Small silent VADs
Powerful tools to beat end-stage HF
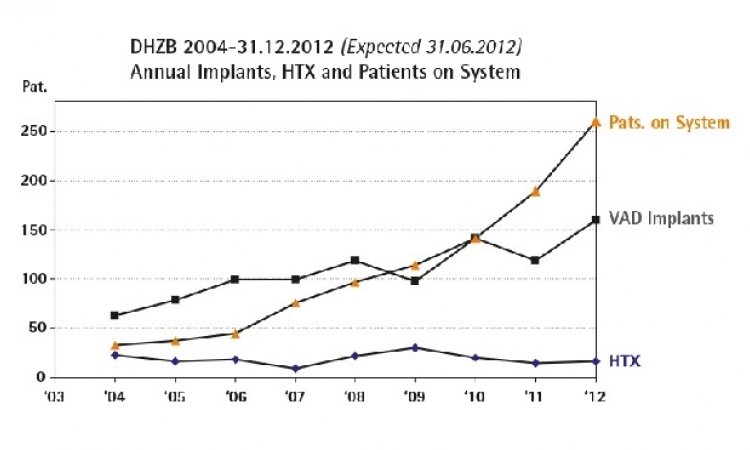
Ventricular assist devices (VAD) have been used since the 1980s, primarily to provide support after cardiac surgery for several days during recovery, or more often to keep patients alive until later heart transplantation (HTx).
This latter concept, named ‘bridge-to-transplantation’ (BTT), has saved many patients who otherwise would have died before a donor heart became available.
Organ failure from cardiogenic shock - brain, lungs, kidney, and liver - was reversed by VAD support, which only then made heart transplantation successful. Thus, in experienced teams, the results of HTx after BTT are the same as after primary HTx. However, with BTT the number of possible HTx is not increased.
The waiting time for HTx has now become as long as many months. This has allowed the observation of extended periods on VADs, which has led to two important concepts. First, some patients with acute myocarditis and dilated cardiomyopathy have displayed complete cardiac recovery after weeks and months of unloading of the heart with a VAD, which could then be removed, followed by stable heart function, up to now for over nine years. Such ‘bridge-to-recovery’ is excitingly attractive as a treatment concept; however, so far, recovery in the individual patient has remained unpredictable.
Second, long BTT waiting periods, improved VADs, high patient mobility and quality of life on VADs and the discharge of patients to home, then a return to work with a VAD have opened the view to permanent VAD support, and now an increasing number of patients receive VADs as ‘destination therapy’, either because of contraindications to HTx or due to a patients’ own wishes.
Some VADs have now been designed for permanent use and experience with this latter concept shows well-functioning devices in patients up to over six years.
Newly developed devices are smaller, need less energy, are silent and mostly follow the continuous flow principle. Expectations are justified that such VADs will become a powerful routine tool to battle end stage heart failure.
01.07.2004