Contrast enhanced ultrasound
In the USA, some patients have bled to death while in the CT scanner because this type of examination takes too long for blunt abdominal trauma diagnosis.
Report: Chrissanthi Nikolakudi

For this reason, internist Dr Josias Mattli, at Davos Hospital, Switzerland, introduced contrast enhanced ultrasound (CEUS) for initial traumatology diagnoses – setting the course for diagnosis even before patients undergo CT scans.
Mattli knows of no other institution where contrast enhanced ultrasound is carried out as a primary examination to the same extent as at Davos Hospital. ‘Since 2003, I’ve collected documentation on 470 such cases where no abdominal CT scan was carried out at all, but exclusively CEUS,’ he explained. The trauma surgeons only use the CT scanner as a follow-on examination for bone diagnosis.
Ultrasound is available everywhere, takes no longer than five minutes and involves no radiation exposure or side effects. ‘It’s a very fast diagnostic tool that can be used in the shock room while IVs are being started,’ he said. ‘This is a particular advantage for smaller hospitals, where often there isn’t a CT scanner available.’ For this reason, eight years ago Mattli also introduced CEUS as a complementary, Focused Assessment with Sonography for Trauma (FAST) ultrasound at the Santa Maria Hospital in Münstertal, Switzerland’s smallest hospital, and an hour away from the nearest CT scanner. Therefore, contrast enhanced ultrasound has become the primary traumatology scanning system to diagnose blunt abdominal trauma.
The right diagnosis in just five minutes
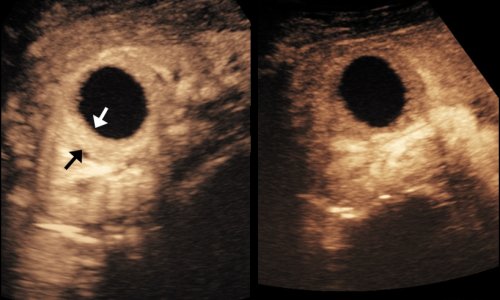
The most commonly injured organ is the spleen, followed by kidneys and then the liver. Most splenic injuries involve tears to the thin capsule and ruptures with or without injuries to the blood vessels. If the conventional ultrasound image suggests an abdominal trauma, perhaps due to the presence of some free fluid in the abdomen, the traumatologist can quickly escalate the examination to a CEUS scan. However, if an unstable patient is admitted with symptoms hinting at blunt abdominal trauma, such as injuries to the lower ribs or pelvis, CEUS takes an immediate role.
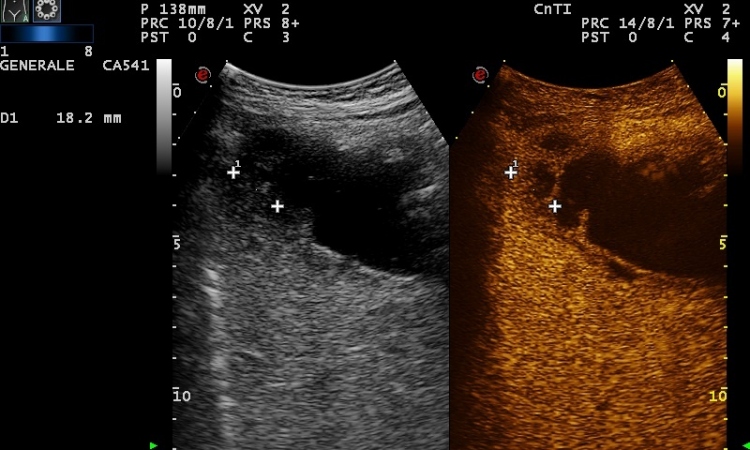
The diagnosis of a splenic injury takes less than a minute. ‘We inject the contrast medium and the microbubbles arrive in the blood after only ten seconds. We focus the image on the spleen and can usually see the tear very clearly. After three to five minutes, we will have examined the entire abdomen, inclusive of the kidneys and liver,’ Josias Mattli said. ‘It’s not only very fast but, above all, a reliable diagnosis.
‘Blunt abdominal trauma often occurs as a result of winter sports accidents,’ said Dr Mattli, naturally seeing cases frequently in the Davos ski area. ‘If the accident involved a fall on the back this tends to affect the kidneys, if the victim falls on their front it’s the liver that tends to be injured, and a fall to the side often results in a splenic rupture.’ Blunt abdominal trauma also often occurs as a result of road traffic accidents.
The examination procedure is particularly suitable for children because the radiation exposure associated with CT examinations can be avoided. However, very elderly patients and patients with renal insufficiency should also be examined with contrast enhanced ultrasound in the first instance. The procedure involves the injection of microbubbles the size of blood cells into the blood, which have a reflecting effect in the ultrasound scan image.
Following diagnosis, a rupture does not always have to be surgically repaired. ‘If the patient is stable and bleeding has stopped the patient can then be monitored in the intensive care unit, with regular follow-up ultrasound scans carried out in short intervals,’ Mattli explained.
In the case of splenic tears, the capsule begins to heal after five days. No other procedure can visualise the reinstated blood flow of the regenerated capsule. In most cases, the patient can thus be treated conservatively and does not have to undergo surgery. Out of 66 cases involving splenic ruptures at Davos Hospital only six patients needed surgery.
10.11.2014