Source: Shutterstock/Stokkete
Article • Telemedicine
COVID-19 pandemic expedites a cultural change in healthcare
The pandemic has sparked a cultural change in healthcare and telemedicine use will increase much faster than planned in the near future, according to Vicent Moncho Mas, IT Director at Denia Marina Salud Hospital near Alicante, Spain.
Report: Mélisande Rouger
Spain is being particularly affected by the pandemic, but its impact on hospitals differs considerably across the country. Unlike many institutions in Madrid or Barcelona, which had trouble coping with the patient flow at first, hospitals like Denia Marina Salud Hospital near Alicante, a popular sea resort south of Valencia, have remained afloat since the beginning of the pandemic. “We have free beds inside the intensive care unit. Our hospital has 220 beds and only 110 are now taken. We have about 30 patients visiting the emergency department per day compared with 150-200 usually, because people are afraid of coming. They also have less injuries as a result of the lockdown,” Moncho said.
Marina Salud is currently treating 160 patients who tested COVID-19 positive, but only 45 have been admitted to the hospital and ten are in the ICU (as of April 8th). The rest are being followed up from home, just as 950 other patients throughout the area.
Moncho and his team had time to organize their strategy to best deal with the pandemic. The experience previously acquired by those hospitals whose emergency services reached saturation early on proved crucial to help prepare adequately.“Our colleagues from Torrejon University Hospital in Madrid shared very valuable information, notably on how to harness patient clinical records and make them available remotely to physicians within 48 hours,” he said.
The deployment of telemedicine, which had been partly implemented in recent years, has been a determining factor in helping the emergency department remain up and running.
Adapting existing tools to a large strategy

Marina Salud prepared for the switch to teleworking on March 13th, a few days before complete lockdown in Spain. Moncho’s impulse was to move the whole IT department, which is located near the emergency room, outside the hospital, to provide free space for patients with COVID-19 or with suspicion. “The transition went smoothly, as we were finalizing two onsite projects - a checking, ticket-based system for outpatient consultation and a project for radiological examinations,” he said.
The VPN had been running since 2009 and proved essential to the operation. The system hadn’t been fully implemented, but it already had many users. “Especially heads of departments valued the tool from the beginning in 2009, to check waiting lists and prepare for surgery, for example. Once we started to work during lockdown, all the other physicians started to use the service very quickly,” he said.
A few days later, outpatient consultations were paralyzed, as up to 900 patients per day came to the outpatient area. The challenge then was to quickly connect doctors who usually attend 90% of their patients on an outpatient basis. “We had to connect them quickly to patient clinical records, so that they could also start working from home,” he said.
Most hospital consultations were then attended on the phone. Physical appointments were only booked when cases couldn’t be solved directly on the phone.
Part of the staff had already been using Zoom for online conferences. The hospital also used another web-based program which is similar to Google Drive and integrated into the PACS, to enable patients to access their radiology studies with a short URL and a PIN code. “We realized and exploited the potential of the tools we already had for virtual patient consultation, for example to provide patients with medical reports or recommendations during their physiotherapy. We filmed physiotherapists showing to teach patients how to do their exercises from home, as in a personalized tutorial,” he said.
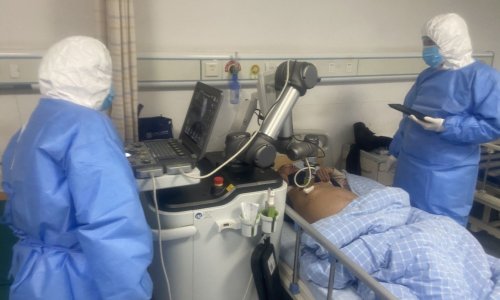
An issue for many patients with COVID or suspicion of COVID is that they are confined in the hospital or ICU and can’t have any visitors. Marina Salud therefore provided smartphones to the nurses to carry out video calls with the patients’ families and facilitated tablets or chargers to help patients stay connected with their loved ones. “A lot of patients did not have time to pack a charger or didn’t have their phone with them when they were admitted to the ER. Having a connection to the outside world is important, especially for elderly patients or patients inside the ICU. Nurses assist and install the equipment for the call whenever needed. Patients can also access all TV programs on the tablet, so they don’t have to watch hospital TV where it’s all depressing COVID news,” he said.
Towards a cultural change in healthcare
The pandemic has highlighted the value of telemedicine as a way to save time and money. Patients have acknowledged the potential and this new perspective will help bring change much faster than expected, Moncho believes.
“The Covid-19 crisis is expediting a cultural change in healthcare that might have taken 5 to 7 years. Now things are going to go much faster because patient acceptation has increased. Things move much better and quicker when patients lead change,” he said.
Physicians who have long resisted the change to telemedicine will be more inclined to use this type of services now that they know their patients’ opinion. “There is always resistance to change. Patients had never been asked what they wanted and physicians hadn’t had the opportunity to try these services. Now they have,” he said.
Although there will be a learning curve to use these tools properly, patients and physicians understand more acutely the benefit of saving time and not having to go to the doctor’s office if it is complicated for them to do so, he added.
The Denia Marina Salud Hospital has just started to assess telemedicine opportunities and will come up with a new agenda for outpatient consultation using virtual tools by August, when things cool off. “It will be interesting to define which patients need to come to the hospital and who can stay home and be attended virtually, depending on their pathology, age, condition, etc. We’ll have to think about that for the next few months,” he said.
In the long run, it will be interesting for Spain to develop a national strategy for telehealth, notably to share the electronic patient record (EPR). “Right now we have 17 autonomous regions each with their own healthcare systems and different levels of maturity, sometimes even within the same region. With the pandemic, people understand that things have to change and that we need a centralized initiative,” he concluded.
PROFILE:
Vicent Moncho is the Director of the Information Technologies and Systems at Denia Marina Salud Hospital. He is also a member of the executive committee of Marina Salud SA and a contributing professor at the Universitat Oberta de Catalunya.
16.04.2020