Prostate scanning too often performed?
Experts on a US panel expressed their doubts on the beneficial quality of prostate cancer screenings for elderly men. Prostate cancer often grows very slowly and may not kill an older man before he suffers from another death reason, they pointed out.
The U.S. Preventive Services Task Force, a panel of 16 experts who guide national health care, issued its report this week, based on a review of past research.
The panel reviewed studies since its last recommendations in 2002. It concluded that for men under age 75, there is too little evidence to determine whether treatment for prostate cancer detected by a PSA blood test offers any benefit over treatment given after cancers are detected by other means, usually when symptoms begin.
Treatment often causes "moderate-to-substantial harms," including impotence and bladder control and bowel problems, the task force said, without evidence it saves the lives of these elderly men. Prostate cancer often grows very slowly and may not kill an older man before he dies of something else, the risks of early treatment may not outweigh the benefits.
"At this point, we recommend that men concerned about prostate cancer talk with their health-care providers to make a decision based on their individual risk factors and personal preference," Dr Ned Calonge of the Colorado Department of Public Health and Environment and chariman of the task force said.
"I think it's a very well done and justifiable recommendation," said Dr. Barnett Kramer, associate director of disease prevention at the National Institutes of Health. "They continue to say the jury is still out for men under 75."
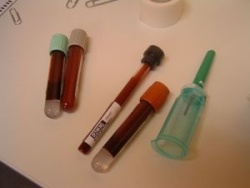
Prostate cancer screening is done with two tests: a blood test that measures prostate specific antigen, or PSA, and a digital rectal exam. The blood test is controversial because the PSA level can be high for many reasons. A positive result from the test must be confirmed by a biopsy. And there's no agreement on the best way to treat it: "watchful waiting," surgery, hormone therapy, radiation or some combination of those.
"I think they're really missing the boat," said William J. Catalona, a professor of urology at Northwestern University. "It's a disservice to patients. A lot of men die from prostate cancer, and there's just an overwhelming amount of evidence that screening saves lives."
Screening is "an area of very intense controversy," said Dr. Durado Brooks, a prostate cancer specialist for the American Cancer Society. "There are many doctors who believe staunchly that PSA testing should be done in all men and there are probably an equal number of doctors who believe very much that testing is of limited value."
Most major U.S. medical groups recommend doctors discuss the potential benefits and known harms of prostate screening with their patients and make individual decisions. And most agree routine testing shouldn't occur before age 50.
The cancer society's advice for screening doesn't set an age to stop screening but suggests that men shouldn't be offered screening if they aren't expected to live another 10 years, Brooks said.
"That's because every 75-year-old is not created equal," he said.
While some have health problems and aren't likely to live long, others are "very active, very vigorous and have minimal health issues, and many of those men are going to live into their late 80s or 90s," Brooks said.
Ryan, in San Francisco, said age shouldn't be the sole measure. "It would be a disservice to patients to have their chronological age be the only factor making important health decisions," he said. "There are some very young 75-year-olds out there."
But rather than feel slighted by the recommendation, Dr. William Hahn of the Dana-Farber Cancer Institute in Boston said those over 75 should "feel liberated from having to have the test. It's one less thing for people over 75 to worry about."
The new guidelines were published in the Annals of Internal Medicine.
The group said two large studies under way -- one in the United States and one in Europe -- should help clarify questions about the benefits of screening in men under 75.
15.08.2008




