Article • Neuro- and spine surgery
Perfection in the networked OR: robot, neuro-navigation and VR headsets
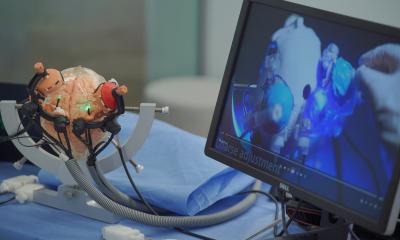
At their workplace, neurosurgeons often have to make compromises since most ORs were not designed with the specific needs of their discipline in mind. To address this issue the University Hospital in Essen, Germany, equipped an OR especially for neuro- and spine surgery. The aim is nothing less than revolutionizing the field with the help of digitalisation and cutting-edge technology.
Report: Sonja Buske

“For some time, we had been planning to integrate intraoperative imaging in the OR but there was no device on the market that met our requirements,” says Professor Dr Karsten Wrede, deputy director of the Department of Neurosurgery and Spine Surgery at the University Hospital Essen. While previously, as Professor Wrede explains, the surgeons had to make a choice for their intraoperative imaging modality – either MRI or CT now “The robot-guided angio system Artis pheno by Siemens Healthineers provides CT images thanks to 3D acquisition technology in top quality and which allows us to perform angio at the same time.” He adds that „Thus we have a single system with which we can perform almost all interventions and which makes the choice between CT and MRI obsolete.”
Installation without shut-down
In order to be able to install this innovative technology in the OR the space had to be expanded. “Not a trivial task without a shut-down,” Wrede remembers. Moreover, Siemens requirements such as lead-enforced walls and adequate safety distances had to be met. “In this particular case, the Corona pandemic turned out to be an advantage. Since we had to reduce the number of surgeries we were able to entirely close one OR for five months,” says Wrede. In addition to the x-ray robot, a complex neuro-navigation system and a robotic arm by Brainlab was installed. After almost three years of prep work, the big day came: right after Easter 2021 the new room was opened.
Unique combination of systems
“The systems by themselves are nothing spectacular – they are used in many hospitals. What’s unique in Germany is the combination and the networking as well as the fact that this OR is specifically set up for neuro- and spine surgery,” Professor Wrede reports proudly. At the same time he concedes that not all technology is fully used in each intervention: “When we are dealing with an aneurysm, we do use the entire set-up but when we fixate screws in the spine, that’s not necessary.” The surgeon is particularly impressed by the many advantages of the networked robotic unit:
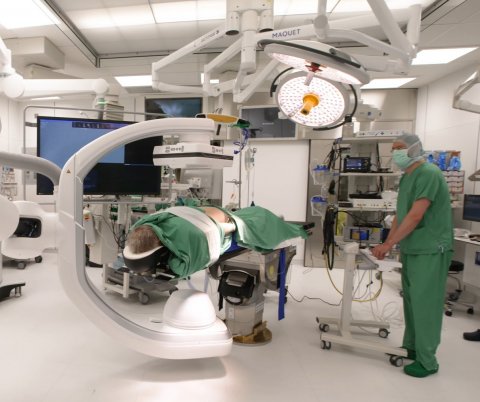
“Before, we made x-rays while fixating the screws in order to check their position. This means high radiation exposure for the patient and the team. Later, we used a 3D x-ray system which was rather cumbersome. Now we can take a 3D image in the OR within 10 seconds without the staff having to leave the room. The image is sent right to the navigation software and we can then guide the robot to the sites in question.” Before the patient leaves the OR, a final image is acquired in order to check the screws. With this technology, Wrede explains, “screw positions that need to be corrected are a thing of the past”.
In brain surgery, the combination of neuro-navigation and ultrasound is crucial. When for example a tumour has been partially removed a 3D ultrasound image can be acquired intraoperatively that shows the remaining tumour tissue live. “That’s much faster than a time-consuming intra-operative MRI,” Wrede points out. Moreover, the ultrasound data can be transmitted to the microscope. Thus the surgeon does not have to interrupt their workflow to review the images on-screen.
Virtual anatomy turns real
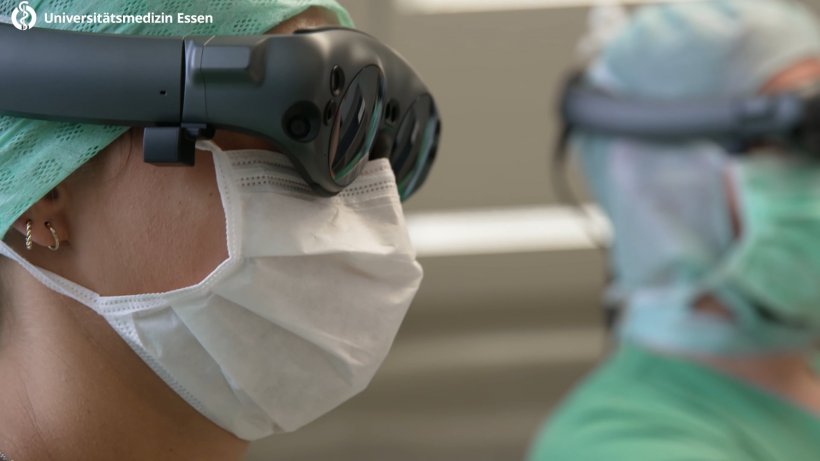
The VR headset shows [our young physicians ]the patient’s vessel structures on-site. They don’t have to imagine where exactly the aneurysm is located in the head. They see it right in front of them
Karsten Wrede
Aneurysm patients also benefit from the checks in the OR. While before an angio had to be performed three to four days after the surgery without anaesthesia, it can now be done on the open skull. Thus remaining damaged vessels are instantly detected and treated. With aneurysms another new technology is used: VR headsets. While they have not yet been approved for intraoperative use, they are a helpful tool for preoperative planning: “Particularly for junior physicians it is quite a challenge to fully understand the complex anatomy of the brain and the spinal cord. Thus our young physicians and students love this technology as the VR headset shows them the patient’s vessel structures on-site. They don’t have to imagine where exactly the aneurysm is located in the head. They see it right in front of them.” Professor Wrede can well imagine that in the future stand-alone navigation systems will be replaced by VR headsets with integrated navigation.
With all these benefits, we must not forget that the complex technology requires a longer learning curve and a well-attuned team. “We had one week of training but still only scratched the surface,” Wrede admits. “No manual tells you how to position a patient for a certain intervention. That is something we learn with practice. In addition, it’s not sufficient for a few physicians to master the technology. The entire team has to be familiarized with their tasks and that takes time“, he emphasizes. Nevertheless, he is convinced that the approach of the University Hospital Essen is the future: “The technology, particularly VR and AR, will revolutionize healthcare.”
Profil:
45-year-old Professor Dr Karsten Wrede has been deputy director of the Department of Neurosurgery and Spine Surgery at the University Hospital Essen, Germany, since 2019. He studied medicine in Greifswald and Ulm after having completed paramedic training. Before joining University Hospital Essen in 2009 as junior physician, he had worked in Switzerland, the US and China. In 2013, he was appointed senior physician and in 2018 managing senior physician. His main areas of interest are vascular neuro-surgery, skull base surgery as well as cerebral and spinal tumour surgery.
27.10.2021