Emergency radiology
The ECR formally recognises ESR as a sub-specialty
The injury was as spectacular as it was ruesome. Struck by a train a male patient was brought to the emergency department in Munich, his right foot hanging on only by muscle and bloody tendons, the bone shattered.
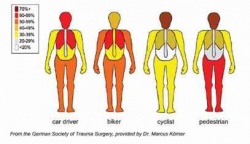
Surgeons quickly prepared the patient for an urgent operation to re-attach the foot. Yet, this was not the real danger to the patient’s life. Because the accident victim had a whole body CT scan as a matter of routine at the Ludwig Maximilians University (LMU) hospital the radiologists could show surgeons a more lifethreatening spinal injury that needed to be addressed first. That was the dramatic introduction by Marcus Körner MD, from the Department of Clinical Radiology at LMU, to demonstrate the increasing value of medical
imaging for emergency doctors during a State of the Art Symposium entitled Polytrauma in the Golden Hour, during the European Congress of Radiology 2012.
This year, the European Society of Radiology (ESR) formally recognised emergency radiology as a sub- specialty, putting its full support behind this critical practice area with a scientific subcommittee to encourage specialised research. The European Society of Emergency Radiologists was officially founded in October 2011 and is now planning its first congress, to be held this summer in Munich.
The chairman for the ECR Symposium Ulrich Linsenmaier MD, also from LMU, described an explosive rise is the use of computed tomography (CT) among patients presenting at the emergency department of hospitals. CT use is doubling every five years due o its ability to rapidly reveal the extent of injury or hidden causes of symptomatic pain. ‘Time makes a difference in emergency and establishing the correct diagnosis as soon as possible is critical for the patient,’ Dr Linsenmaier said, adding that it also proves to be more cost-effective for a hospital. Results from a study of 9,689 patients proved conclusively that whole-body CT performed when the patient enters emergency significantly reduced mortality.
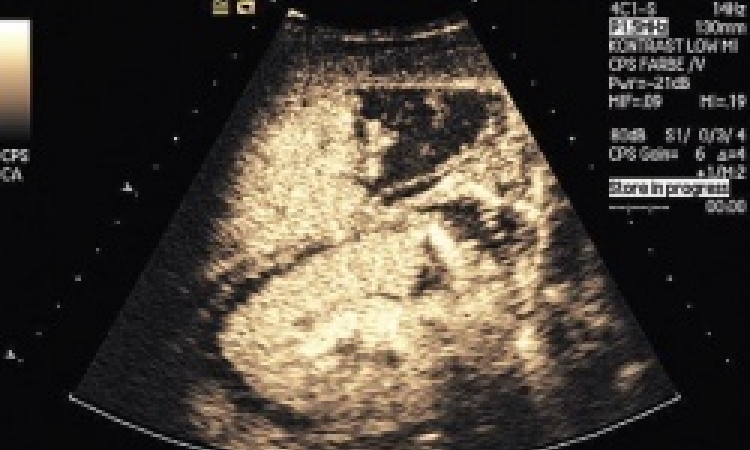
Dr Koerner showed how a rapid whole body scan, called a long-range scout view, provides an invaluable first look at the extent of a patient’s trauma. A study he presented found the whole body scan replaces conventional radiography by providing a sensitivity of 93% and a specificity of 84% for injuries, as well as a negative predicative value of 97%. Yet not all medical imaging performed in emergency is necessarily in the right hands, which is the motivation behind the effort to build a sub-specialty among radiologists in trauma. Along with CT, the use of ultrasound is also rapidly increasing in emergency, but where CT is clearly left in the hands of trained radiologists, emergency physicians and residents do not hesitate to perform ultrasound exams at the patient’s side, to the detriment of accurate diagnosis.
The widely used ultrasound exam for focused assessment with sonography for trauma, or FAST, is often regarded as being a simple extension of clinical examination routinely performed by emergency resident physicians in two minutes. The FAST scan seeks to quickly detect free intra-abdominal fluid or cardiac complications among patients with signs of haemorrhagic shock or suspicion of intra abdominal injury.
Pierre-Alexandre Poletti from Geneva reported studies showing that the FAST scan is better performed by more highly trained radiologists who can provide optimal results for better management of patients with polytrauma.
Free liquids of less than 400 millilitres in the abdomen, such as blood, as a result of blunt trauma, were found among unstable patients with a sensitivity of 98% by radiologists using FAST, compared to 42% by emergency residents.
According to ECR 2012 President Lorenzo Bonomo, recognition of the subspecialty of Emergency Radiology is a first step in a move to re-assert the role of radiologists in this critical area of medical practice. By John Brosky.
05.02.2012