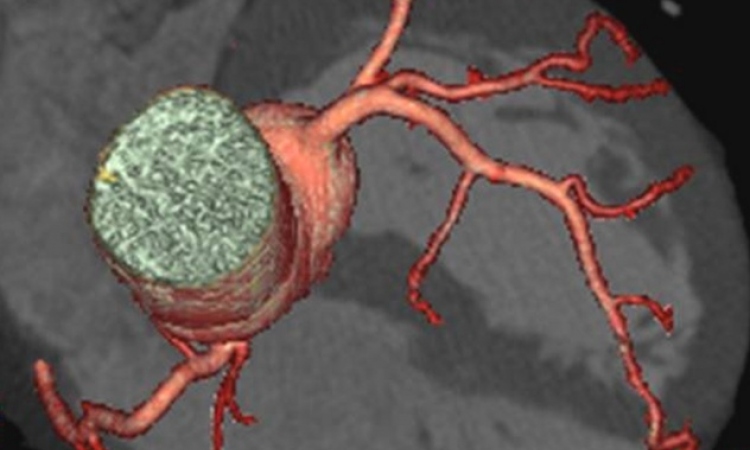
Should CTA become a screening procedure?
With low tube voltage, reduced radiation and contrast agent dose, the system delivers sufficient and meaningful data
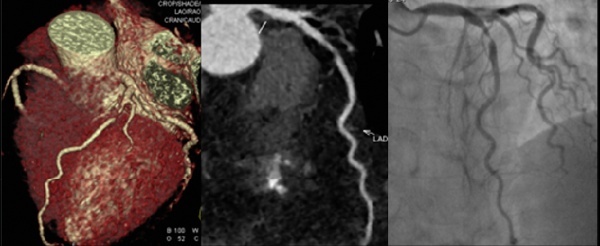
CT angiography (CTA), an objective method to visually assess cardiovascular risk, provides reliable data that can help save treatment costs. As CTA is becoming less invasive due to reduced radiation and contrast agent dose, low tube voltage and new technologies the technique’s popularity among physicians is increasing. In view of these facts, could CTA become a screening tool for disease prevention? Radiologist Professor Uwe Joseph Schöpf, specialist in cardiology and paediatrics and Director of the Division of Cardiovascular Imaging at the Medical University of South Carolina in Charleston, is carefully optimistic: ‘At least we are now in a position to collect sufficient and meaningful data on this issue.’
Selective procedure
A CTA frequently shows that an alleged high-risk patient is not at such a high risk after all – a fact that has obvious implications for treatment costs. For example, a patient with a high lipid level undergoes a CTA but the scan shows no arteriosclerosis whatsoever. Imaging thus indicates that a long-term therapy to rigorously decrease lipid levels might not be necessary. In short: Imaging shows which patients really do need therapy and prevention. ‘This is an important contribution to cost efficiency – made by an imaging procedure. Quite a surprise in view of the fact that imaging is often considered expensive and a prime candidate for cost reduction initiatives,’ the cardiologist points out.
Prospective triggering supports dose reduction
High risk or not, and is there a stenosis in the coronary arteries and if so, how severe is it? These are important questions for cardiac patients – 80 to 90 percent of whom can be examined using a prospectively triggered CTA protocol (approx. 1 to 3 mSv), which provides reliable and precise diagnostic information. A major advantage: Heart rate does not affect this procedure; 80 to 110 bpm are no problem and do not result in artefacts as long as the heart rate is not too irregular. ‘It is important to trigger during systole, not diastole – a fact not every CT operator is aware of,’ Prof. Schöpf points out. Contrast agents are applied when stenoses need to be detected or when arteriosclerotic changes, including unspecified coronary plaque, need to be visualised comprehensively. High-speed CT allows further dose reduction – currently, however, this new technology is limited to patients with a suitable heart rate.
Alpha and omega: low tube voltage
Radiation dose depends on tube voltage and obviously patient physique. ‘With normally built patients we perform a prospectively triggered exam at 100 kV, which means a radiation exposure of 1 mSv and less,’ the expert explains. The adjustment of tube voltage to the individual patient is an important and very simple tool to reduce exposure effectively. Tube voltage also affects the signal transfer of the contrast agent: the lower the voltage the stronger the signal and lower the necessary contrast dose. Professor Schöpf: ‘Today, a complete CTA at 80 kV can be performed with 30 ml of contrast agent.’
Increasing new technologies
In recent years the discussion – initiated primarily by US physicians – focused on dose reduction. Today, many technological innovations aim to reduce voltages, independent of patient physique. ‘Now there are even programmes that determine the optimal tube voltage automatically for each patient. This makes the standard protocol of 120 kV, which is very popular in the US, obsolete,’ Prof. Schöpf adds. Another factor that previously limited voltage reduction was the actual capacity of X-ray tubes. The systems could develop sufficient current to scan a patient at low voltage only if the patient was very lean. ‘This is another technological problem that has been solved: Now we can use low tube voltage across the board.’
Imaging for preventive screening?
He believes that more patients can benefit from this technology due to three major factors – low tube voltage as the precondition for reduced radiation dose and reduced contrast dose – which continuously reduce CTA invasiveness. ‘In view of these innovations we should seriously consider CTA as preventive screening procedure,’ the expert suggests. Whether in the end cardiac CT will really be a suitable procedure to risk stratify patients and to determine medication remains to be seen – currently the available data do not allow a final conclusion. Since there are low invasive techniques and procedures, Prof. Schöpf sums up: ‘It’s our task to do further research on cardio CT and to provide meaningful data to assess the suitability of the procedure.’
Profile:
Austrian-born Professor Uwe Joseph Schöpf studied medicine at Ludwig Maximilian University in Munich, Germany, where he then became a resident at the diagnostic radiology unit at Klinikum Grosshadern. His cardio-thoracic imaging interests led him across the Atlantic to Brigham & Women’s Hospital, Harvard Medical School in Boston.
Today he is professor of radiology, cardiology and paediatrics and Director of the Cardiovascular Imaging Division at South Carolina Medical University in Charleston, SC, and a renowned expert in CT and MRI diagnostics. His national and international medical societies’ awards and honours are numerous, and Medical Imaging Magazine has twice ranked him among the ‘Top Ten Cardiovascular Imagers in the Nation’.
03.03.2014