Clinical trial validates CT virtual colonoscopy
By Cynthia E Keen
When the International Agency for Research in Cancer (IARC) 2007 statistics report, showed that 429,000 new cases were reported in Europe in 2006, Director Peter Boyle recommended that colorectal cancer screening programmes be implemented throughout Europe.
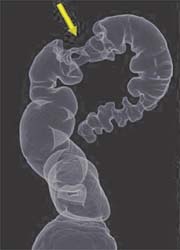
This disease is not fatal – if diagnosed in its earliest stages. Adults should have a colorectal screening examination from aged 50 and then every three to 10 years, based on their level of cancer risk. The barium enema and optical colonoscopy — traditional tests to identify polyps — are resource-intensive and time consuming. Traditional optical colonoscopy is invasive, usually requiring sedation and incurring a 1-in-1,500 risk of colon perforation.
Patients find both processes unpleasant, and many avoid screening. In the USA, for example, although there were over 112,300 new cases of colon cancer and over 52,000 deaths from this disease in 2007, the US Centers for Disease Control and Prevention reports that only 44% of individuals eligible for screening (about 70,000,000 people) had a screening examination.
From a hospital resource perspective, non-invasive CT colonoscopy, or virtual colonoscopy (VC), is a far more efficient alternative, as long as there are physicians qualified to interpret the procedure. With the proliferation of multi-detector CT scanners in hospitals and clinics, the ability to offer this procedure, by medical facilities throughout Europe, has increased significantly.
Two barriers have prevented widespread implementation: procedure cost and validation to show that VC has equivalent detection sensitivity. The publication in 2007 results from major clinical trials conducted in Europe and the USA have validated VC’s accuracy and effectiveness. In September last year, the preliminary results were announced from the National CT Colonography Trial, sponsored by the American College of Radiology Imaging Network (ACRIN) and funded by the US National Institutes of Health. ACRIN reported that VC procedures performed on 2,531 asymptomatic patients in 15 US academic hospitals and private practice imaging centres yielded a 90% per patient sensitivity for adenomatous colorectal lesions 1 cm or larger in diameter. This level of sensitivity was comparable with that of optical colonoscopy.
Presenting those results, C Daniel Johnson MD, Professor of Radiology at the Mayo Medical School, Rochester, MN, emphasised that rigorous reader training was an important component for the results. All interpreting physicians had to read 500 cases, or attend a 1.5 day training course, and also pass a certified examination consisting of 50 cases of mixed levels of difficulty.
The results of the Munich Colorectal Cancer Prevention Trial, first reported at the 2007 International Symposium on Virtual Colonoscopy (ISVC) held in Boston, Mass. in October, yielded 100% per patient sensitivity in identifying lesions 10 mm and larger. Sensitivity for polyps between 6-10 mm was 93.4% and 76.9% for lesions smaller than 6 mm. The 300 asymptomatic patients were given both optical colonoscopies and VCs using a 64-detector row Siemens Sensation CT scanner. The same radiologist read both studies, using a computer assisted detection (CAD) program with the CT scans. Dr Anna Graser, radiologist at the Grosshadern campus, University of Munich and principal investigator of this study, stated that the VC images enabled radiologists to identify clinically significant polyps nearly as accurately as optical colonoscopy. However, she cautioned that flat lesions were difficult to detect, as is the case with optical colonoscopy.
A clinical trial conducted at 12 medical centres in Italy, sponsored by the Societa Italiana di Radiologica Medical (SIRM), performed both optical and VC procedures on 934 asymptomatic subjects. Principal investigator Daniele Regge MD, radiologist at the Institute for Cancer Research and Treatment (IRCC) in Candiolo, a private, non-profit institution founded and supported by the Fondazione Piemontese per la Ricerca sul Cancro-Onlus, also presented preliminary results at the ISVC meeting. The research team determined that accuracy of VC ranged from excellent to acceptable.
This comparative trial assessed the sensitivity and specificity of VC in a population at increased risk for colorectal cancer. 40% of the participants had a family history of colorectal cancer or polyps, 36% had had a polypectomy, and 24% had a positive faecal occult blood test result. The 341 postpolypectomy patients represented one of the largest VC surveillance populations studied to date.
10 centres acquired images on 16-slice CT scans and two centres used 4-slice CT scanners. Of the 25 radiologists and gastroenterologists who participated, only five had read more than 500 VC examinations; 11 had read 50-100 and nine had read 100-500.
Dr Sarah Jane La’Porte, radiologist at Northwick Park & St. Mark’s Hospitals in Chesham, UK, presented at RSNA 2007 the experiences of her hospital’s conversion from barium enemas to VC for symptomatic and high risk patients. Over a nine-month period, she said, the 287 VC procedures were of adequate quality for interpretation. Detected cancers underwent immediate CT staging and these patients had an optical colonoscopy.
A study conducted at the University of Wisconsin Medical School in Madison, compared the results of VC screening of 3,120 consecutive adults with optical colonoscopy screening of a different group of 3,163 adults. Both groups were from the same general screening population and geographic region. The results (Pub: 4/10/07. New England Journal of Medicine) also found comparable results between the two types of procedures.
Cost-effectiveness - VC is still very open to evaluation. Radiologists at the Pitié-Salpêtrière Hospital, Paris, used simulation modelling over a 10-year period to assess the cost of faecal occult blood tests, optical colonoscopy, and VC for a virtual asymptomatic French population aged over 50.
Dr Medhi Cadi, who presented the results at RSNA 2007, said the team had presumed that 50% of the eligible population would present for screening. Assumptions were made that the optical/VC procedures would be repeated at 10-year intervals if negative, and after 3-5 years if positive with adenomas. The faecal occult blood tests would be repeated every two years.
Medical costs were based on 2007 French rates. The cost per individual over a 10-year period averaged ?885 for an optical colonoscopy, ?543 for a CT VC, and ?459 for faecal occult blood tests.
A cost-effectiveness simulation on a virtual population of 100,000 Italians was conducted at the Gastroenterology and Digestive Endoscopy Unit of Nuovo Regina Margherita Hospital in Rome: Lead author: Cesare Hassan MD. Based on 2006 Italian rates, all types of screenings were shown to save medical expenses, with the CT VC saving most, at ?48 per person compared with ?11 for an optical colonoscopy and ?17 for a flexible sigmoidoscopy.
The technology of CT colonoscopy, interpretation techniques, 2-D/3-D software and CAD for polyp detection is evolving rapidly. Hospital decisions to offer VC need determination by many factors. However, the good news is that, in 2007, important clinical trials have proved that VC provides another method to help reduce unnecessary death from colon cancer.
01.03.2008