Article • Radiographers in Spain report
Equipment hygiene: taking back center stage during the COVID-19 pandemic
The COVID-19 pandemic is putting extra pressure on radiology services. Radiographers are particularly at risk of catching and spreading the disease.
Report: Mélisande Rouger

This is why they must follow strict cleaning and disinfection protocols, according to Pablo Valdés Solís, President of the Spanish Society of Radiology (SERAM), who has just published new guidelines on how to protect staff and patients (PDF; 250kb, in Spanish), as the number of infected breaches the 100,000 threshold. Radiographers are key to help identify patients who have been potentially infected with the coronavirus disease and make sure everyone else remains safe. Ever since the first cases were reported in January, the radiology workflow has changed entirely. The focus has been shed on an essential yet not visible part of the department’s work: equipment hygiene.
“Increasing awareness on how to clean and disinfect devices adequately is crucial not only to protect our staff, but also not to spread the disease to our patients and colleagues during radiology examinations,” Valdés said.
The SERAM has just published guidelines to help radiographers keep staff and patients safe during the pandemic, as the Spanish radiographer training doesn’t include the necessary microbiology background to understand how the disease spreads. “Radiographers don’t receive that much training in virology. But if you understand what the disease is and how it spreads, you will better understand what needs to be done,” Valdés said.
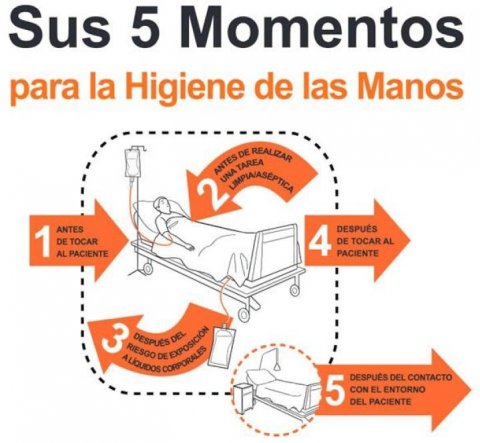
The graph shows the 5 moments for hand hygiene, which are recommended by hygiene experts around the world; hands should be cleaned:
- before touching a patient,
- before clean/aseptic procedures,
- after body fluid exposure/risk,
- after touching a patient, and.
- after touching patient surroundings.
The document reviews the basic concepts of the COVID-19 coronavirus and suggests a detailed list of measures that must be taken in radiology departments to prevent its spread during radiological examinations. The virus can survive as long as three days on stainless steel and plastic. Staff must therefore not only wash their hands before, during and after the examination (see graph on left side), but also clean and disinfect all the equipment they have used with a patient.
Keeping the equipment intact means that all the surfaces that are going to be in direct contact with the patient should be covered as much as possible with impermeable material that can be thrown after each examination. For example, in portable x-ray, radiographers should cover the shell with a plastic bag. In ultrasound, it is preferable to use a sleeve to cover the probe, but not absolutely necessary if the patient’s skin is clean. “If you have sleeves, you should cover the equipment and especially the console area, to facilitate posterior disinfection and minimize damage risk to the equipment,” Solís said. The equipment can be washed directly with soap and water or specific cleansers. Powerful cleansers, organic disinfectants, alcohol and dissolvent should never be used as they may damage the surface.
Disinfection is another key step of the cleaning routine, especially during the pandemic. The aim is to diminish the microorganism load, assuming that some will remain in non-threatening levels. Disinfection can be classified into three levels.
- The so-called low level is the elimination of bacteria, fungus and some viruses by applying the product in the examination room and on the equipment surface for less than ten minutes.
- Intermediate-level disinfection consists in eliminating TB bacillus and most of the existing bacteria, viruses and fungus.
- High-level disinfection is the complete elimination of germs - except bacterial spores - and is traditionally used to decontaminate medical devices such as endoscopes, anesthetic material and other medical devices that have been in touch with the patient’s mucosa.
Sterilization will eliminate all microorganisms including bacterial spores from any surface in critical material like endocavity probes, surgical material and non-reusable interventional material.
The coronavirus is covered by a lipid layer and is therefore vulnerable to soap and traditional disinfectants. For most medical equipment that is used in daily routine, low to intermediate disinfection is enough. Special products are not necessary and the disinfectant solution can be applied for five minutes. For example, a solution made of 0.1% sodium hypochlorite (bleach), 62-71% ethanol or 0.5% hydrogene peroxyde can inactivate the virus in just a minute. The solution should not be applied directly though, but using a gauze, compress or cloth that has been previously soaked. In addition, the surface that will be in contact with the patient should be completely dry.
Besides equipment, the examination room must also be cleansed and disinfected, and proper coordination must be carried out with the cleaning workforce to make sure the room is available as soon as possible.
Different areas, different protocols
Hospitals across Spain are affected differently depending on the local incidence of COVID-19. La Paz and Ramón y Cajal hospitals, two major hospitals in the Spanish capital, now mainly treat COVID-19 and derive other patients to nearby hospitals. Hotels in the hospitals’ neighborhoods have also been requisitioned and new hospitals created. Madrid conference’s center IFEMA, which hosts countless art fairs and trade conventions, has now become Spain’s largest hospital with 5,500 beds. Madrid Hospitals (MH) are tending to about 900 patients with COVID-19, 110 in intensive care units (ICU) and 100 in floors with reservoirs - i.e. systems that facilitate oxygenation. “This is wartime medical care,” Valdés said.
Infectious diseases are traditionally the concern of clinicians, but this pandemic has reminded us of how important hygiene is and that we all have a role to play
Pablo Valdés Solís
Things are quieter at Costa del Sol Hospital, a medium sized institution in Marbella that tends to nearly half a million patients. Although he is not at liberty to communicate patient data, Valdés admits that things are starting to heat up this week. “We’ve been preparing for this for over a month and are now expecting the big part,” he said. According to the Spanish Ministry of Health, Andalusia registered 6,392 infected patients, 260 of whom in the ICU as of April 1. To this day, 29,840 patients have been infected and 1,514 are in the ICU in Madrid, while in Murcia, one of the least affected regions so far, 1,041 patients have been infected and 59 are in the ICU. Because of these differences, hospitals must decide themselves what hygiene protocols they need to follow. “We recommend establishing these rules together with the local preventive medicine experts. Taking care of the examination rooms and materials starts by adequate cleaning, according to the hospital policy,” Valdés said.
Also important to bear in mind are the protocols recommended by equipment manufacturers, as some devices or components may be more sensitive, for instance ultrasound probes and some areas in CT gantries.
Recommended article

Article • The math behind corona
Predicting the future of the Covid-19 pandemic with data
Mathematical models can help shed light on the evolution of the coronavirus pandemic, according to Spanish mathematician Juan Luis Fernández Martínez, who predicted Spain could have between 90,000 and 160,000 infected patients. The next trend in epidemic data science will be to issue prediction models that focus on early detection.
Unexpected positive consequences
Radiology is learning a few lessons from the pandemic, the head of Spanish radiology explained. “We’ve regained an excellent habit, which is to report on simple x-ray examinations. This is really something we need to value more. Being able to study simple radiology is extremely important,” he said.
Keeping the equipment clean has also taken back center stage. “Radiation and magnetic resonance safety have long been the focus of our preoccupations, but it’s very important to take care of the material as well. Infectious diseases are traditionally the concern of clinicians, but this pandemic has reminded us of how important hygiene is and that we all have a role to play,” he concluded.
Profile:
Pablo Valdés Solís is Area Director of Costa del Sol Healthcare Agency in Marbella, Malaga, Spain and the current President of the Spanish Society of Radiology (SERAM). He has over 25 years professional experience and has a special interest in pediatric radiology and emergency radiology. For the past fifteen years he has been focused on management and quality.
02.04.2020