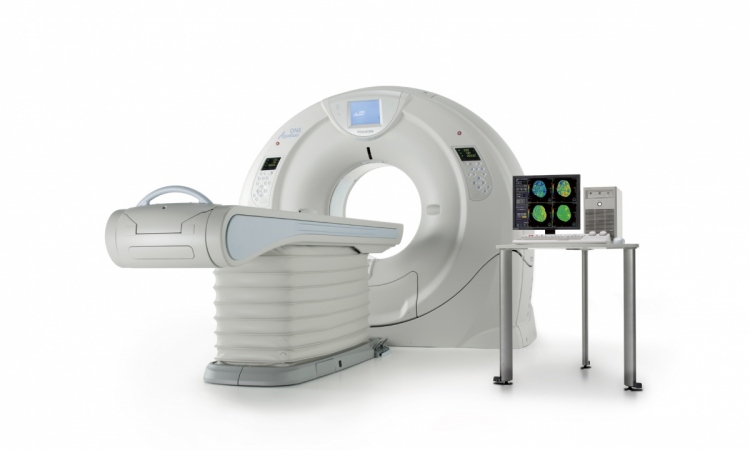
Radiation dose-reduction strategies
Depending on the institution, CT examination doses can vary dramatically by a factor of ten, said Professor John Damilakis, PhD, associate professor at the University of Crete, Iraklion, ahead of the session. The difference is related principally to variations in the examination technique, as the protocol or the imaging system itself determines the level of radiation.
According to Prof. Damilakis, unjustified CT examinations and non-optimised examination protocols are significant contributors of unnecessary dose. Appropriate selection of exposure parameters, reduction of scanning length and minimisation of the number of scans included in a single imaging study would all contribute to dose optimisation. Moreover, automatic exposure control, if used appropriately, is an effective technique for patient dose reduction.
'Over-scanning', the additional rotation of the x-ray tube at each end of the scan length, which allows the first and last slices to be reconstructed, contributes significantly to overall patient exposure during the examination. Typically, the over-scanning doses are not included in calculations of effective dose, which are usually based on the planned scan volume and not the actual volume exposed. Prof. Damilakis recommends appropriately selecting three parameters – beam collimation, pitch and reconstruction slice width – to limit the extent of over-scanning.
“The relative contribution of extra x-ray exposure due to over-scanning may be considerable, especially when the planned image volume is limited, as in paediatric studies for example,” Damilakis said. Children and adolescents are more radiosensitive than adults, so appropriate dose management is very important for them.
PET/CT
PET/CT has now replaced standalone PET for many oncology applications. The level of radiation exposure from CT can be several times higher than that from PET, but patient exposure can vary depending on the clinical indication and combined imaging protocol, according to Dr. Thomas Beyer, a teaching professor at the University Hospital Essen and CEO of cmi-experts, a company specialising in cross-modality imaging.
CT is often only needed to give a rough anatomical framework to the PET images, for instance when assessing therapy response in lymphoma patients. In other cases such as primary staging of a head or neck cancer, a fully-diagnostic, contrast-enhanced CT study is required.
Beyer suggests using PET/CT instead of CT or PET when clinically indicated. Perhaps most importantly, radiologists and nuclear medicine physicians must cooperate to define the most appropriate imaging parameters for different clinical indications for PET/CT.
It is crucial to consider risks together with the benefits brought by advances made in both modalities, said Dr. Dr. Reinhard Loose, associate professor and head of the institute for Diagnostic and Interventional Radiology at the Nuremberg North Hospital in Germany. Technological progress has helped reduce the likelihood of patient morbidity and/or mortality in some areas, for instance in patients with severe polytrauma. Twenty years ago, the diagnostic
work up used to take 35 to 45 minutes for separate imaging examinations. Today, polytrauma victims can be imaged within 20 seconds thanks to multi-slice CT, allowing more patients in a critical condition to undergo this examination.
Finally, patients who receive CT scans regularly are very ill, and the likely reduction in life expectancy from their medical condition is much greater than that associated with the CT examination they undergo. The justification of CT use is more critical when it comes to outpatients and participants in screening programmes.
But the development of referral criteria for imaging studies should help to reduce the number of inappropriate CT and x-ray examinations, as is the case in paediatric radiology, Loose stressed.
08.03.2009