Electrical impedance tomography
A new respiratory monitor visualises lung activity in real-time
This March, Dräger Medical will bring to the bedside of respiratory patients an innovative new monitor that vividly shows, breath-by-breath, their response to treatment. After shifting a patient’s position, or adjusting the respirator setting, or delivering a drug to open airways, physicians and nurses will be able to watch in real-time the response inside the patient’s lungs.
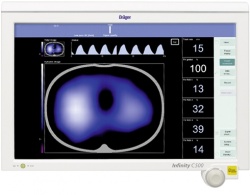
The images created by this novel technology, called electrical impedance tomography (EIT), are stunning. The cross section view of the patient’s lung on the new Dräger monitor looks like weather maps used on TV, with regions changing from dark blue to powder blue as warm air masses flow in. Where the lung remains closed to the passage of air, the region remains dark.
Gently move the patient and the change to lung capacity can be immediately seen on the monitor.
‘It’s a giant step forward in the handling of ventilator patients,’ according to Professor Ola Stenqvist at the Sahlgrenska University Hospital in Göteborg, Sweden, who over the past five years has conducted research using EIT. ‘This technology will bring a new clarity into handling patients with uneven lung disease,’ he added, providing continuous bedside monitoring of effective recruitment and indicating the optimum PEEP (positive end-expiratory pressure) settings on respirators.
EIT provides a functional image of breathing that is a complement to the structural images provided by computed tomography or chest X-rays.
Non-invasive, radiation free, and portable, the bedside EIT monitor means these fragile patient’s will not need to be transported as often to the radiology department to evaluate changes in their condition.
The video-like EIT images of the lung are constructed from data collected by16 pairs of electrodes on a belt that circles the patient’s thorax. The electrodes rest gently against the skin and no gel is required to enhance conductivity.
In sequence, each emitter on the r sends a low-energy electrical pulse, using the same voltage as an electrocardiogram, which is captured by the ring of detectors.
The impedance of the signal passing through body tissue is filtered, a complex challenge considering the number of cross currents of electricity in the human body, and more so for patients attached to ventilators.
By sequentially firing the emitters in a rotational pattern around the patient’s chest 208 data sets are collected to construct a single image. Up to 50 images can be acquired each second, creating the video motion that depicts the patient’s breathing patterns with the regional ventilation distribution and, significantly, the end-lung expiratory impedance that is a key indicator for physicians.
The image on the monitor is divided into four quadrants showing the left dorsal and left ventral, right dorsal and right ventral regions, and provides a quantification of variations in tidal volumes.
EIT has been used in research for 20 years, but Dräger is the first manufacturer to bring the technology successfully into routine clinical use.
The new model, which the company estimates is the fifth generation evolution of the EIT technology, was demonstrated for the first time at Medica in 2007.
Dräger has not released the name of the new EIT monitor that it previewed at Medica 2010, but told European Hospital that the final product will be introduced to hospitals at the end of March.
Anne-Catherine Grüntges, who heads the marketing efforts for Dräger Respiratory Care in Europe, told us: ‘People who have seen the EIT monitor have a hundred ideas right away about how and where they want to use it,’ and, she added, ‘The purpose is clear, yet the clinical potential is open to what clinicians will want to do with the technology. Now the question is how EIT will influence ventilation therapy practiced at the bedside.’
25.02.2011





