Article • Superior in identifying cancers in symptomatic younger women
Breast cancer detection: advantage DBT
Digital breast tomosynthesis (DBT) increases detection of breast cancer in symptomatic women under the age of 60, especially in dense breasts. A large, multi-institutional study conducted in the United Kingdom comparing the sensitivity of full-field digital mammography (FFDM), DBT, and FFDM plus DBT supports findings of two similar published studies, both conducted in China in the same time frame.
Report: Cynthia E. Keen
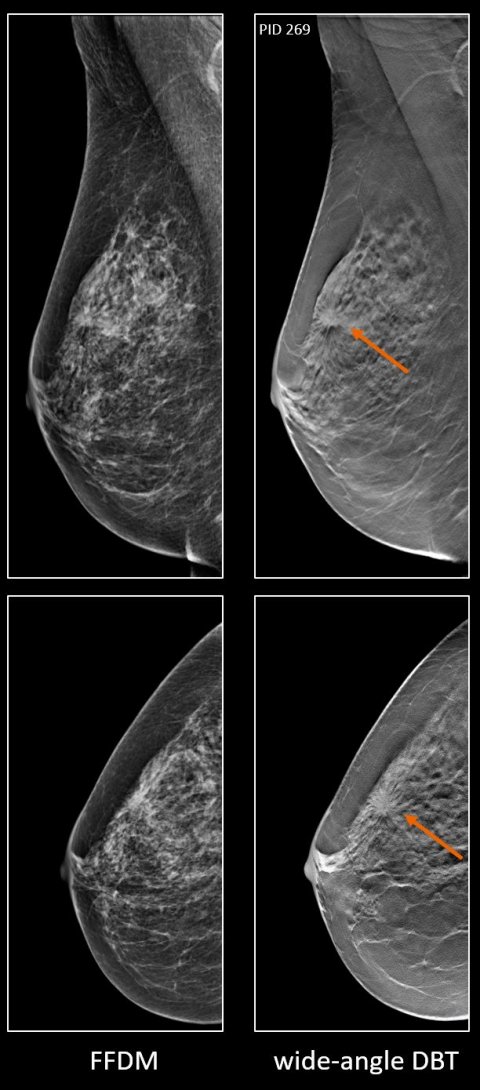
© Siemens Healthineers
Much research has been conducted to confirm the increased cancer detection capabilities of DBT technology as a breast cancer screening tool, but very little has been undertaken to evaluate and quantify the accuracy of DBT in symptomatic patients. The rigorous double-blind retrospective study, led by researchers at the University of Dundee in Scotland, utilized images acquired from a different mammography system than that used by the Chinese researchers. Because DBT technology differs significantly among vendors, findings of a single-vendor study are not necessarily generalizable when other equipment is used. This newly published study online in the British Journal of Radiology complements the research in China with similar data for a European population.
The participants included 300 women with symptoms or signs of breast cancer representing a 20% or greater likelihood of malignancy following a clinical examination. They had both FFDM and DBT at five U.K. hospitals’ specialist breast centers within a five year period starting in 2011. All sites used Mammomat Inspiration units from Siemens Healthineers. Images were acquired at all sites. The study cohort included all 152 women recruited who were diagnosed with cancer, plus a randomized selection of half of the 209 recruited women with benign lesions and half of the 76 women with normal breasts.
Mean age was 47 years, but participants were as young as 24 years. None of the patients had breast implants, as DBT had not yet been approved for use. Masses, at 89%, were the dominant radiological feature in malignant breasts, and 85% were unifocal tumors. The majority of cancers were Grade 3 or 2 invasive ductal tumors (42% and 33% respectively) and invasive lobular carcinoma (12%). Ductal carcinoma in situ (DCIS) represented only 1% of the 157 cancerous breasts.
Recommended article
Article • Alternative for mammography
Breast cancer screening: Does the future belong to the abbreviated MRI?
Is mammography still the best method for breast cancer screening? For a number of breast cancers, the latest scientific findings suggest otherwise. For more than a decade, Professor Christiane Kuhl MD, Director of the Clinic for Diagnostic and Interventional Radiology at the University Hospital RWTH Aachen, has researched the use of MRI in breast cancer screening.
Twelve breast imagers experienced with Siemens DBT independently analyzed a batch of 50 cases for each category, for a total of 150 readings, two readers per batch. Each batch had similar distributions of different aged patients, and cancerous, benign, and normal cases. To replicate real-life practice conditions, they were provided with the patient’s age and clinical records.

Image source: Siemens Healthineers
The imagers made their interpretations using FFDM images only, DBT images only, and FFDM+DBT images, marking regions of interest, measuring lesions they identified, and describing abnormalities. They scored suspicious lesions on a 1-to-5 scale (normal to malignant). For FFDM images, the readers categorized breast density using a BI-RADS️ density 1-4 category score, and used an on-screen 0-100 mm visual analogue scale to assign an area-based percentage mammographic density. The percentage of volumetric breast density was also assessed using Volpara️ Data Manager software (Volpara Solutions, Wellington, NZ).
Andy Evans, M.D., Professor of Breast Imaging at the University of Dundee and honorary consultant radiologist in NHS Tayside, and co-authors, compared the 1,800 case findings with the diagnosis of each patient, based on clinical exam, medical imaging, and histopathology. Readers identified 260 unifocal malignant lesions on DBT images compared to 214 on FFDM. The FFDM+DBT combined exams had the highest sensitivity in detecting breast cancer, at 97%, followed by 89.1% for DBT alone, and 86.6% for FFDM alone. In the densest breast category, FFDM+DBT identified 10.3% more cancers than FFDM alone, but DBT alone was most accurate for breasts in the third BI-RADS️ breast density category.
Overall specificity was highest for DBT alone (84.6%), followed by FFDM (81.4%), and then FFDM+DBT (79.6%). The researchers attribute the lower FFDM+DBT reader results as a function of needing to interpret two exams instead of just one. Tumor measurement accuracy was comparable for all three groups.

Based on their findings, the authors recommend that DBT be used for symptomatic younger women with known very dense breasts, or as a second-line exam following a negative FFDM. And in view of increasingly available contrast-enhanced digital mammography (CEDM), they also recommend that the performance of DBT be evaluated in clinical studies with this breast exam. “With respect to additional research, the Dundee team is currently conducting a UK multicentric study called CONTEST, comparing the diagnostic accuracy of CEDM with FFDM, DBT and MRI,” lead author Patsy Whelehan, a researcher at the University of Dundee School of Medicine and at consultant radiographer at NHS Tayside, tells Healthcare in Europe. “The study started as single center in 2018, but we now have several centers on board and recruitment is ongoing. Another major current UK-wide project from the Dundee team is MEDICI, which aims to assess whether a reduction in mammographic density in women taking adjuvant endocrine therapy following breast cancer surgery is associated with a lower risk of recurrence and/or a lower risk of dying.”
Profile:
Patsy Whelehan has been conducting clinical breast imaging research in Dundee with Professor Andy Evans since 2009. Her previous roles include leading the mammography training service at King’s College Hospital in London. As well as radiology research, she has a strong interest in patient experience in mammography. Clinically, she exemplifies the extended role opportunities available to radiographers in the U.K., whereby with rigorous additional training radiographers may undertake advanced practice such as reporting mammograms and performing breast biopsies.
04.03.2021





