Image source: Adobe Stock/blueringmedia
News • Guidance about maximal cytoreductive surgery
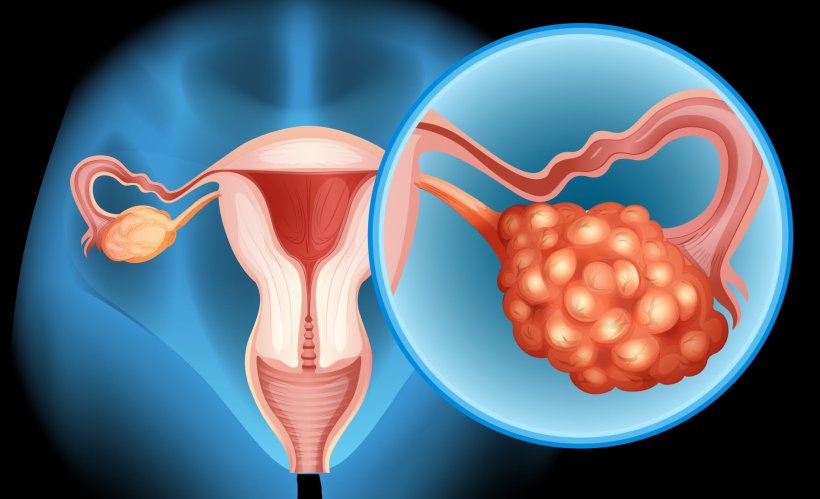
Ovarian cancer: new recommendations for safer surgery
Patients with advanced ovarian cancer are now being recommended surgery that University of Birmingham researchers have found leads to better outcomes.
The National Institute of Clinical Excellence (NICE) have published new guidance about the use of maximal cytoreductive surgery following a consultation on evidence including research from Professor Sudha Sundar and colleagues from the University’s Institute of Cancer and Genomic Sciences for the SOCQER-2 trial published in BJOG: an International Journal of Obstetrics & Gynaecology and Cancers.
Among the key pieces of research consulted on, Professor Sundar’s research conducted between the Institutes of Cancer and Genomic Sciences and Applied Health Research showed that women treated in centres where this kind of surgery is routinely conducted (which involves operating on a number of organs and can include removal of part of the breathing muscle and bowel) had six months increased overall survival rates compared to those that only conducted less extensive surgery.
This major surgery to fully remove all traces of cancer, despite the seemingly high levels of impact on women’s lives afterwards, made a significant difference to their quality of life as well as increasing survival time after surgery
Sudha Sundar
Put differently, women with late-stage ovarian cancer treated at centres that routinely conduct maximal cytoreduction surgery have a 20% reduction in their chance of dying from ovarian cancer. The research further found that quality of life in women was the same after 12 months regardless of whether women underwent maximal cytoreductive surgery or less extensive surgery.
Sudha Sundar, Professor of Gynaecological Cancer at the University of Birmingham, commented: “Ovarian cancer is a huge burden affecting women across the UK. Anything that improves survival rates and quality of life for women is significant. Increasing the time that women can spend with those they love after a late-stage diagnosis has a profoundly positive impact and is something that I am immensely proud to have contributed to. The SOCQER-2 trial has shown that this major surgery to fully remove all traces of cancer, despite the seemingly high levels of impact on women’s lives afterwards, made a significant difference to their quality of life as well as increasing survival time after surgery.”
Source: University of Birmingham
11.04.2023