Article • Study delivers screening advice
Breast cancer: Detection during, not between screenings is best
Tumours with the same biology have different prognoses based on their method of detection, and this information should be taken into account when deciding which treatments might be needed, a Dutch researcher explained at the 12th European Breast Cancer Conference.
Report: Mélisande Rouger

High-risk breast cancers detected in screening program mammograms have a better prognosis than those cancers detected in the interval between screening rounds, suggests an analysis of results from over eight years’ follow-up of a major international clinical trial. A team of Dutch researchers looked at cancers that had been identified as being high risk by the 70-gene signature test, but differed in the way they were detected, i.e. either during the biannual national screening program or in the two-year interval between screenings, typically when a lump or other abnormality is detected at the GPs and a mammography is prescribed.
The researchers compared the data of over 1,000 Dutch breast cancer patients aged 50-70 who had enrolled in a European phase III clinical trial and participated in the Dutch national biannual screening program. The authors found that although some tumours may have the same genetic make-up, the way they are detected makes a significant difference to the period of time before the disease starts spreading or results in death – a lapse of time known as the distant metastasis-free interval (DMFI). ‘We found a significant difference in survival between high-risk cancers detected during screening or in the interval between screenings. The eight-year DMFI rate was higher among women with screen-detected cancers than for women with interval cancers: 93.8% versus 85.2%,’ said PhD candidate Dr Josephine Lopes Cardozo at the Netherlands Cancer Institute (NKI) in Amsterdam, and medical fellow at the European Organisation for Research and Treatment of Cancer (EORTC) in Brussels. Additionally, those patients with high-risk tumours detected in the interval between screenings had a 2.4-fold increased chance of developing distant metastases compared to those whose cancer was detected during screening.
These findings complement previous research done by the same group showing that interval cancers more often have a high-risk genetic profile, as shown by the 70-gene signature, and are therefore at higher risk of distant metastases. ‘We know these interval cancers are more aggressive and thus also have a worse prognosis,’ Cardozo explained. ‘However, there are also screen-detected cancers with a high-risk 70-gene signature.’
MINDACT
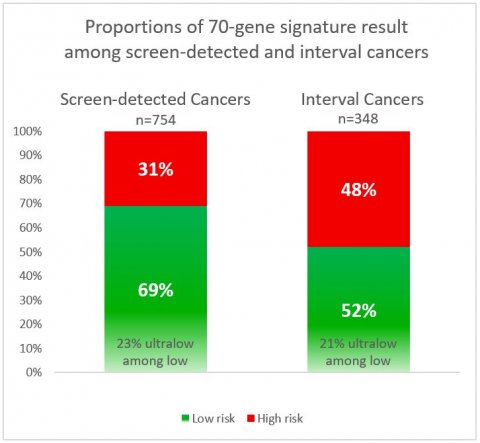
In their current work, Lopes Cardozo and colleagues looked at the data of 1,102 Dutch patients enrolled in the MINDACT study, a large prospective trial testing the 70-gene signature MammaPrint as guidance for adjuvant chemotherapy in breast cancer patients across nine European countries. The team calculated differences in DMFI for high, low and ultra-low risk tumours, as classified by the 70-gene signature, which looks at the activity of 70 genes in the breast cancer tissue. 754 cases were detected during screening and 348 during the interval between screenings.
The data indicated that 50% of patients reached at least 8.6 years of follow-up and there were 83 occurrences of distant metastases or death due to breast cancer. When looking at survival rates at eight years, researchers found that patients with screen-detected cancers had an eight-year DMFI rate of 98.2% in 118 women with ultra-low-risk tumours, 94.6% in the 398 women with low-risk tumours, and 93.8% in the 238 women with high-risk tumours. Patients with interval cancers had an eight-year DMFI rate of 97.4% in the 39 women with ultra-low-risk tumours, 92.2% in the 143 women with low-risk tumours, and 85.2% in the 166 women with high-risk tumours.
Towards tailored treatments
For patients with a very low risk of recurrence, longer follow-up may also help to identify those who are currently at risk of being over-treated
Josephine Lopes Cardozo
These results suggest that the method of detection is an additional prognostic factor in patients with high-risk tumours, and that the combination with genetic information may help to tailor treatment better for these and other patients, Lopes Cardozo believes. ‘The method of detection combined with the 70-gene signature can further optimise treatment for this group of patients who have a high risk of recurrence, the cancer researcher concludes, adding: ‘For patients with a very low risk of recurrence, longer follow-up may also help to identify those who are currently at risk of being over-treated.’
Profile:
Dr Josephine Lopes Cardozo is a PhD candidate at the Netherlands Cancer Institute in Amsterdam, and a medical fellow at the European Organisation for Research and Treatment of Cancer (EORTC) in Brussels, Belgium. Her lengthy interest in breast cancer continues with a focus on the role of the 70-gene signature for clinical decision-making in breast cancer, to evaluate how to select those patients who would benefit from adjuvant systemic therapies or not.
19.11.2020