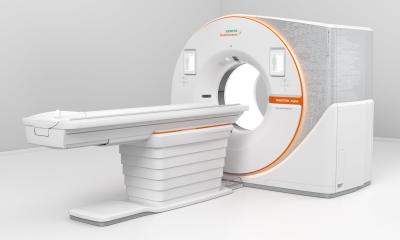
Fusing images from different sources
Okan Ekinci, Global Director of Cardiology at Siemens Healthcare, is convinced that, ultimately, ultrasound will remain the ‘entry level’ imaging procedure for patients. European Hospital met up with him at this year’s ESC congress to hear his thoughts on the potential of ultrasound – and particularly its fusion with other imaging modalities.
‘Ultrasound will not become obsolete – to the contrary,’ confirmed Okan Ekinci, Siemens Healthcare’s Global Director of Cardiology. ‘Because the modality is continuously developing, and more ultrasound scanning is actually done from inside the body, the significance of this modality is increasing.’
He also believes that three important points will also make ultrasound indispensable in the future – the costs, which are lower than those for any other imaging modality; real-time images, which facilitate conclusions in real time, and finally the ability to fuse ultrasound images with other imaging modalities. Helped by adapted software algorithms for image reconstruction and processing, data from almost all imaging modalities can be fused with one another. This makes fusion a technological reality utilised by various types of users to a different extent. ‘The hype around visual fusion seen a few years ago has calmed down somewhat. Now it’s all about proving the clinical added value.
‘One exciting trend,’ he added, ‘is the generation of new information through the fusion of image data from different modalities and through modelling.’ One graphic example of this is the fusion of ultrasound scans that visualise the movement patterns of the heart in high temporal resolution with the anatomical precision of CT scans. During the fusion process the images are increasingly not only being visually fused, but complex threedimensional flow patterns can be shown, which are not measured but calculated.
‘The basis is complex cardiac computer modelling, in this case fed from high resolution CT information – such as the ventricular cavity shape, wall thickness - and functional information such as heart muscle movement and valve function, from the ultrasound scan.’ Similar to a car no longer needs to be tested in a wind tunnel because the aerodynamics can be calculated via a computer based on established principles, he explained, heart modelling enables information to be gained about the entire flow pattern in a patient’s heart. ‘The virtual heart model will not only enhance diagnostic opportunities but also revolutionise the optimisation of treatment planning.’
Designed with continuously increasing attention to detail, he pointed out that models of the heart could make it possible to predict the effect of interventions on heart function and morphology with sufficient accuracy. A surgeon or cardiologist could, for instance, use the model to simulate how the heart will ‘react’ to the implantation of different heart valve models and sizes, possibly reducing the occurrence of paravalvular leaks or other complications. This enhanced choice of valves would constitute personalised medicine in the best sense of the term.
Dr Ekinci sees great potential for the ‘virtual heart model’ as well as Cardiac Resynchronisation Therapy (CRT). Patients with heart failure (HF) are often given a pacemaker to help synchronise the pumping function of right and left ventricles. Even when implanted according to guidelines, up to half of those patients do not respond to treatment. ‘Many factors can impact on therapy response,’ he stressed. ‘One is that many patients have CRT devices implanted in parts of the heart muscle affected by scar tissue, where no electric impulse can be transmitted. However, it also depends on the size and transmural extent of the scar where the best place for implantation would be. A personalised heart model, taking into account the complex, electrophysiological effects of a scar, could predict the success of CRT even before an intervention and therefore improve patient selection.’
This would not only lower treatment costs but also the rate of complications for implanted pacemakers. Dr Ekinci believes the fact that each imaging modality can test its strengths with the modelling approach is also an advantage: ‘Modelling and simulation of the integrated view of data from different sources means a new era for imaging, and we are very motivated to generate new and novel informa tion from the data measured. In the future, imaging will not only be restricted to the visualisation of the “best possible” images, but will revolve around extracting as much information as possible from data integration – for the advantage of patient and examiner.’ Not least, these procedures should also help to drastically cut exam times and time to diagnosis.
A further, still relatively new procedure to deliver real-time images from inside the heart in 3-D is the ultrasound catheter AcuNav V. With a diameter of only a few millimetres, the system is inserted through vessels in the groin to reach and be positioned in the atria or ventricles. For many cardiac procedures this would provide an unlimited view of the exact location where an intervention is being performed. ‘Particularly with electrophysiological procedures or TAVI, cardiologists ideally would like to know in realtime where they are and what they are doing,’ Okan Ekinci explained.
The advantages of the new catheter system compared to conventional procedures such as the TEE transducer are obvious: With the AcuNav V the patient does not need a general anaesthetic and the procedure is only semi-invasive because the catheter can be inserted via venous access. ‘Previously, there was a lack of spatial orientation with catheter transducers. The AcuNav V now facilitates a 3-D view of the implantation area during the TAVI procedure. The orthogonal view of a newly implanted valve allows the search for paravalvular leaks.’
AcuNav V also has practical, procedural advantages: Many interventionists do not like the look of the voluminous TEE transducer on fluoroscopic images – therefore, a transducer of only a few millimetres in size, which can be manoeuvred quickly, is an advantage.’
To what extent cost savings can be achieved with the procedure remains to be proved. ‘On one hand the AcuNav V catheters are disposable,’ he said. ‘However, on the other, the fact that the procedure can be carried out under sedation rather than a general anaesthetic means there may be no need for the presence of an anaesthetist during an interventional procedure.’
19.11.2013