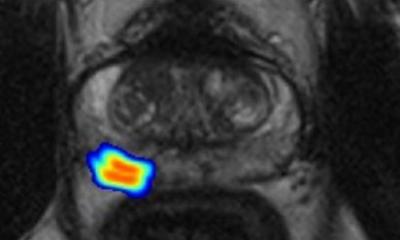
Multi-parametric MRI
Prostate MRI: “Yes, we scan!”
One in six men will develop prostate cancer. It is the second leading cause of cancer death amongst men in both the US and the EU. Definite diagnosis at an early stage is vital for survival and early treatment minimizes the risk of adverse effects, such as incontinence, erectile dysfunction, or impotence. While there is no preventive screening there is a ray of hope. Prof. Jelle Barentsz, Professor of Radiology and Head of the Prostate MRI Reference Centre of Radboud umc., and his team established new MRI techniques that can quickly confirm or dismiss suspected aggressive prostate cancer as well as accurately determine the aggressiveness of the disease and stage it.
Report: Sascha Keutel

Latest studies show that many patients with mild forms of prostate cancer (known as indolent carcinoma) seem to undergo excessive treatment, a consequence of inadequate staging prior to therapy with the commonly used diagnostic tools. This current diagnostic work-up has several disadvantages. Patients with an elevated prostate-specific antigen (PSA) levels usually undergo a transrectal ultrasound (TRUS)-guided biopsy which typically involves sampling of tissue from twelve (sometimes six or as many as 24) points in the prostate in accordance with an established pattern. However, the probability of detecting a carcinoma using this method is only about 50 percent, since ultrasound shows the prostate itself but often does not reveal the position of a carcinoma. In other words, many painful tests establish results that are often inaccurate creating stress and physical inconvenience for the patient without providing diagnostic safety.
Improved accuracy
Therefore leading urologists are calling for a non-invasive and reliable method to detect or rule out prostate carcinomas. MRI has been shown to be the most promising method. The new technology is known as mpMRI which stand for multi-parametric MRI – because it uses several parameters. mpMRI enables physicians to probe tissue parameters such as cellular density (with diffusion-weighted imaging) in addition to depicting the anatomical features and vascularity. It significantly improves accuracy of diagnosis and has the potential to save men pain, discomfort and infection. The latest clinical data suggest a sensitivity of more than 89 percent, which means that a patient with a negative MRI result does not need to undergo any further biopsy. Therefore it is currently the most reliable procedure available to confirm and stage a prostate carcinoma or to rule it out.
Economic viewpoint
However, there is a problem: This technique is not yet widely available. As it is considered very time consuming and demanding it tends to be restricted to centers of excellence. Due to the complexity of the images and the data volume that needs to be processed, evaluating the results is a very complex task for the treating physician, and the results are often difficult to interpret for the referring urologist. Barentsz disappointedly confirms: “Ignorance, legislation and cost accounting mean that a mpMRI is not the first option in the case of suspected prostate cancer.” Nonetheless the expert points out that even “From an economic viewpoint the new MRI techniques are also favourable: they clearly lower the costs of diagnosis and treatment throughout the entire course of care, and improve the quality of life.”
For example: SEEit, the new prostate MRI solution by Siemens makes this examination as comfortable as possible: powerful coil technology (Body 60 and Tim 4G) and unique applications (RESOLVE) allow a non-invasive examination in less than ten minutes.
Mr. Prostate’s dream
Barentsz, who has often been called ‘Mr. Prostate’, advocates for the future a general screening program for men above a certain age: “If this is done for breast cancer which afflicts 1 in 7 women, then why isn’t it done for prostate cancer, where 1 in 6 men is affected? Why don’t we have a ‘mannography’ yet?” MRI scans could radically change the diagnosis and treatment of prostate cancer and halve the number of unnecessary biopsies. “My dream is that MRI screening becomes standard practice if somebody comes to their GP with an elevated PSA level.”
However, the introduction of new medical services always depends on decisions by the national healthcare authorities. Barentsz has a clear opinion about the use of prostate MRI: “I hope that we – government, health insurers, specialists, GPs and patients – will increasingly be able to work together to give men with suspected prostate cancer the benefits of a modern MRI scan. Yes we scan!”
PROFILE:
Prof. Jelle Barentsz is Professor of Radiology and Head the Prostate MRI Reference Centre of the Radiology and Nuclear Medicine of the Radboud umc. He received his medical degree from Utrecht University in 1980 and his doctorate in 1990 for his research on MRI of the bladder. As an internationally recognized expert and renowned speaker he has been awarded many international prizes, inter alia in 2008 the Koningin Wilhelmina Research Prize: an award of 2 million euros for his research into using MRI for the diagnosis and treatment of prostate cancer, and he has recently been Knighted for the societal impact of his work.
30.07.2015