VuCOMP takes lead in aiding diagnosis of breast cancer
It may well be the first computer-aided detection (CAD) software that went to school with radiologists to study breast cancer.
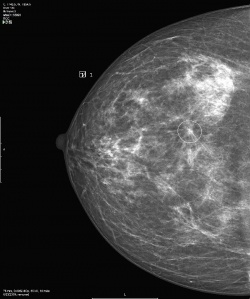
On the second day of RSNA, VuCOMP won approval from the U.S. Food & Drug Administration (FDA) for the third version of the M-Vu CAD, the industry leading technology for assisting radiologists by automatically identifying areas of a mammogram that are consistent with breast cancer. The updated software is available immediately, and for free, to existing customers.
In fact, CEO Jeff Wehnes was celebrating a series of success at RSNA. Fujifilm agreed during the congress to include M-Vu as a companion technology of the Aspire mammography systems, making M-Vu CAD immediately available through Fujifilm’s U.S. distribution network.
Since the break-through approval by the FDA for the first version of M-Vu 13 months ago, VuCOMP has been integrated on board digital mammography systems manufactured by Carestream, GE, Giotto, Hologic, Konica Minolta, Philips, Planmed, and Siemens, more than twice as many vendors as any other mammography CAD product.
During RSNA, VuCOMP also announced an expansion of its product portfolio with M-Vu Breast Density. Used in tandem with the M-Vu system the Breast Density component responds to a growing legal requirement in 13 U.S. states to provide women with a rating of their specific breast density.
Using advanced computer vision algorithms, the add-on software module analyses a mammogram to find dense areas that may have a higher risk of masking cancer. By calculating the percentage of breast area that is dense and converting it to one of four density categories corresponding to the BI-RADS standard, radiologists are better able to advise women of a need for additional examination using alternative diagnostic modalities, such as ultrasound.
While VuCOMP is suddenly on a roll, Wehnes said that convincing radiologists to use CAD assistance in reading mammograms continues to be an uphill climb requiring teaching and preaching, thanks to the poor experience most doctors had with the first wave of CAD software 10 years ago.
"It requires a lot of education with customers, particularly in Europe," he said, explaining that starting as early as 2000, European radiologists were early adopters for CAD but quickly became disappointed with the high rate of false positives.
"Among the early CAD systems, the rate of false positives was so high, radiologists got tired of seeing these marks on mammograms. The biggest challenge we have is convincing doctors we have new technology that greatly improves CAD and will make them want to use it," said Wehnes.
"There are fundamental differences in the approach we take," he explained. "It requires that our engineers thoroughly understand problems from a doctor's perspective. For example, what is it about normal tissue that makes it look normal?"
"We have to go through the same training as doctors do in order to read mammograms, and then we have to define all of the concepts for spiculation, asymmetry, irregularity or an unusual degree of uniqueness, and then develop mathematical formulas to represent each concept," he said.
"This is what allows us to be able to find cancer," said Wehnes. „I don't know of any other products out there, even in other fields of computer assisted recognition that take our approach."
by John Brosky
03.12.2013