr Stephen Davies is Medical Director of the Medica Group and Fulltime Executive Director. A former NHS radiologist, with more than 25 years’ experience as a consultant radiologist within the NHS, he is also a Past President of the British Institute of Radiology.
Dr Thomas Weikert is a resident in the Department of Radiology at University Hospital Basel, Switzerland, where he researches translation of digital solutions in medicine and is involved in an evaluation of the IPF teleradiology program.
15.07.2020





