MPR 3-D echocardiography
Mark Nicholls reports
A cardiologist at a UK hospital has become the first in the world to develop a technique to ‘slice’ 3-D images of the heart into intricate sections using computer software. The method, devised by consultant congenital cardiologist Dr Joseph Vettukattil at Southampton General Hospital, is known as multiplane review (MPR) 3-D echocardiography. This allows cardiologists to identify heart defects more accurately than on traditional 2-D or standard 3-D scans.

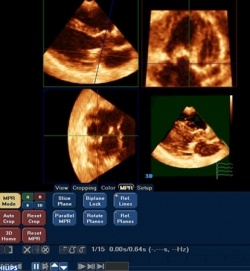
‘The most important aspect is the operator’s ability to slice the dynamic cardiac structures in infinite sections through all the three dimensions, which was not possible before we developed MPR 3-D echocardiography,’ Dr Vettukattil explained.
The hope is that the technology, which, for the first time, lets the user see the three dimensions of the heart move simultaneously, could eventually replace the need for magnetic resonance imaging (MRI) for most aspects of cardiac imaging.
Dr Vettukattil said the technique enabled cardiologists to see what was wrong and exactly where it was wrong on the screen. ‘By using MPR, because you are slicing and seeing it in three different planes, you can get a clear understanding of a patient – especially in a child whose heart is congenitally malformed.’
Traditionally, diagnosis of heart defects has been made using 2-D scans with the addition of invasive cardiac catheterisation. ‘The 2-D images show pictures of the heart in two planes, so it just takes one slice of the heart and, because it has not been easy to know without doubt what the problem is, surgeons have often had to perform exploratory operations as well,’ he said. ‘Now, though, we are able to visualise even more than a surgeon can during an operation, minimising the need for additional and invasive assessments.’
The system also enables cardiologists to compare the anatomy before and after surgery. ‘The main benefit is in delineating the anatomic details before surgery in complex cases,’ he pointed out. ‘This helps in better decision making and a better surgical approach and it has helped to find certain conditions that were not possible to define without opening up the heart.’
For the patient it means that more often the most appropriate surgical procedure is carried out and for the hospital it can have cost benefits in reducing the number of other investigations, such as cardiac MRI or catheterisation. ‘It potentially could reduce the hospital stay by identification and early and appropriate re-interventions,’ Dr Vettukattil added.
The 3-D MPR is not specific for detecting a particular defect, he pointed out, but a tool that helps cardiologists to understand the cardiac anatomy and pathology better and the method has been most helpful in detecting valve abnormalities and complex congenital heart defects.
Dr Vettukattil made the discovery after an upgrade from conventional 2-D imaging on echo machines in the children’s heart unit at his hospital. He set up two PCs with 3-D software programmes to read results from the echo scans and developed MPR from that.
A next step in the technique’s development is to further software modifications and improve image resolution, along with developing tools to visualise the 3-D images on a 3-D screen.
Dr Vettukattil said that remote uploading and data analysis of images should be possible soon via the internet and he has set up a website (www.3dechocardiography.com) to discuss and teach related topics.
He has also taught the use of MPR in countries such as Germany, Denmark and Sweden and aims to help develop Southampton University Hospitals NHS Trust as a world leader in advanced 3-D echocardiography through the establishment of an imaging and training centre.
‘The success of our work has led to 3-D echocardiography moving from a research tool to a clinical tool, with bi-weekly clinics and ward echograms performed in Southampton,’ he said. ‘We are also seeing increased numbers of patients referred for 3-D assessment and are determined to push forward our vision.’
06.11.2010




