Credit: F. Hummel (EPFL)
News • Connectome analysis
Machine learning improves prediction of stroke recovery
An international team of scientists led by EPFL has developed a system that combines information from the brain’s connectome – the “wiring” between neurons – and machine learning to assess and predict the outcome of stroke victims.
When blood flow to the brain is somehow reduced or restricted, a person can suffer what we know as a stroke (from “ischemic stroke” in medical jargon). Stroke is one of those conditions that seems fairly common. This isn’t a misperception: just in Europe, there are over 1.5 million new cases each year.
Some strokes can be lethal, and when they’re not they often result in serious damage to the victim’s ability to move. In fact, stroke is one of the major causes of long-term disability today. Recovery can be a long and arduous road. Again, in Europe, under 15% of the patients achieve full recovery, leaving 3.7 million patients with persistent impairments. Clearly, this is a medical problem that needs urgent addressing.
But rehabilitation is a complicated problem to solve. Strokes can occur in different parts of the brain, affecting different brain systems, and patients who undergo rehabilitation show a “heterogeneity in outcome”, which is the medical way of saying that recovery can be very different between individual stroke victims. “The key is to find the optimal neuro-rehabilitative strategy to maximize individual treatment outcome,” says Professor Friedhelm Hummel, a neuroscientist and Director of the Defitech Chair for Clinical Neuroengineering at EPFL’s School of Life Sciences. “If we want to address these challenges in everyday clinical practice, we have to first enhance our ability to predict the individual courses of recovery,” adds Dr Philipp J. Koch, the study’s first author.
Hummel has now led an international team of scientists into a new approach for outcome prediction that can significantly improve stroke treatment. Publishing in the journal Brain, they demonstrate a predictive method based on two powerful, cutting-edge tools: connectomes and machine learning. The team included scientists from Sungkyunkwan University School of Medicine (Professor Y.-H. Kim), University Medical School of Geneva (Professor A. Guggisberg), Inserm Paris (Professor C. Rosso), Santa Lucia Foundation IRCCS, Rome (Professor G. Koch), and EPFL (Professor Thiran).
What is a connectome? Simply put, it’s a map of a brain’s wiring. The term itself was coined independently in 2005 by two scientists (one from Lausanne’s University Hospital) to describe the “blueprint” of how a brain’s neurons connect to each other, evoking the concept of the genome – hence, “connectome”.
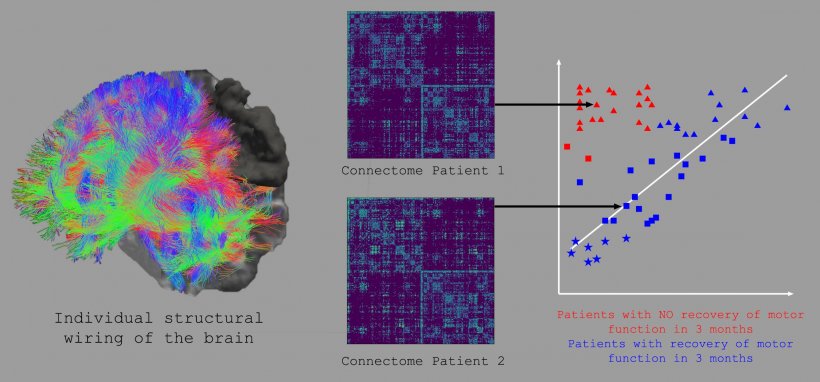
Credit: F. Hummel (EPFL) © 2021 EPFL
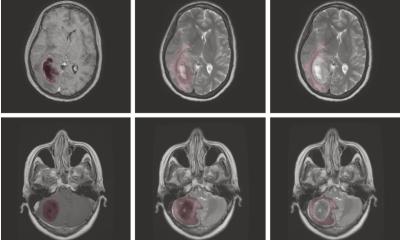
Connectomes are generated by analyzing multiple images taken from magnetic resonance imaging and reconstructing the brain’s structural or functional wiring non-invasively and in vivo. Today, connectomes are indispensable tools for neuroscientists, especially when they want to interpret structural or dynamic brain data and associate them with functions, functional deficits, or recovery processes. In short, the connectome shows how the brain is wired to control the body and its functions, which makes them important for working out the best recovery approach for a stroke victim.
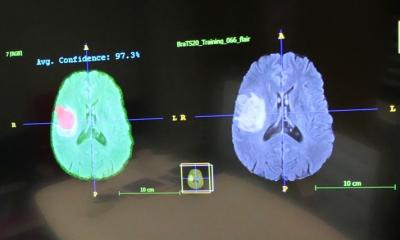
In the study, Hummel’s group analyzed connectomes from 92 patients two weeks after the stroke, tracking connectome changes up to three months later while assessing motor impairment with a standardized scale. This allowed them to monitor connection changes in the individual brains of the patients while they underwent recovery. The scientists input the connectome information into a “support-vector machine”, or SVM, which is a type of machine-learning model that uses examples to map an input onto an output. SVMs are particularly useful for classification, where they tell things apart and categorize them appropriately, e.g. spam and non-spam email.
In this study, the researchers trained the SVMs to distinguish between patients with natural recovery from those without based on their whole-brain structural connectomes. The SVMs then defined the underlying brain-network pattern of each patient, focusing on those who were severely impaired to make predictions about their recovery potential, with the accuracy of each prediction cross-validated internally and externally with independent datasets. The result is a cutting-edge tool of personalized medicine: a machine-learning system that can identify neuronal network patterns to make high-accuracy predictions on the outcome of recovery for stroke patients. “This tool can support the prediction of individual courses of recovery early on and will have an important impact on clinical management, translational research, and treatment choice,” says Hummel.
Source: École polytechnique fédérale de Lausanne (EPFL)
12.07.2021