MRI may replace biopsies
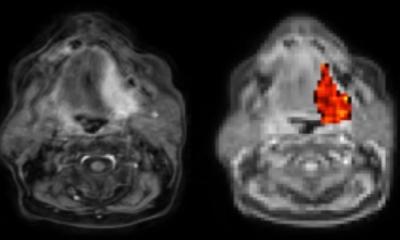
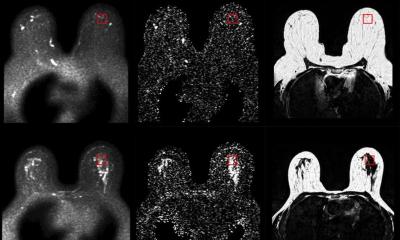
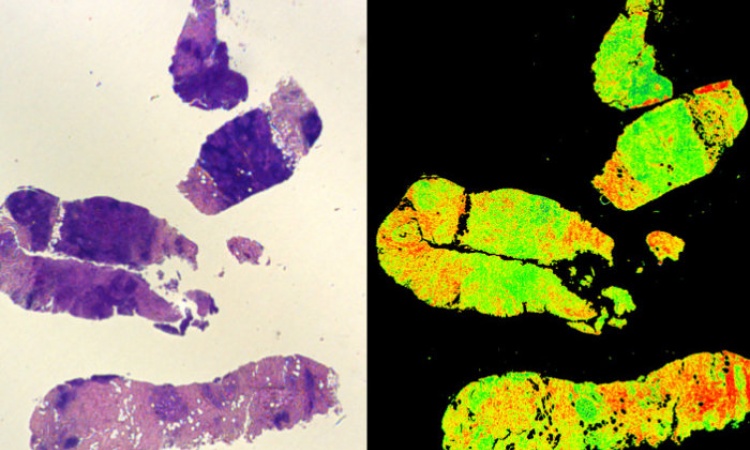
Imaging tests like mammograms or CT scans can detect tumors, but figuring out whether a growth is or isn’t cancer usually requires a biopsy to study cells directly. Now results of a Johns Hopkins study suggest that MRI could one day make biopsies more effective or even replace them altogether by noninvasively detecting telltale sugar molecules shed by the outer membranes of cancerous cells.
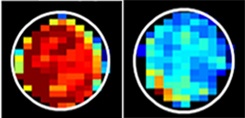
“We think this is the first time scientists have found a use in imaging cellular slime,” says Jeff Bulte, Ph.D., a professor of radiology and radiological science in the Institute for Cell Engineering at the Johns Hopkins University School of Medicine. “As cells become cancerous, some proteins on their outer membranes shed sugar molecules and become less slimy, perhaps because they’re crowded closer together. If we tune the MRI to detect sugars attached to a particular protein, we can see the difference between normal and cancerous cells.”
Bulte’s research builds on recent findings by others that indicate glucose can be detected by a fine-tuned MRI technique based on the unique way it interacts with surrounding water molecules without administering dyes. Other researchers have used MRI but needed injectable dyes to image proteins on the outside of cells that lost their sugar. In this study, Bulte’s research team compared MRI readings from proteins known as mucins with and without sugars attached to see how the signal changed. They then looked for that signal in four types of lab-grown cancer cells and detected markedly lower levels of mucin-attached sugars than in normal cells.
Xiaolei Song, Ph.D., the lead author on the study and a research associate in Bulte’s laboratory, explains that this is the first time a property integral to cancer cells, rather than an injected dye, has been used to detect those cells. “The advantage of detecting a molecule already inside the body is that we can potentially image the entire tumor,” she says. “This often isn’t possible with injected dyes because they only reach part of the tumor. Plus, the dyes are expensive.”
Bulte cautions that much more testing is needed to show that the technique has value in human cancer diagnosis. His team’s next step will be to see if it can distinguish more types of cancerous tumors from benign masses in live mice.If further testing does show such success, Bulte and Song suggest the technique could be used to detect cancer at an early stage, monitor response to chemotherapy, guide biopsies to ensure sampling of the most malignant part of a tumor and eventually make at least some biopsies unnecessary.
Source: John Hopkins Medicine
27.03.2015