Bootcare by Telemedicine
Mobile healthcare is a major buzzword nowadays: take the devices and the data to the patient, not the other way round. Mobility in this concept is not restricted to the hospital where devices and data flow freely from department to department, but encompasses follow-up care at home.
Report: Anja Behringer
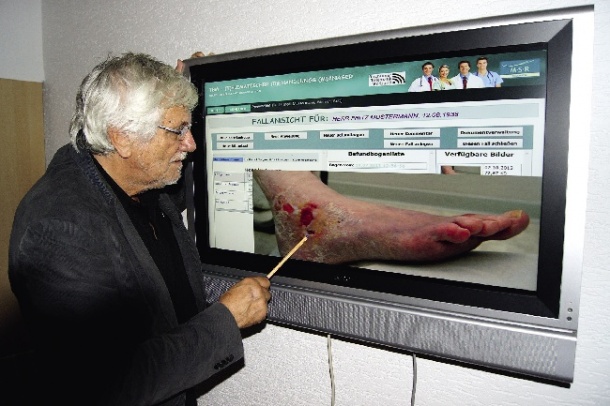
Whilst wound management has not been a major focus of telemedicine, it can benefit immensely from mobile devices – they support digital wound documentation to make wound management safer, more efficient and more cost-effective.
By law, wound documentation, which describes all criteria relevant for therapy planning, performance, control and follow-up, as well as prognostic evaluation, to ensure that approved medical and care procedures are being followed. However, beyond any legal aspects, written wound documentation is an indispensable quality control tool, since the differentiated parameters provide a detailed picture of the individual wound situation that can offer guidance for all parties involved in therapy and care.
Dr Bernhard Clasbrummel, Director of the Clinic of Orthopaedics and Trauma Surgery Zollernalb in Balingen, Germany, has been interested in telemedicine since it first appeared on the healthcare scene about 15 years ago. Still enthusiastic about the technology’s potential to change the prevailing healthcare paradigm, he also has a clear view of the realities: while the cost advantages of telemedicine in wound management are praised unanimously, mobile technology has yet to conquer everyday clinical practice and routine. We asked the expert – who had used telemedicine resources for wound management ten years ago on the Spanish island of Mallorca – to answer three questions, beginning with which manufacturer he works with in telewound care.
‘Our applications are manufacturer-neutral. Many big manufacturers do not invest in this issue. We save the wound record on a web-based platform that can be accessed and used by everybody involved,’ Dr Clasbrummel explained.
‘Firstly, wound documentation ensures information flow between physicians and nurses and thus ensures that no contradicting measures are taken, no matter who performs the wound care at any given point. Secondly, written wound documentation plays a major role when liability issues arise regarding the medical or care services. Next, verbal agreements, for example those made in shift or ward meetings, do not satisfy the legal quality of care requirements.
‘A precise initial wound assessment, the basis of the wound documentation, will promote urgently needed interdisciplinary cooperation. If, for example, the development of a diabetic ulcer is detected, coordinated action by diabetologists, angiologists and surgeons can prevent major interventions such as an amputation.
What’s new in modern wound management?
‘Telewound care is still new. 15 years ago, although all those involved welcomed it, nothing much has happened since 2000. Despite the fact that theoretically telewound management is widely accepted, in practice there is no significant progress because nobody wants to pay for it. The medical advantages are undisputed, but without money nothing happens. A wound costs between €4000 and €5000. Ideally, you have two physicians from different disciplines – without doubt a pretty costly approach, but if you take a closer look you’ll see major long-term benefits: your outcomes are much better, there’s faster healing, shorter length of hospital stay, top quality, satisfied patients, and all this will be unambiguously documented and accessible in your digital wound record – but, every society has to decide how much health it can afford.
‘The meticulous collection of data for wound documentation forces physicians and nurses to work systematically and look at the individual wound situation precisely and in-depth. Using more than a dozen differentiated and tried and tested wound parameters, data are collected and a confident assessment of progress, stagnation and setbacks is possible. Consequently well-founded decisions on therapy adjustments, which may spare a patient from enormous suffering, can be made.’
Envisioning the future of telewound management
‘Today, we only have documentation models but no payment models. I’m confident, however, that eventually professional wound management will be paid for separately, particularly in out-patient care.
‘Above all the GP needs solid documentation, which can be assessed when need be by a relevant specialist physician. We simply need to ensure that such a cooperative system can function without a hitch. Due to the major social impact, correct wound documentation should be mandatory.’
PROFILE:
In 1991, after Private Docent Bernhard Clasbrummel MD graduated in medicine in Freiburg, he trained as a surgeon at the Bergmannsheil hospital in Bochum’s Ruhr University and, in 1994 founded the working group Clinical Microsystems Technology. From 2000 to 2005 he was speaker for the Telemedicine Centre of Excellence Teltra (Gesellschaft für telematische Traumatologie mbH). He was appointed Medical Director at Evangelisches Krankenhaus Witten in 2006 and, since 2009, has been Medical Director of the Clinic of Orthopaedics and Trauma Surgery in Balingen, Germany. Currently he focuses on clinical care in a regional trauma centre, including the clinical assessment of telemedicine projects.
18.11.2013