Test combination predicts high risk of relapse and death in bladder cancer patients
A new testing approach has effectively identified patients at the highest risk of cancer relapse after bladder cancer surgery, according to a study published in the February issue of The Lancet Oncology http://oncology.thelancet.com. Vol 8 Feb 2007 91.
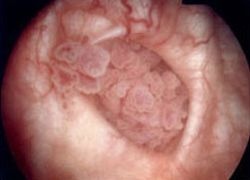
‘Bladder cancer and apoptosis: matters of life and death’). ‘Bladder cancer recurs in many patients after radical cystectomy (bladder and surrounding tissue removal). Conventional prognostic features such as tumour grade, stage, and lymph-node status are not accurate enough to predict outcomes in patients with bladder cancer,’ explained Dr Yair Lotan, one of the study’s researchers at the Texas Southwestern Medical Centre, Dallas, Texas.
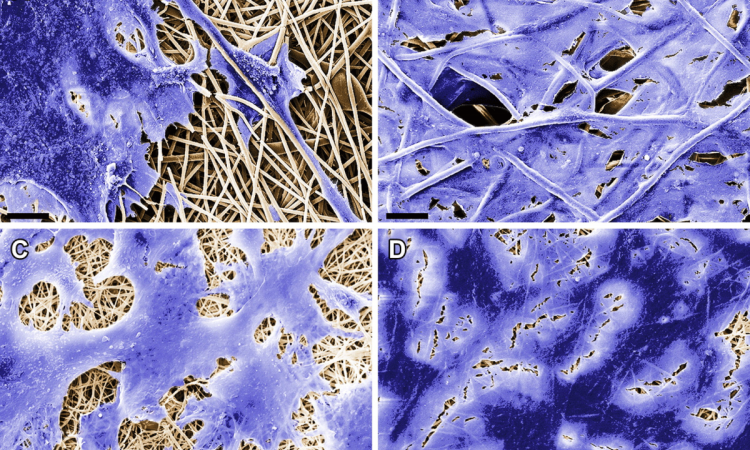
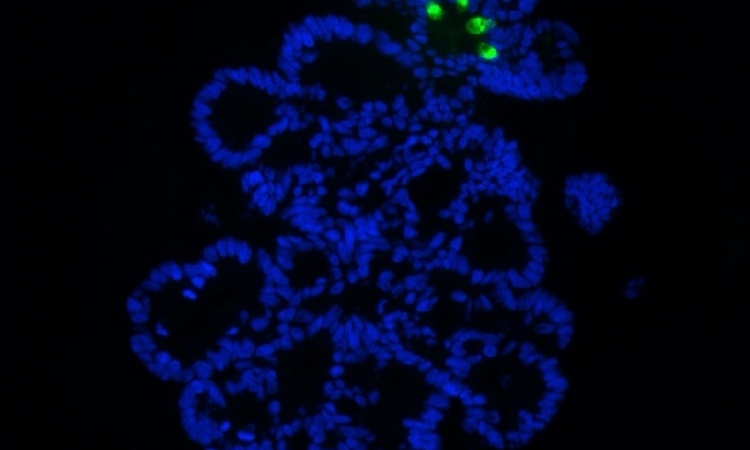
For the study, the team analysed bladder samples, from 226 patients, which had been removed during bladder cancer surgery. Using a tissue profiling technique, the authors tested for four different proteins (P53, Bcl-2, caspase-3, and survivin) which have been implicated in causing cancer. When hen expression of all four proteins was altered, the researchers found the patients had a greater risk of developing a recurrence of their bladder cancer - and eventual death from the disease - compared with patients who had no change of expression of these proteins. ‘We found that evaluation of combined apoptosis biomarkers [markers of cell death] status can help identify patients at high risk of recurrence and death from bladder cancer after radical cystectomy, independent of conventional prognostic features,’ said Dr Jose Karam, another member of the research team.
Lead researcher Professor Shahrokh Shariat, the teams lead researcher added, ‘…clinical trials are needed to target bladder cancer in patients with a high number of [alterations], as these patients have poor survival rates with current treatments and might benefit the most from experimental therapy’.
In a Lancet Oncology ‘Reflection and Reaction’ link (see website), Dr Francisco Real and Dr Nuria Malats commented that this is the first study in which multiple apoptosis markers have been used together to assess the value in improving accuracy of predicting outcome for patients with bladder cancer. However, they add: ‘Although the paper provides important, novel information, the findings do not call for any change in current clinical practice.’
They point out: ‘Ideally, these hypotheses should be tested in multicentre prospective studies in the context of either standardised clinical care or therapeutic trials. Even then, the results will need to be independently replicated before clinical application is justified. These studies will require five years or more of follow-up, depending on sample size, to achieve the number of events necessary to reach statistical power. Because many other markers are rapidly being reported (e.g., molecular profiling), it would be more efficient to assess them within the same studies, to better compare their predictive accuracy. Meanwhile, confirmation in large, high quality, retrospective studies might be warranted; this strategy could allow for a pre-screening of the many competing markers, to reduce the number of hypotheses to be tested in prospective studies, and the likelihood of false-positive results.
‘The major challenge that urologists, oncologists, pathologists, and general scientists face is to integrate their scientific interests and work together in large, collaborative, prospective studies in order to answer questions of clinical relevance. It is certainly not an easy task, but it is a matter of life or death.’
Contact: Dr Jose Karam, UT Southwestern Medical Centre, Dallas, USA. Phone: 001-214-417-7687
08.03.2007