Bariatric surgery: A last resort -- or the only way to go?
More than half of the European population is overweight, or worst, obese. When diet and lifestyle changes do not result in permanent weight reduction in obese patients, bariatric surgery is now considered a final option. But, that’s far too late, says Professor Rudolf A Weiner, head of the surgical department at Sachsenhausen Hospital in Frankfurt/Main, Germany, and President of the German Society for Surgery for Obesity.
Report: Karoline Laarmann

Although surgery is mostly the ultimate step after a long chain of therapy measures, he believes it to be the only treatment that actually delivers long-term success -- and effectively reduces treatment and post-treatment costs.
‘Obesity is a chronic disease which today – just like diabetes mellitus – is not curable,’ points out Professor Weiner, President of this year’s World Congress of the International Federation for Surgery of Obesity and Metabolic Disorders (31August - 3 September. Hamburg, Germany). ‘We can try to manage overweight and moderate obesity with conservation therapies. However, as far as extreme obesity is concerned, bariatric surgery is the only method that shows long-term success. Conservation therapies can only support successful surgery, never replace it.’
What he deplores is that, in Germany, this proven fact is widely ignored, and thus many patients undergo surgery too late. When bariatric surgery is performed, patients are older and, on average, their body-mass index (BMI) is seven points above that of patients in other European countries. At that stage many patients already suffer severe medical conditions: only 15% of German patients undergoing weight-loss surgery have not yet developed severe co-morbid conditions, compared to 40% internationally. At the same time, the guidelines are unambiguous: with a BMI <35 kg/m² accompanied by severe co-morbid conditions and a BMI <40 kg/m² without co-morbid conditions only surgical intervention has proved really effective.
The International Diabetes Federation new research indicates that, in certain cases, bariatric surgery can also be considered for patients with a BMI of 30 to 35 kg/m² with Type 2 diabetes that is difficult to manage and who did not respond to conservation measures. However, this innovative approach is highly controversial. Its critics oppose the manipulation of healthy organs.
Nevertheless, diabetologists increasingly support bariatric surgery. ‘Today, surgical procedures are extremely safe; in a high-volume surgical centre morbidity rates are between 0.1 to 0.1% – much lower than for gall bladder or hip surgery. Meanwhile morbidity among patients who do not undergo surgery increases by 100%,’ as shown in a 2005 Canadian study by Raj S Padwal.
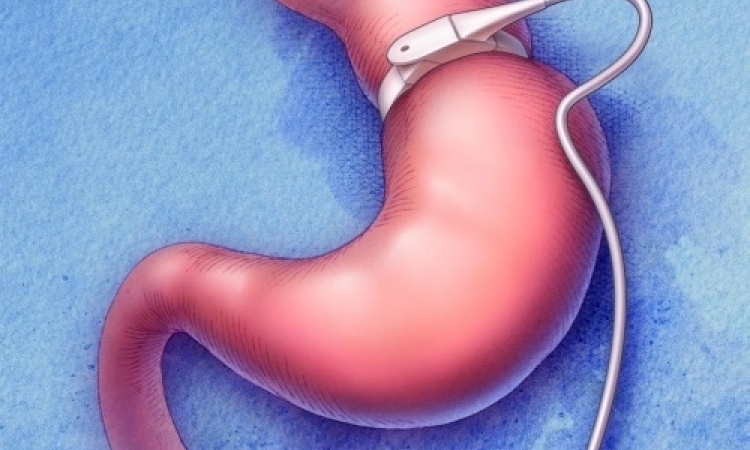
Bariatric surgery in children and adolescents is also hotly debated. Professor Weiner, who has performed bariatric surgery in 84 patients under 18 years in the past decade, strongly advocates surgery at an early stage. For young patients, however, he recommends reversible procedures such as gastric bands, which do not change a patient’s anatomy.
The decision for a certain therapy is based on the patient’s individual risk profile, which considers factors such as current body weight, weight history or co-morbid conditions. Moreover country-specific differences can play a role in the selection of the appropriate therapy as Professor Weiner points out: ‘This has socio-economic reasons. In Germany, you can observe a trend away from gastric banding towards bypasses, while in the USA gastric banding is gaining ground due to the fact that it has passed official approval procedures. In addition in Germany, the number of tube gastrectomies has reached its apex. In this intervention, the fundus of the stomach, where the appetite-stimulating hormone ghrelin is produced, is partially removed. After this intervention the patient feels less hungry and can intake only a certain amount of food. In other countries the so-called gastroplication is increasingly performed, which means the size of the stomach is reduced by suturing or removing a stomach fold.’
As a rather young medical discipline, bariatric surgery will no doubt offer interesting surprises and developments in procedures and applications.
IFSO 2011 this summer offers a forum for experts to discuss the future of surgical weight loss interventions.
14.06.2011