'Treat first what kills first'
1,500 international trauma surgeons descended on ECTES and WTC 2014
There is room for worldwide improvement of trauma care, as Congress President Professor Ingo Marzi, Frankfurt/Main (Germany), emphasised.

Although road traffic deaths – around 1.25 million annually – are declining in countries where the comprehensive care pathway, from pre-hospital through emergency and primary surgical care has been optimised, the logistics, procedures, workflows and resources remain insufficient in many regions.
During our EH interview (see underneath), Professor Luke Leenen, Utrecht (Netherlands), President of the European Society for Trauma and Emergency Surgery (ESTES), elaborated on the significant differences in trauma care within Europe. The European umbrella organisation ESTES brings together 30 national professional associations in trauma care and emergency surgery representing more than 10,000 members.
All diagnostic and therapy measures in trauma care aim at speedy vitalisation and maintenance of functionality. This, according to Pol Rommens, Mainz (Germany), requires the first caregiver to do a primary survey, a quick but nonetheless comprehensive assessment of the trauma pattern. An in-hospital examination, including imaging, is followed by primary life-saving surgical care of the trauma patient. A final care plan can only be designed and implemented after the patient has achieved a certain degree of stability.
At ESTES, Professor Reinhard Hoffmann, Frankfurt/Main (Germany), looked at the principle ‘treat first what kills first’. Hoffmann, Secretary General of the German Trauma Society, confronted the fictional ‘Emergency Room’ image of daily work in a shock room with the reality. No doubt, he conceded, time is of the essence in any medical emergency, but work in a shock room is far from chaotic. To the contrary; headed by a trauma leader, a life support team applies minutely designed and highly standardised procedures. Certified trauma centres comply with the care algorithms defined in the Advanced Trauma Life Support (ATLS) programme, including the so-called ABCDE process, a step-by-step diagnostic assessment, and diagnostic imaging.
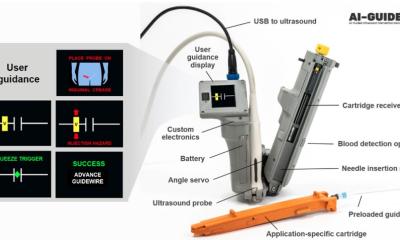
However, the actual contents of the initial care procedure implemented in a trauma centre can vary greatly, depending on the available infrastructure and individual hospital environment. In Germany, for example, diagnostic peritoneal lavage has almost entirely been replaced by ultrasound. Today, Focused Abdominal Sonography for Trauma (FAST) is the routine, first-line, diagnostic procedure in almost every shock room. Additionally, in this and other ultrasound procedures the real work horse in any shock room is computed tomography (CT). Almost 75% of all trauma patients undergo a usually contrast-enhanced whole-body CT.
In the past decade the time-to-CT has been reduced from 40 to 20 minutes. In Germany, however, the costs for having both technology and staff on stand-by are neither recorded nor reflected in the diagnosis related groups (DRGs). In 2006, the German Trauma Network (TraumaNetzwerk DGU) was established to counter the reimbursement gap in polytrauma care, the reduction of staff in trauma departments and the care providers’ increasing focus on plannable and thus lucrative care options.
These networks, as Professor Bertil Bouillon, Cologne (Germany), President of the German Trauma Society, explained, managed to secure qualified care of acutely injured patients across the country. Today, the ‘relay’ of the different care systems from the site of the accident to a rehab centre can well be called high-end care, which not merely saves patients’ lives but also ensures the best possible quality of life later on.
According to Bouillon, it is the successful network structure that enables ambulance services, hospitals and rehab centres to provide such high-quality services. Like Professor Marzi before him, and moving beyond any professional turf wars in Germany, Bouillon acknowledged the crucial role of the trauma surgeon. However, despite the many improvements, a European-wide high standard of trauma care remains pie-in-the-sky as long as regions exist where accident victims have to be carried to the next hospital in a donkey cart.
18.08.2014