Small bowel imaging
For gastrointestinal exams, MRI fluoroscopy offers an alternative to conventional methods of swallowing and gastric emptying that are so repugnant to patients.
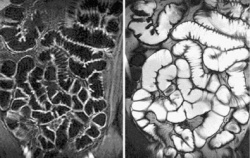
MRI exams eliminate radiation dose exposure, provide full views of soft-tissue structures, and produce multiplanar imaging. For radiologists, the value of MRI of the small bowel is its ability to display both morphology and motility. Small bowel motility (the bowel wall motions and contractions of muscles within the intestinal walls) dysfunction can be a symptom of inflammatory bowel disease, e.g. Crohn’s, obstructive bowel disease, diabetes mellitus and scleroderma (a disease of connective tissue that causes fibrosis to form). The standard protocol for MRI motility assessment begins with the acquisition of several coronal 2-D sequences over the entire small bowel using fast imaging pulse sequences, such as echo planar imaging, fast spin echo, or steady-state free precession.
Evaluating small bowel motility is tedious and time consuming. The quantification of small bowel motility patterns, such as contraction frequencies and amplitudes, can be made by measuring the cross-sectional diameter change of selected single small-bowel segments over time. That calculating and plotting measurements is so time consuming and susceptible to errors has formed one of the primary barriers against using MRI-assisted motility assessment in hospital radiology departments. The challenge is that all measurement points must be corrected due to the inherent modality movement or shifting of the small bowel segment.
Radiology researchers at the Institute of Diagnostic, Interventional, and Paediatric Radiology at University Hospital in Bern, with software engineers at Sohard AG in Bern, developed a software prototype (Motasso) to quantify small bowel peristalsis. The software permits semi-automatic measurements of small bowel diameter over long time periods, thus displaying motility.
With colleagues at Zütovh University Hospital, ECR session* presenters Doctors Michael A Patak, Sebastian Bickelhaupt and Johannes M Froehlich, conducted a study to validate Motasso software for small bowel motility tracking by comparing it with the traditional manual measurement method. In January, they reported their analysis of 45 MRI enterography exams online in Clinical Radiology.
The research team analysed 91 small-bowel segments. Small bowel motility parameters including contractions per minute, luminal diameter and amplitude were measured three times each in identical segments, using both manual techniques and the semi-automatic software assisted method. They compared the methods for agreement, repeatability, and time needed for each measurement.
The Motasso software worked very well. It produced standardised, accurate identification of the small bowel wall and subsequent quantification of small-bowel motility. It expedited measurement, and performed each assessment in half a minute compared to a minute and a half when done manually. It also provided higher reproducibility and standardisation of data acquisition made by different individuals.
‘Measurements with Motasso are faster, more accurate, and significantly more reproducible than measurements by hand. The user-friendly point and click interface facilitates widespread clinical adoption of the software,’ the authors wrote. They also believe that the Motasso software can provide new insight into the pathophysiology of small-bowel motility-related gastrointestinal complaints. Research is on-going.
06.03.2014