The potentiated value of MR-PET imaging
Even more precise diagnoses, even better process controls -- the future of MR-PET technology has dawned. The first commercial, full-body hybrid scanners are either waiting in the wings or already installed. But what does the introduction of the MR-PET really mean for clinical practice? Professor Heinz-Peter Schlemmer MD, Head of the Radiology Department at the German Cancer Research Centre in Heidelberg, sees enormous potential, particularly for oncology.
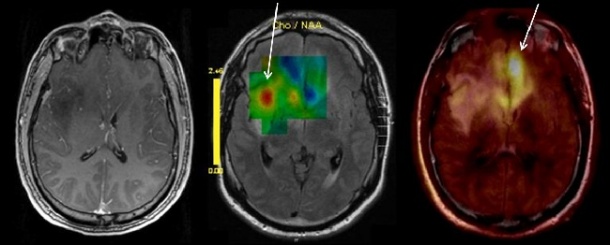
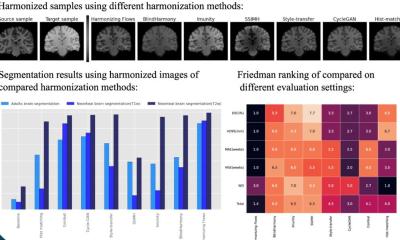
As Professor Heinz-Peter Schlemmer explains, MRI scanning offers functional methods that help to gain important information about blood supply, metabolism or movement of a tumour. ‘These biochemical and physiological parameters enable us to make conclusions about the aggressiveness of a tumour and are therefore important decision-making aids for treatment planning and process control.’ The image can safely confirm a suspected highly aggressive, malignant growth for many tumours, for instance brain tumours, liver tumours or prostate cancer. For many parts of the body, such as the brain, the abdominal and pelvic organs and the bone marrow, MRI is considered the most sensitive diagnostic imaging procedure.
High resolution PET scanning offers similar help for tumour diagnosis on a microbiological level. ‘Depending on the substance, the radiotracers fulfil different tasks. They accumulate in benign or malignant changes, bind to certain receptors at the cell surface or measure the process of substance absorption- and change in the cell. Therefore, whilst PET-CT shows a combination of anatomy (CT) and metabolism (PET), MR-PET allows us to show a combination of anatomy (MRI) and two sources for the determination of functional information, such as metabolic activity (MRI + PET). Future studies will show the extent of the benefit that can be derived from this potentiated imaging information,’ the professor points out, adding that a further advantage of MR-PET is the simultaneity of the examination. Unlike the PET-CT, which is carried out sequentially, this procedure guarantees a particularly precise spatial and chronological attribution of imaging information.’
A further important quality criterion compared to hybrid technologies such as PET-CT and SPECT-CT is and will remain that MR tomography can be carried out without exposure to X-rays. This significantly reduces the radiation dose for patients during the MR-PET examination, as the exposure caused by the radiotracers used for PET scanning is comparatively low – however, combined with CT it adds up to a not insubstantial overall dose. As functional imaging procedures are often used repeatedly for the individual control of treatment progress for cancerous diseases this additional exposure for patients has to be viewed particularly critically. It will not only be tumour patients in general but particularly young people -- down to the very youngest cancer patients -- who will benefit from the lower radiation exposure generated by MR-PET scanning.
‘With all this technological and medical finesse we must not forget that a PET – no matter whether integrated into a CT or an MRI scanner – is only ever as good as the radiotracers used with it. The PET itself only shows the spatial distribution of the radioactive substance or the marker. This is why the development of specific radiotracers with high sensitivity has an important, key function within the field of nuclear medical imaging procedures,’ Prof. Schlemmer points out.
Currently various radiotracers are being controversially discussed in terms of their therapeutic significance. However, when it comes to the development of new cancer medication, it is very important to document success and failure in the individual treatment of patients. The urgency of research into suitable radioactive probes is also reflected in the desperate search for qualified radiopharmacists. Prof. Schlemmer: ‘A good radiopharmacist can make the most hidden biochemical processes visible.’
However, as he points out, in the future specialists will be needed to evaluate imaging information from a MR-PET scanner. ‘Apart from a radiologist who is very familiar with MRI scanning, a nuclear medicine specialist familiar with PET scanning will also be required. Indeed, MR-PET scanning is a very extensive and complex examination, which requires a high degree of expertise but, on the other hand, it will result in enormous benefits for the visualisation of tumours.’
28.10.2010