Radiation dose and digital mammography
By Kerry Heacox
The use of mammography to maintain breast health comes with a caveat: exposure of the breast to radiation, which can increase the susceptibility risk of breast cancer. Thus, using the lowest possible radiation dose for mammograms is of utmost importance.
A standard mammography examination with four exposures, two to each breast, is approximately equivalent to a whole-body dose from background radiation over the course of a year. Radiation dose from a mammogram is a direct consequence of the amount of X-rays that are absorbed in the breast tissue. With a well calibrated mammography unit, no other tissues of the body are exposed to X-rays. Radiation dose is affected by the energy of the X-ray beam, the thickness and composition of the breast, amount of compression, and type of imaging equipment used.
The introduction of digital imaging systems for mammography provides a lower dose alternative option for mammographers and patients. One of the advantages of digital mammography systems over traditional analogue screen-film ones is that dose can be reduced by at least 30%. New technological innovations are providing even greater levels of dose reduction.
Mammography is a very technically demanding radiographic procedure because it simultaneously requires high spatial resolution and good dose performance. High resolution is needed, because some objects that must be depicted are very small microcalcifications, which need to be visualised when they are as small as 200 microns.
Years of engineering development and clinical experience proved that molybdenum was the optimal X-ray tube anode material for breast imaging with traditional screen-film systems. Analogue mammography has a very limited dynamic range determined by the screen-film combination. The introduction of digital mammography systems using molybdenum X-ray tubes have already demonstrated a 30% reduction in dose compared to analogue mammography systems.
Recent clinical trials and scientific investigations have determined that a tungsten X-ray tube with rhodium and silver filters will allow for an additional dose reduction of up to 30%. The use of a tungsten anode in the X-ray tube also offers superior performance for new technologies currently in advanced stages of development and clinical testing, such as digital breast tomosynthesis, iodinated contrast, and dual energy breast imaging.
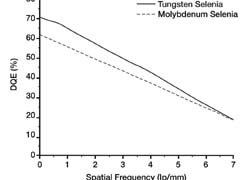
Hologic Inc. has replaced molybdenum X-ray tubes with tungsten X-ray tubes in its Selenia digital mammography system. In laboratory testing, using identical Selenia systems, with the exception of the type of tube used, with radiation dose of 1.0 mGy imaging a breast phantom, superior imaging was achieved with a better Detection Quantum Efficiency (DQE) curve. This produced better digital images (fig. 1.)
The addition of a silver filter enables large breasts to be imaged better. Silver filters, which replace molybdenum ones, produce superior imaging performance at lower dose. They also reduce the X-ray exposure time that is needed for women with large and/or dense breasts, and that reduces the potential problems associated with patient motion. The use of silver filters with Selenia systems ensure that superior image quality is not compromised by breast size or density (fig 2).
Hologic also has eliminated the need for dual track anode X-ray tubes. In the golden age of screen-film mammography, X-ray tubes with dual track configurations were used on some analogue mammography X-ray systems to enable dose optimisation for large breasts. But dual track configuration X-ray tubes are less reliable and more expensive than single-track configurations. A Selenia system with a single track tube can deliver the highest current exposure needed for the largest breasts at an acceptable exposure time reducing motion artifacts. This ensures against underpenetrated images, long exposure motion blur and poor quality. The use of a single track configuration with a tungsten X-ray tube in digital mammography systems minimises the need for retakes – and repeated radiation exposure – and ensures that women of all breast sizes and densities will have mammogram images of superior quality.
The mammogram radiation dose is a minimal risk for women compared to the benefit of early breast cancer diagnosis. Digital mammography reduces the risk further by substantially reducing dosage needed to produce superior image quality that reveal much more breast detail when displayed on a diagnostic workstation equipped with mammography specific image processing tools. Digital mammography benefits mammographers, and in terms of lower radiation dose for a lifetime of mammograms, the patients who receive them.
28.10.2008





