Video • Enhanced therapeutic delivery
Focused ultrasound shows promise for Alzheimer's treatment support
A recent preclinical study from scientists at Sunnybrook Research Institute, Canadian Blood Services and the University of Toronto has demonstrated that focused ultrasound improves the delivery of intravenous immunoglobulin (IVIg), a blood product composed of antibodies from healthy donors, previously shown to have potential in treating a subgroup of patients with Alzheimer’s disease.
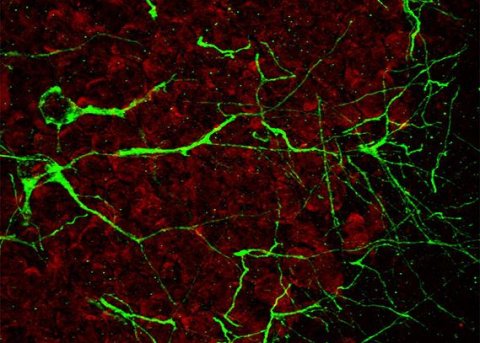
Image courtesy of Kate Noseworthy and Dr. Rikke Hahn Kofoed.
Alzheimer’s disease is a neurodegenerative disease that impacts 419,000 Canadians aged 65 years and older. By 2050, it is estimated it will affect more than 132 million individuals worldwide. Hallmarks of the disease include “plaques” and “tangles” composed of toxic protein that develop and eventually prevent areas of the brain from producing nutrients and sending signals involved in the health of brain cells. Over time, this causes deficits in cell-to-cell communication and functions, including difficulty in thinking and reasoning, confusion and memory loss. Without a treatment, brain cells will continue to degenerate and die.
“Intravenous immunoglobulin (IVIg), a therapeutic biologic composed of pooled antibodies from tens of thousands of donors, has been used to treat patients with various autoimmune and neurologic diseases since 1981 with high efficacy and safety,” says Dr. Donald Branch, a senior scientist with the Canadian Blood Services and professor in the Department of Medicine and Laboratory Medicine and Pathobiology at the University of Toronto. “IVIg has shown promise in reducing amyloid pathology in the brain and increasing neurogenesis,” says Dr. Sonam Dubey, who completed the study as part of her PhD work in Dr. Isabelle Aubert’s lab. “However, the properties of the blood-brain barrier make it difficult for sufficient amounts of IVIg to reach the brain.”
The blood-brain barrier surrounds blood vessels in the brain and restricts the passage of substances from the bloodstream to the brain. “We knew IVIg had potential for Alzheimer’s but, at the dosages used, it had failed to show significant improvement in clinical trials. We thought: how can we rescue it?” says Dr. Isabelle Aubert, Senior Scientist in the Hurvitz Brain Sciences Program at SRI and Canada Research Chair in Brain Repair and Regeneration. “How can we deliver more IVIg to the brain?”
Using preclinical models, the research team tested whether focused ultrasound combined with microbubbles, a non-surgical method used to briefly increase the permeability of the blood-brain barrier, could improve the delivery of IVIg to the hippocampus, an area of the brain involved in learning and memory and severely degenerated in patients with Alzheimer’s disease. “Our results show that focused ultrasound increased the bioavailability of IVIg from the blood to the hippocampus, where it reached therapeutic efficacy at a relatively low dosage given intravenously,” says Dr. Dubey.
The study paves the way for future clinical studies combining focused ultrasound and therapeutics, such as IVIg, for patients with Alzheimer’s disease. “We are extremely encouraged by these results. Over the years, both IVIg and focused ultrasound have been shown, independently, to be safe in humans. When IVIg and focused ultrasound are combined in models of Alzheimer’s disease, they reduce pathology and improve regeneration, says Dr. Aubert, who is also a professor in the Department of Laboratory Medicine and Pathobiology at the University of Toronto. “Based on these results, and with our colleagues and collaborators at Sunnybrook, we are well positioned to bring therapeutics and focused ultrasound together to the clinic, where it could become of benefit to patients in the future.”
Source: Sunnybrook Research Institute
09.12.2020