Quantitative PET imaging
Visual analysis of PET scans for non-Hodgkin lymphoma may be improved by using standardised uptake value in monitoring response to treatment, according to research published in the Journal of Nuclear Medicine.
Evaluating a patient’s response to chemotherapy for non-Hodgkin lymphoma (NHL) typically involves visual interpretation of scans of cancer tumours. Researchers have found that measuring a quantitative index – one that reflects the reduction of metabolic activity after chemotherapy first begins – adds accurate information about patients’ responses to first-line chemotherapy,
‘We demonstrated that a quantitative assessment of therapeutic response for patients with diffuse large B-cell lymphoma (DLBCL) is more accurate than visual analysis alone when using the radiotracer FDG (fluorodeoxyglucose) with PET scans,’ said Michel Meignan, professor of nuclear medicine at Henri Mondor Hospital. in Creteil, France. ‘The ability to predict tumour response early in the course of treatment is very valuable clinically, allowing intensification of treatment in those patients who are unlikely to response to first-line chemotherapy,’ he added. ‘Similarly, treatment could possibly be shortened in those patients who show a favourable response after one or two cycles of chemotherapy, and quantification also may help identify the disease’s transformation from low-grade to aggressive stage. ‘However, visual interpretation of PET scans will always be the first step of analysis and will prevail in case of difficulties to quantify images.’
Diffuse large B-cell lymphoma is a fast-growing, aggressive form of non-Hodgkin lymphoma, a cancer of the body’s lymphatic system. Although there are more than 20 types of NHL, DLBCL is the most common type, making up about 30% of all lymphomas.
Ninety-two patients with DLBCL were studied before and after two cycles of chemotherapy, and tumour response was assessed visually and by various quantitative parameters, explained the co-author of Early 18F-FDG PET for Prediction of Prognosis in Patients With DLBCL: SUV-Based Assessment Versus Visual Analysis. ‘We found that quantification of tumour FDG uptake (the ratio of tissue radioactivity concentration) can markedly improve the accuracy of FDG PET for prediction of patient outcome. Additional studies need to be done,’ Prof. Meignan said.
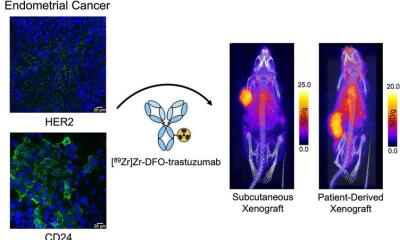
PET is a powerful molecular imaging procedure that uses very small amounts of radioactive materials that are targeted to specific organs, bones or tissues. When PET is used to image cancer, a radiopharmaceutical (such as FDG, which includes both a sugar and a radionuclide) is injected into a patient. Cancer cells metabolise sugar at higher rates than normal cells, and the radiopharmaceutical is drawn in higher amounts to cancerous areas. PET scans show where FDG is by tracking the gamma rays given off by the radionuclide tagging the drug and producing 3-D images of their distribution within the body. PET scanning provides information about the body’s chemistry, metabolic activity and body function.
15.11.2007