Image Source: Possover
Article • Neuropelveology
Forging links between neurology and surgery
Surgery in the lower pelvic region often involves injury to or severing of nerve tissue. As in chronic diseases of the nervous system, the result can be pain, sensory disturbances or loss of function.
Interview: Meike Lerner
Up to now the poor view of the nerves, partially formed of fine interwoven networks, has been one of the major problems – exacerbated by the strict division of skills between neurologists and surgeons, which has not facilitated a holistic way of thinking. Professor Marc Possover, senior consultant at the Gynaecology and Obstetrics Clinic of St. Elisabeth Hospital Cologne-Hohenlind, Germany, has addressed this problem and founded a new discipline, which he calls neuropelveology and has patented. This field has already produced incredible and groundbreaking results for patients. In our Interview, Prof. Possover explained new procedures that have developed in the context of neuropelveology, such as laparoscopic neuronavigation (LANN) and the possibilities of implanting neuroprostheses.
As the pioneer of neuropelveology, would you outline what this field includes?

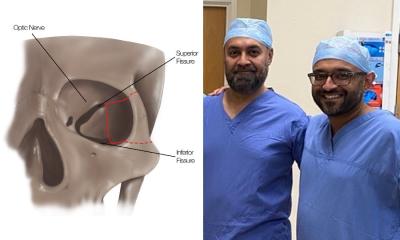
Prof. Possover: Neuropelveology pools the expert know-how of surgery and the expert knowledge of neurology. The true pelvis is a region that concerns many specialists: surgeons, urologists, gynaecologists, vascular surgeons; they all operate in this region, which is difficult to access, but they have only slight knowledge of the nerves encountered there - with dire consequences, for the nerve plexus transmits very important information including pain impulses, sexual activity and how full the bladder or rectum is. About 20%-40% of women patients suffer from bladder voiding disorders after radical removal of the uterus as a consequence of a tumour.
‘There is therefore a need to deal with this. First, the nerve plexus has to be made generally visible, because in conventional surgical procedures via laparotomy it is concealed from the surgeon. This can be done by laparoscopy, in which the nerves are magnified fivefold – you can then see even tiny nerves of a millimetre or so in size. Furthermore, the whole procedure can be performed by keyhole surgery with a maximum of three incisions near the navel.’
How do you find out the function of the nerve you have exposed?
‘Neuropelveology uses a technique called laparoscopic neuronavigation (LANN). The nerve seen is subjected to an electrical impulse and the reaction assessed. If, for example, it is the sacral root S2, which in humans is responsible for, among other things, erection, the penis will erect. With a nerve leading to the rectum, the large intestine contracts when stimulated. This technique proved its worth in neurosurgery quite a long time ago. However, neurosurgery is concerned only with the spinal cord and brain, and less with the true pelvis. Consequently, a few years ago, I was the first person to use the method in this region. First of all it led to being able to reduce complications occurring even in radical operations, such as hysterectomy, for example, where it reduced the likelihood of bladder voiding disorders from forty percent to not quite one percent. Clearly you damage nerves less if you can see them.
Thanks to LION, nerves can not only be blocked but also stimulated, and that is really a medical breakthrough, since it means that functions lost owing to multiple sclerosis or paraplegia can be restored
Marc Possover
‘But considerably more is possible. In laparoscopic implantation of neuroprostheses (LION), a procedure I developed, selected nerves are fitted with an electrode. The function of nerves can then be selectively influenced and striking effects obtained: in pain therapy, for example, an electrode, combined with a pacemaker, is connected by laparoscopic implantation to the nerve and the latter is then “turned off” with regular electrical impulses. In treating phantom pain in a patient whose leg had been amputated, I thus blocked the sciatic nerve and consequently eliminated the pain. This patient can now live without analgesics. I also use this procedure for pain therapy in polyneuropathy. Around six million people in Germany suffer from polyneuropathy, about two million of them due to diabetes. Patients are virtually free of pain after implantation, and that increases quality of life enormously for those affected.
‘Thanks to LION, nerves can not only be blocked but also stimulated, and that is really a medical breakthrough, since it means that functions lost owing to multiple sclerosis or paraplegia can be restored. Neuroprostheses in these cases force physical function, so to speak. I performed the first operation of this kind in February 2006 at St. Elisabeth Hospital Cologne-Hohenlind: and now the muscles concerned with closure of the bladder and rectum contract at the press of a button. The patient, a woman, controls voiding with a remote control; she is no longer incontinent nor does she need a catheter. In men I have not only been able to restore bladder and rectal voiding but also erection and ejaculation.
‘I have operated in China on children with open spina bifida. Many of these children die before the age of fifteen of the consequences of chronic urine retention. In one young female patient I exposed the sacral root and inserted electrodes and cables. The girl controls her body functions by selecting different programmes on a kind of remote control, which is connected to the stimulator: programme one for voiding the bladder and program two for voiding the rectum. Neurosurgeons obtain similar results by putting electrodes on the spinal cord, a complicated and risky procedure that, in the meantime, has been forbidden in the USA. The patient runs the risk of dying if inflammation arises. By contrast, in LION, the stimulator and the cable are placed in the pelvis, so that inflammation from bedsores, or external injuries, are excluded.'
Recommended article
Article • Neuro-research
Brain-computer interfaces: Getting a Grasp on how we think
A world where machines can be controlled by thought alone – such is the promise of so-called brain-computer interfaces (BCI). BCIs are both hardware and software communication systems that read brain and nerve signals, convert those into electrical signals and translate human thoughts into machine commands. Developers of BCIs rely on artificial intelligence, neural network models and big data…
How widespread has this revolutionary method become?
‘At present I am training gynaecologists in exposing the nerve pathways in the true pelvis, in order to make it possible to conserve the nerves in future operations. The technique could become established as an additional training module for neurosurgeons. My work met with considerable recognition at several neurosurgery congresses; the procedure has been recognised in the meantime by the FDA, which is why I am optimistic that in the medium term it will become more widely known in Europe.'
What are your future objectives with laparoscopic implantation of neuroprostheses?
‘Presently the procedures are still aiming to achieve control of bladder and rectal function, erection and ejaculation. I work with French researchers from the CNRS (French national scientific research centre) and INRIA (French national institute for research in computer science and control) who are currently developing wireless electrodes, which I shall use in the future. With the electrodes used hitherto there are still defects caused by the cables breaking.
‘However, far and away the most significant project is the exploration and stimulation of the nerves responsible for moving the legs. With colleagues in surgery I’m working on influencing standing up, standing and moving the legs. I have already performed the first implantation in a paraplegic patient. This patient is now able to move his left leg by stimulation. Now if several neuroprostheses were connected to the appropriate nerves and the latter were stimulated remotely by computer, in the future this procedure could make it possible for paraplegics to walk. That’s still a dream but one that might become reality one day.'
30.10.2007