News • Impact on mammography performance
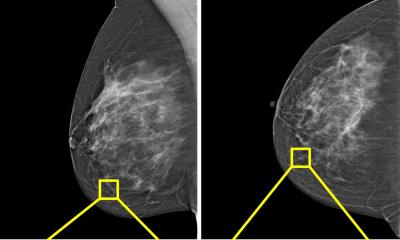
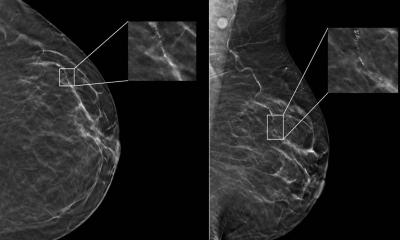
Breast cancer screening: better detection, fewer false positives with AI
Mammography successfully reduces breast cancer mortality, but also carries the risk of false-positive findings. In recent years, researchers have studied the use of AI systems in screening.
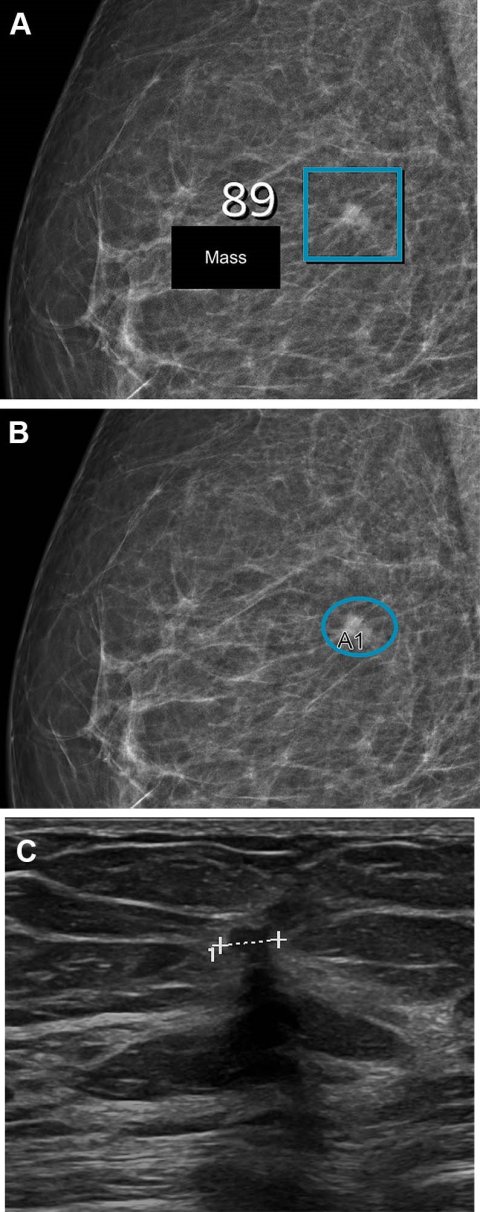
Image credit: Radiological Society of North America (RSNA)
Using artificial intelligence (AI), breast radiologists in Denmark have improved breast cancer screening performance and reduced the rate of false-positive findings. Results of the study were published in Radiology, a journal of the Radiological Society of North America (RSNA).
“We believe AI has the potential to improve screening performance,” said Andreas D. Lauritzen, Ph.D., a post-doctoral student at the University of Copenhagen and researcher at Gentofte Hospital in Denmark.
When used to triage likely normal screening results or assist with decision support, AI also can substantially reduce radiologist workload. “Population-based screening with mammography reduces breast cancer mortality, but it places a substantial workload on radiologists who must read a large number of mammograms, the majority of which don’t warrant a recall of the patient,” Dr. Lauritzen said. “The reading workload is further compounded when screening programs employ double reading to improve cancer detection and decrease false-positive recalls.”
Dr. Lauritzen and colleagues set out to compare workload and screening performance in two cohorts of women who underwent screening before and after AI implementation.
The retrospective study compared two groups of women between the ages of 50 and 69 who underwent biennial mammography screening in the Capital Region of Denmark. In the first group, two radiologists read the mammograms of women screened between October 2020 and November 2021 before the implementation of AI. The screening mammograms of the second group of women performed between November 2021 and October 2022 were initially analyzed by AI. Mammograms deemed likely to be normal by AI were then read by one of 19 specialized full-time breast radiologists (called a single-read). The remaining mammograms were read by two radiologists (called a double-read) with AI-assisted decision support.
Recommended article
Article • Lesion detection and mammographic texture analysis
Dual AI model to optimize breast cancer risk assessment
A team of Danish and Dutch researchers has combined an AI diagnostic tool with a mammographic texture model to improve the assessment of short- and long-term breast cancer risk. This new approach represents a significant step forward in refining the ability to predict the complexities of breast cancer risk.
The commercially available AI system used for screening was trained by deep learning models to highlight and rate suspicious lesions and calcifications within mammograms. All women who underwent mammographic screening were followed for at least 180 days. Invasive cancers and ductal carcinoma in situ (DCIS) detected through screening were confirmed through needle biopsy or surgical specimens.
Radiologists typically have access to the women’s previous screening mammograms, but the AI system does not. That’s something we’d like to work on in the future
Andreas Lauritzen
In total, 60,751 women were screened without AI, and 58,246 women were screened with the AI system. In the AI implementation group, 66.9% (38,977) of the screenings were single-read, and 33.1% (19,269) were double-read with AI assistance. Compared to screening without AI, screening with the AI system detected significantly more breast cancers (0.82% versus 0.70%) and had a lower false-positive rate (1.63% versus 2.39%). “In the AI-screened group, the recall rate decreased by 20.5%, and the radiologists’ reading workload was lowered by 33.4%,” Dr. Lauritzen said.
The positive predictive value of AI screening was also greater than that of screening without AI (33.5% versus 22.5%). In the AI group, a higher proportion of invasive cancers detected were 1 centimeter or less in size (44.93% vs. 36.60%). “All screening performance indicators improved except for the node-negative rate which showed no evidence of change,” Dr. Lauritzen said, adding that more research is needed to evaluate long-term outcomes and ensure overdiagnosis does not increase. “Radiologists typically have access to the women’s previous screening mammograms, but the AI system does not,” he said. “That’s something we’d like to work on in the future.”
It is also important to note that not all countries follow the same breast cancer screening protocols and intervals. U.S. breast cancer screening protocols differ from protocols used in Denmark.
Source: Radiological Society of North America
05.06.2024